Neurogenic shock is a serious complication of spinal cord injury that disrupts your blood flow and heart rate. It can lead to dangerously low blood pressure and reduced oxygen to vital organs. Fast emergency care is crucial, but with the right support, recovery is possible.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Neurogenic shock is a condition in which you have trouble keeping your heart rate, blood pressure and temperature stable because of damage to your nervous system after a spinal cord injury.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This is a serious condition that can be life-threatening. When nerves can’t tell your blood vessels to tighten, your blood pressure drops. With less pressure, blood flow slows, and your organs don’t get the oxygen and nutrients they need. Damage to your nerves can also slow your heart rate. This makes circulation worse.
Without enough blood flow, your organs may stop working. This could cause them to shut down. Fast care can protect your brain, heart and other organs.
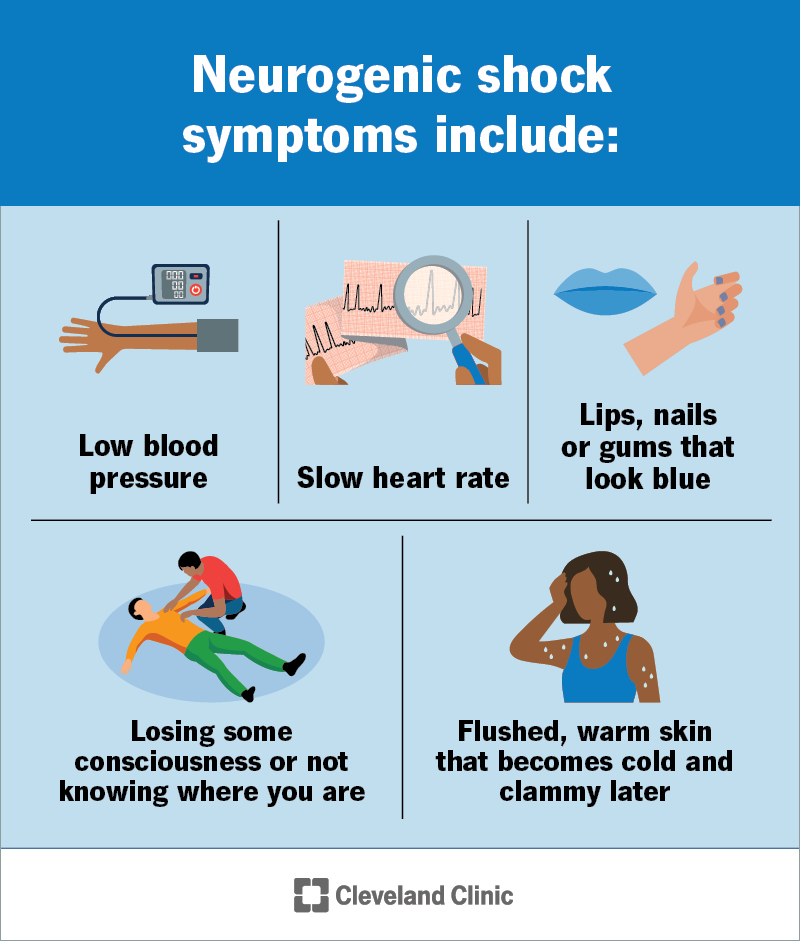
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/neurogenic-shock)
Recognizing symptoms quickly is important because this condition can become serious fast. Look out for the following:
Healthcare providers will make sure you’re safe and stable, especially after a spinal cord injury. Symptoms of the shock phase may last days to weeks. Ongoing symptoms usually come from the original injury.
A spinal cord injury is almost always the cause of neurogenic shock. Other causes could include:
Advertisement
Some of the complications can become serious and, in certain cases, even life-threatening if not treated quickly. That’s why close monitoring and timely medical care are so important after a spinal cord injury. Complications may include:
A healthcare provider will diagnose neurogenic shock with a physical exam and some tests.
Your provider will examine your body for signs of injury and damage. If you can, tell your provider what happened right before you noticed shock symptoms.
Your provider will need some tests, including:
These will show where you have spinal cord damage (and if you have other injuries).
The main goals of treatment are to restore your normal blood flow and heart rate. You may need:
Your healthcare provider will tell you how often you’ll need follow-up appointments after you start treatment. You might need more tests to make sure your heart rate and blood pressure stay at safe levels.
Tell your provider if you feel any new or changing symptoms, especially if your heart’s beating slower or faster than normal.
Call 911 (or your local emergency services number) if you think you have neurogenic shock.
Advertisement
After calling for help, you should lie on your back and prop your legs above the level of your heart. This can help increase your blood pressure while you wait for help to arrive.
Neurogenic shock can be a dangerous, sometimes fatal condition. Recovery can take time, especially if you had a spinal cord injury. What you can expect depends on a few factors, like:
A spinal cord injury can bring changes to how your body works. And you may need support as you adjust. Your care team might recommend physical therapy or occupational therapy while you recover.
Your provider will help you set realistic goals and expectations based on your unique circumstances.
While your body is physically recovering, this condition and its cause may also affect your emotional health. Ask your provider about support groups or rehabilitation programs that offer counseling, peer mentoring and caregiver education. Talking with a mental health professional can also help you process feelings of depression, anxiety or other challenges. Many people find strength and comfort in connecting with others who understand what they’re going through.
Advertisement
There are different types of shock that can happen after trauma or injury. Each one targets your body in a different way:
Neurogenic shock is a medical emergency, and it doesn’t leave much room for hesitation. Fast treatment can protect your vital organs.
Recovery may not follow a straight line, especially when it involves your nervous system. But with a clear plan, follow-up care and support from a medical team, many people are able to regain strength and move forward. Emotional healing is just as important, and there are resources to help with that, too.
You don’t have to do it all at once, just take it one step at a time.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Get the care you need today! At Cleveland Clinic, we offer specialty care that’s focused on you.
