Pulseless electrical activity (PEA) is a condition where you don't have a pulse. Your heart stops, and you're in cardiac arrest. Without medical attention, your heart can't recover by itself. It's a potentially deadly condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
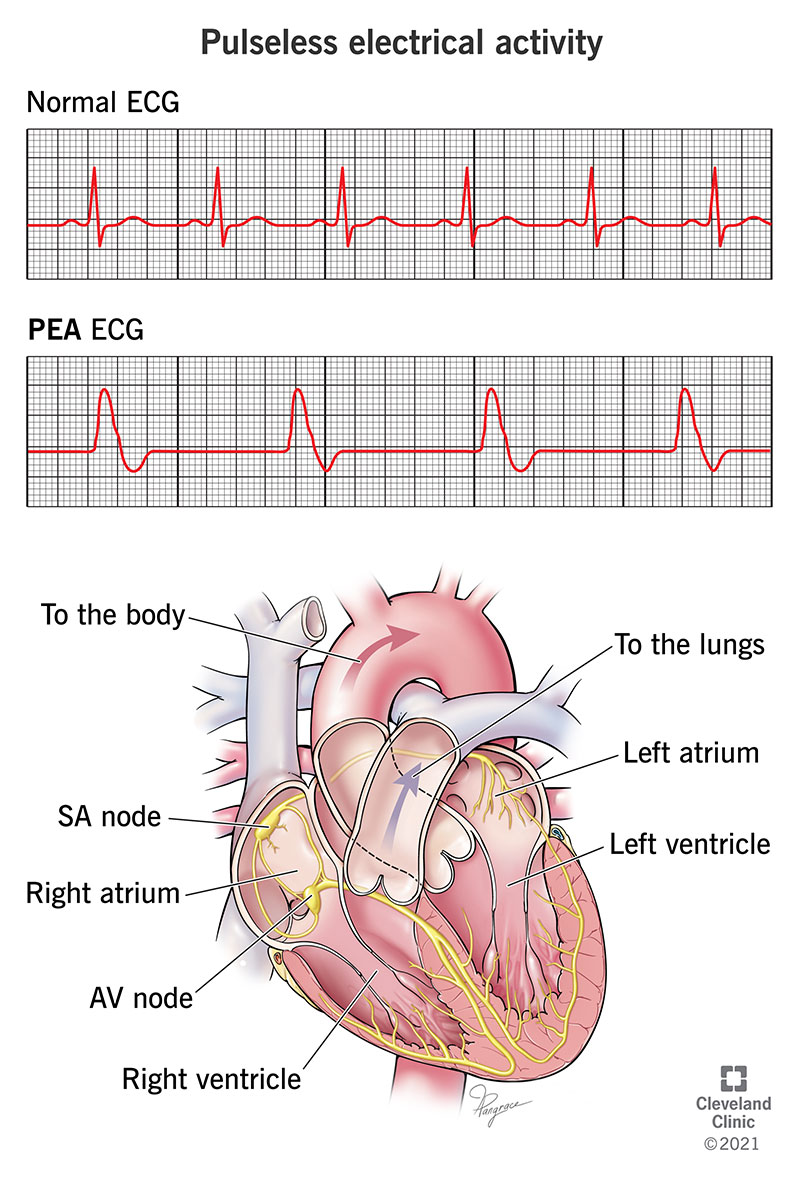
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23213-pulseless-electrical-activity)
Pulseless electrical activity (PEA) is a condition where your heart stops. The electrical activity in your heart doesn't generate a heartbeat. When your heart stops, you go into cardiac arrest, and you don’t have a pulse.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
PEA is a “nonshockable” heart rhythm, meaning a defibrillator won’t correct it. If not treated quickly, PEA causes sudden cardiac death within minutes.
At the beginning of every normal heartbeat, a cluster of cells (the sinoatrial node) near the top of your heart creates an electrical current, which then spreads to other areas of your heart. As the current passes through the heart muscle, the muscle reacts by flexing. That causes your heart to squeeze and pump blood.
That electrical current is detectable with a diagnostic test called an electrocardiogram (ECG or EKG). With PEA, your heart does have a detectable electrical current, but your heart isn’t strong enough to pump blood to the body.
PEA can take two different forms:
Time is critical. When someone's heart stops, call 911 and start CPR by performing chest compressions immediately to improve their chance of surviving.
Advertisement
PEA and asystole (also known as “flat-lining”) can lead to cardiac arrest. The difference is that with PEA, your heart still has some detectable electrical activity. With asystole, there’s no electrical activity to detect.
The causes of PEA fall into two distinct categories.
This happens because of a problem with your heart itself.
This is PEA from a distinct outside cause rather than from a problem with your heart itself. The most likely causes of secondary PEA are:
PEA occurs in about 20% of sudden heart-related deaths outside of hospitals. Inside hospitals, it accounts for about 10% of heart-related deaths.
The only way to know if a stopped heart involves PEA is with an electrocardiogram, which isn’t always available outside of a hospital setting. Fortunately, the treatment for cardiac arrest is always the same, regardless of whether or not PEA is involved.
Immediate, effective CPR, delivering chest compressions, should always be the top priority when cardiac arrest happens, especially outside of a hospital setting. CPR should continue until emergency services or first responders arrive.
If PEA happens inside a hospital, the following treatments are likely:
Certain malfunctions in your heart’s electrical system that create arrhythmias are “shockable.” That means defibrillation (an electric shock) can stop those rhythms by restoring your heart to a normal rhythm.
The cardiac arrests with shockable rhythms are ventricular fibrillation and pulseless ventricular tachycardia. Both of those can turn into PEA, but PEA itself isn’t shockable. However, CPR for pulseless electrical activity can sometimes get your heart to switch to a shockable rhythm. If that happens, then defibrillation can happen, which has a chance of restoring your heart to a normal rhythm.
Advertisement
PEA doesn’t happen predictably, and it’s a common part of the normal dying process. While it might be possible to revive someone who has PEA, this isn’t always possible, even if you begin CPR right away.
Cardiac arrest is always a medical emergency that needs immediate care. You should always call 911 (or the local emergency services number in your area) and start CPR. If you don’t know CPR, 911 operators can often instruct you over the phone on how to give CPR.
The main symptoms of cardiac arrest are:
Pulseless electrical activity is a type of cardiac arrest. Fortunately, modern medicine’s understanding of PEA and similar conditions has grown tremendously over the past few decades. However, the first few moments are especially critical. That means effective CPR and quick medical attention can make a big difference and improve the chances of survival.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart rhythm is out of sync, the experts at Cleveland Clinic can find out why. We offer personalized care for all types of arrhythmias.
