A urethrocutaneous fistula is a rare condition in which an unwanted opening develops between your urethra and perineum. Symptoms include urinary incontinence and recurrent UTIs. It’s usually a surgical complication. But it may develop after an infection or injury, or it may be present at birth. Treatment usually involves surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
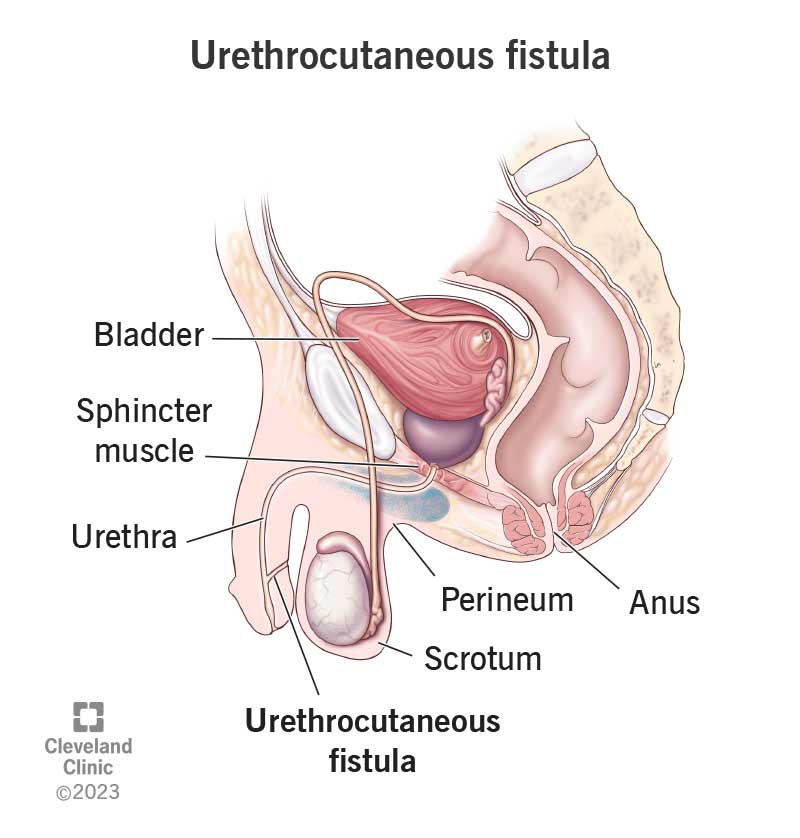
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/urethrocutaneous-fistula)
A urethrocutaneous fistula is an opening or tunnel between your urethra to anywhere along your genital skin and perineum. Your urethra is the tube that allows urine (pee) to leave your body. Your perineum is the thin layer of skin between your anus (butthole) and genitals (vaginal opening or scrotum).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When working as expected, your urethra and sphincter muscles control your pee flow. A urethrocutaneous fistula can bypass your urethra and sphincter muscles and cause pee to leak out of your body. It can also lead to urinary tract infections (UTIs). UTIs can damage your organs and tissues in the surrounding area.
Urethrocutaneous fistulas are rare. Sometimes, they’re congenital (present at birth), and other times, they develop after infection, injury or as a complication after surgery on or near your urethra.
Other names for a urethrocutaneous fistula include:
A urinary fistula is serious. It won’t heal on its own, and it requires surgery to treat it.
The most common symptoms of a urethral fistula include:
The most common cause of a urethrocutaneous fistula is a previous surgery, especially hypospadias repair. Other common causes include:
Advertisement
In rare cases, a urethrocutaneous fistula is present at birth or develops as a result of mismanaged diabetes (having an A1C greater than 8% for a year or more despite standard care).
Urethrocutaneous fistulas are rare. The greatest risk factor for a urethrocutaneous fistula is having a surgical procedure around your urethra, such as a hypospadias repair, urethroplasty or circumcision.
A healthcare provider might suspect a urethrocutaneous fistula if you have unexplained pee leakage or an unexplained infection in your urinary tract. There are several tests that a healthcare provider can order to check for a urethrocutaneous fistula. These include:
Surgery is usually necessary to treat a urethral fistula. But there are many variables a provider must consider before treating it, such as:
Smaller fistulas (less than 2 millimeters in size) are fairly easy to close. A provider will give you a sedative to help you relax, and then a surgeon will close the fistula with stitches.
Larger fistulas require a more involved procedure. If the skin around your fistula isn’t healthy, the surgeon may need to perform an approach that uses multiple layers of skin. They’ll use flaps of skin from other areas of your body to replace the unhealthy tissue and create a “waterproofing” layer to help seal off the opening.
Most people need to use a urinary catheter to help drain pee from their bladders while they heal after surgery. You may need to spend one night in the hospital after the procedure.
No, a urethral fistula can’t heal itself. Most people require surgery to close a urethral fistula. A healthcare provider who specializes in conditions that affect the urinary and reproductive systems (urologist) can treat a urethral fistula.
It’s important to remember that your body is unique, so recovery times may vary. In general, swelling and bruising after surgery to correct a urethrocutaneous fistula should go away after a few weeks. You should make a full recovery after about six weeks.
Advertisement
If you have a urethrocutaneous fistula, the overall outlook is good with treatment. One study found that the success rate for fistula repair is 89%. For people who still have symptoms after surgery, a follow-up surgery with a more complicated layered approach is very effective. You may need to wait at least six months after the first surgery before going through a second surgery to ensure complete healing in the area.
You can’t prevent all causes of urethrocutaneous fistulas. But you can help prevent injuries to the area by:
Schedule regular appointments with your healthcare provider after surgery to repair a urethrocutaneous fistula. They’ll want to ensure you’re healing properly. If you still have symptoms, they may schedule another surgery.
Go to the nearest emergency room if you have any of the following symptoms after surgery to repair a urethrocutaneous fistula:
Advertisement
It’s also a good idea to see a healthcare provider if your catheter comes out or if pee is leaking around your catheter.
You may want to ask your provider:
A urethrocutaneous fistula is an unwanted opening that develops between your urethra and perineum. It can cause embarrassing or frustrating problems like urinary incontinence or frequent urinary tract infections. But you don’t have to live with the complications of a urethrocutaneous fistula. Talk to a healthcare provider if you have symptoms. They can surgically close the opening, which should relieve your symptoms.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a condition that’s affecting your urinary system, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
