Neural tube defects (NTDs) are birth defects of the brain, spine or spinal cord that happen in fetuses within the first month of pregnancy. NTDs are linked to folate deficiency before and during pregnancy. So, it’s important to make sure you’re getting enough folate and folic acid through your diet and supplements before and during pregnancy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
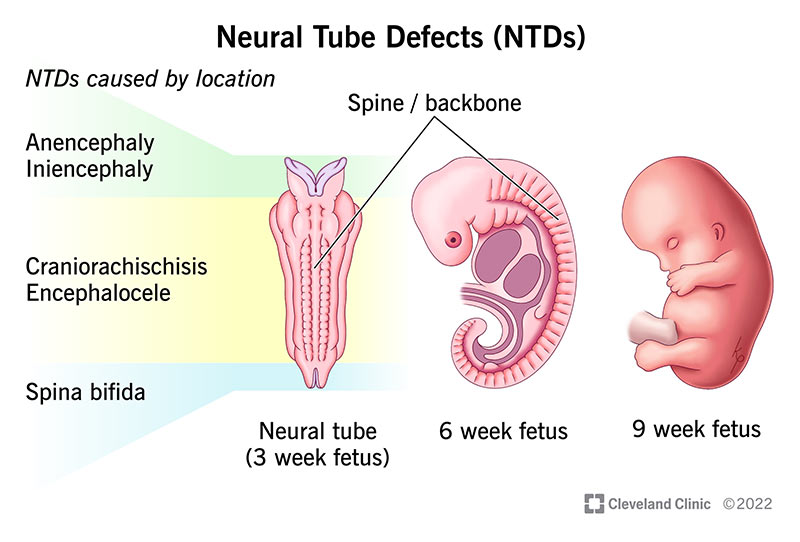
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22656-neural-tube-defects)
Neural tube defects (NTDs) are birth defects (congenital conditions) of the brain, spine or spinal cord. They happen to developing fetuses within the first month of pregnancy — often before you even know you’re pregnant. The two most common neural tube defects are spina bifida and anencephaly.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Normally, during your first month of pregnancy, the two sides of the fetus’s spine join together to cover and protect the spinal cord, spinal nerves and meninges. At this point, the developing brain and spine are called the neural tube.
As growth continues, the top of the neural tube becomes the brain. The rest of the tube becomes the spinal cord. An NTD happens when this tube doesn’t close completely somewhere along its length.
Neural tube defects affect about 3,000 pregnancies each year in the United States.
Types of neural tube defects include:
Spina bifida is the most common type of neural tube defect (NTD). It happens when the neural tube doesn’t close completely somewhere along the spine during fetal development.
Types of spina bifida include:
Advertisement
Anencephaly happens when the fetus’s neural tube doesn’t close at the top. This causes the skull, scalp and brain not to develop properly. Portions of the brain and skull are missing. The brain tissue that does form is usually exposed because there isn’t enough skin and bone to cover it.
Infants with anencephaly are either stillborn or die soon after birth.
Encephalocele happens when the neural tube doesn’t close near the brain. There’s also an opening in the skull. The fetus’s brain and the membranes that cover it can protrude through the skull, forming a sac-like bulge.
In some cases, there’s only a small opening in the nasal cavity or forehead area that’s not noticeable.
Iniencephaly happens when the spine is severely misshapen. It often causes a lack of a neck. The fetus’s head may be bent severely backward. The facial skin is connected to the chest. And the scalp is connected to the back.
Babies with iniencephaly are usually stillborn.
Each type of neural tube defect has different symptoms or features. But there’s no way to know you’re carrying a fetus with an NTD without medical tests, like an ultrasound.
If your healthcare provider suspects a neural tube defect, they’ll provide more information about what to expect. NTDs affect each baby differently.
Healthcare providers and scientists don’t know the exact cause of neural tube defects. But they believe it’s a complex combination of genetic, nutritional and environmental factors.
In particular, low levels of folate before and during early pregnancy appear to play a role.
Any woman can have a baby with an NTD. But certain factors increase the risk, including:
Advertisement
Some babies born with NTDs have no complications, while others have serious disabilities. Babies with iniencephaly and anencephaly are typically stillborn or die shortly after birth due to complications.
General complications of NTDs can include:
Healthcare providers typically diagnose NTDs during pregnancy through prenatal tests, like:
Advertisement
Healthcare providers also use imaging tests, like MRI or CT scans, to diagnose some NTDs after birth.
There are several treatment options for spina bifida and encephalocele, depending on the severity of the condition. Surgery is a common option for both.
Anencephaly and iniencephaly aren’t treatable. Infants with these conditions are typically stillborn or die shortly after birth.
Healthcare providers typically treat encephalocele with surgery to place the protruding part of your baby’s brain and the membranes covering it back into their skull. They then close the opening in your baby’s skull.
Treatment for myelomeningocele usually involves surgery to repair the opening in your baby’s spine. Surgeons can do this before birth (fetal surgery) or shortly after birth.
Long-term treatment for both conditions depends on your child’s case. They may need multiple surgeries over time. Or they may need other treatments related to complications, like a shunt to drain excess fluid surrounding their brain.
No two people with a neural tube defect, especially spina bifida and encephalocele, are affected in the same way. The best way you can prepare is to talk to healthcare providers who specialize in researching and treating these conditions.
Advertisement
If your child was born with an NTD, they’ll likely need to see their healthcare team regularly as they grow.
It’s not always possible to prevent NTDs. But there are several steps you can take to try to lower the risk.
One key way is to make sure you’re getting enough folate and folic acid. A folate deficiency before and during pregnancy increases the risk of having a baby with spina bifida and other NTDs.
Folate and folic acid are forms of vitamin B9. They support healthy cell growth and development, especially in early pregnancy. Folate occurs naturally in foods. It refers to all types of vitamin B9, including folic acid. Folic acid is a manufactured form of B9 found in supplements. It’s also added to certain foods.
The general recommendation is to take 400 micrograms (mcg) of folic acid per day if you’re at average risk of carrying a fetus with an NTD. If you’re at high risk, your healthcare provider may have you take more. Eating foods with folate is also important. These include dark leafy greens, legumes, citrus fruits, and nuts and seeds.
Other preventive steps include:
Learning that the fetus you’re carrying has a neural tube defect (NTD) can turn an exciting experience into one filled with anxiety and uncertainty. You may suddenly have a million questions and not know where to begin. But you’re not alone — many resources are available to help you and your family. Speaking with a healthcare provider who’s very familiar with NTDs can help you prepare.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
As your child grows, you need healthcare providers by your side to guide you through each step. Cleveland Clinic Children’s is there with care you can trust.
