Spina bifida happens when a fetus’s spine doesn’t close completely during embryonic development. There are different types that range in severity. It can lead to symptoms like incontinence, loss of feeling and leg paralysis. Some babies need surgery after birth, and others may need ongoing care and support.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
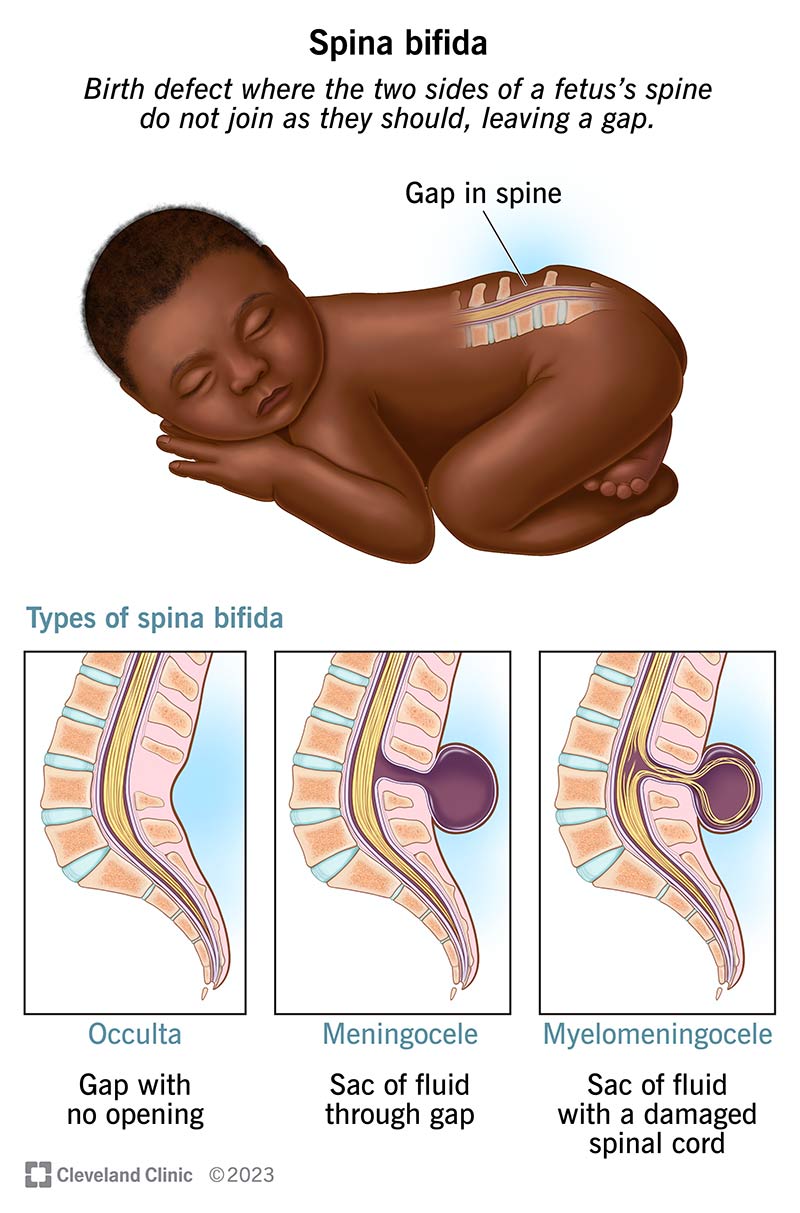
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/spina-bifida)
Spina bifida is a type of neural tube defect that happens when a fetus’s spine and spinal cord don’t close properly during early pregnancy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The neural tube forms the brain and spinal cord during embryonic development. When it doesn’t close, it leaves a gap in the spine. This gap can affect the vertebrae, spinal cord and nearby nerves. In more severe cases, a fluid-filled sac may stick out through the opening.
Symptoms range in severity. Your child may need surgery to repair the opening in their spine shortly after birth. In addition, treatment is available to help them manage symptoms throughout their lifetime.
Each year, about 1 in every 2,875 babies born in the U.S. has spina bifida. The exact cause of spina bifida isn’t known. But certain factors may increase the risk. There are ways to reduce the risk.
There are three main types of spina bifida:
Symptoms vary based on the type, size and location of the gap in your child’s spine. They may include:
Advertisement
If your child has a mild case, they may not notice any symptoms.
The exact cause isn’t fully understood. Experts believe a combination of genetic and environmental factors may interfere with how the neural tube develops in early pregnancy. When this process doesn’t go as expected, it can result in conditions like spina bifida.
Talk to your provider to learn more about whether or not you’re at risk of having a child with this condition. For example, your child may be at higher risk if you:
Your risk also increases if you have the condition or you’ve already had a child with a neural tube defect (genetics).
Your care team can help you manage these risks and have a healthy pregnancy.
Complications are more common with severe types and may include:
This condition may affect your child’s emotional health as they get older. Living with a chronic condition can be tough to manage day in and day out. They may find comfort in speaking with a mental health professional or joining a support group.
Adults who have spina bifida face different problems than children, including:
Women with spina bifida are able to get pregnant, but their condition can make pregnancy more complex.
Healthcare providers may make a diagnosis during pregnancy (prenatal diagnosis). They’ll use the following tests:
If the fetus has a myelomeningocele, your provider may recommend delivering your baby via C-section. This prevents injury to that area of your child’s spine.
To diagnose the condition in children, providers will offer imaging tests to get a better view of their spine and spinal cord. These tests include:
For mild cases where symptoms aren’t noticeable, you may not receive a diagnosis until adulthood. This could happen when you receive an imaging test of your spine for an unrelated reason and your provider notices a gap.
Advertisement
While there’s no cure for this condition, treatment options are available to manage symptoms. These may include:
A healthcare provider will customize your child’s treatment plan to fit their specific needs.
There are different types of surgery to close the gap in your child’s spine. For severe cases, like myelomeningocele, this can be done during pregnancy. But this is most often done during the first few days after your child is born.
If there’s a sac outside of your child’s spine, a surgeon will drain it, repair the opening and close the surgical site. Your child’s surgeon will meet with you before the procedure and tell you what you can expect.
In many cases, children experience a complication where their spinal cord attaches to their spinal canal (tethered spinal cord) instead of floating freely. Surgery treats this as well.
How this condition affects walking depends on where the gap is in your spine and how severe it is. If the gap is closer to your neck, walking independently may be difficult. If it’s lower near your hips, you may be able to walk with some assistance. In mild cases, it may not affect walking at all.
Advertisement
Mobility devices like braces, walkers or wheelchairs can help you move through daily life with more comfort and independence. Your care team will work with you to choose the right tools and teach you how to use them safely.
Your child will have several follow-up appointments with their surgeon after surgery. Your child’s surgeon will check the surgery site to be sure it’s healing well. They’ll also answer any questions you have about your child’s recovery.
This is in addition to regular wellness visits to see your child’s pediatrician to monitor their general health, growth and development.
Talk to your child’s care team about the frequency of visits that best support their needs.
Every child is different, and that’s especially true for a child with spina bifida. Here are some things to keep in mind as your child grows:
Advertisement
If your child has spina bifida, talk to their care team about what to expect. They can answer your questions and connect you with helpful resources.
Mild cases of spina bifida don’t affect life expectancy. But more severe forms may slightly shorten lifespan.
But life expectancy estimates are just that — an estimate based on other people’s experiences. If your child has spina bifida, ask their care team to explain if this condition could have an impact on their future.
You may be able to reduce your risk of having a child with spina bifida if you:
Like many other conditions, education about spina bifida and local support groups can be the greatest tools for managing the disorder and preventing further complications. These organizations will give you additional information on spina bifida:
Learning your newborn has spina bifida can turn a joyful moment into one filled with anxiety and uncertainty. You may suddenly have a million questions and not know where to begin. Your healthcare team understands how overwhelming this news can be. But you’re not alone. They’ll be by your side every step of the way to make sure you and your baby get the care you need.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.