A hypothalamic hamartoma is a noncancerous growth on your hypothalamus. This is located deep in the base of your brain. It can cause early puberty, seizures, cognitive dysfunction and other symptoms. Medication and brain surgery are the most common treatments.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
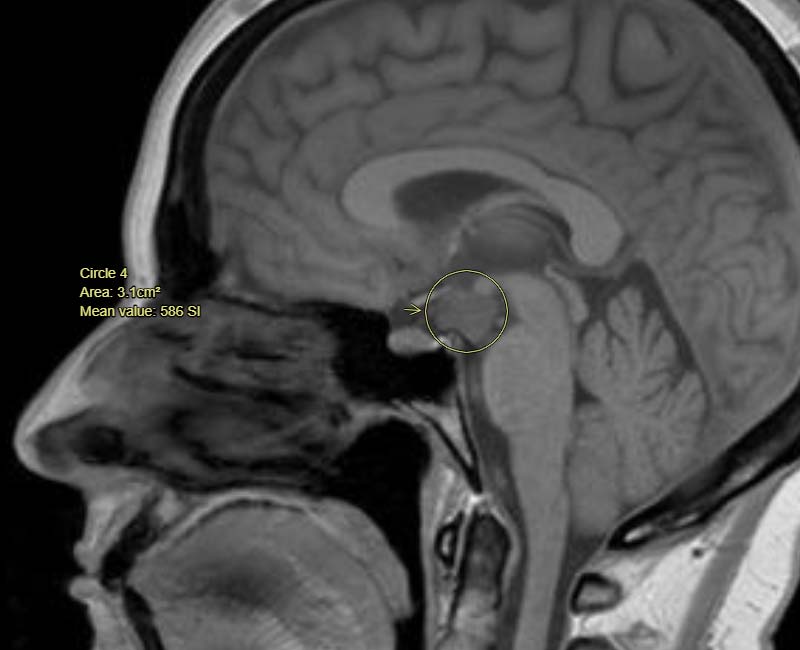
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17118-hypothalamic-hamartoma)
A hypothalamic hamartoma (HH) is a rare, present-at-birth growth on your hypothalamus. The hypothalamus is an almond-sized structure deep within your brain. It links your endocrine system and your nervous system to maintain homeostasis, or a state of balance, for your body systems to function as expected.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The growth is a noncancerous tumor. It can disrupt many important functions of the hypothalamus, including:
A hypothalamic hamartoma forms while a fetus develops. It grows as your brain grows. HH doesn’t spread to other parts of your brain or body. It usually involves one lesion, but in some cases, there are several.
Treatment options are available to manage symptoms of HH.
The symptoms of hypothalamic hamartoma vary for each person but may include:
Central precocious puberty happens when your brain releases sex hormones too soon. This typically happens before age 8 in girls and before age 9 in boys.
Physical signs for girls include:
Physical signs for boys include:
Seizures are common with this condition. One of the most frequent types is a gelastic seizure. This brief episode may only last a few seconds but can happen multiple times per day, even per hour in severe cases.
Advertisement
A gelastic seizure causes you to burst into an uncontrollable fit of laughter when there’s abnormal electrical activity happening in your brain. These seizures usually begin before your child’s first birthday. They reduce in frequency after age 10.
You may experience other seizure types like:
HH may affect your behavior, mood and cognitive function, including:
What are the types of hypothalamic hamartomas?
The two types of hypothalamic hamartomas are based on the location and the symptoms they cause:
It’s possible to have both types at the same time.
Experts don’t know exactly what causes HH and there’s no known way to prevent it. The majority of cases happen randomly. This means that they don’t usually run in your biological family history, so you likely won’t inherit it.
Recent studies of removed tumor tissue found a somatic variant within the tumor of the GLI3 gene. Other genetic variants have also been found in removed tumor tissue. Research is ongoing to learn more about the possible genetics involved.
There may be a link between hypothalamic hamartoma and a genetic condition called Pallister-Hall syndrome (PHS). This condition is the result of a genetic variant that can cause abnormalities in how your hands, feet, larynx (voice box) and anus develop.
Anyone can develop this condition. It’s slightly more common in males. HH primarily affects children and adolescents. But in some cases, you might not receive a diagnosis until symptoms appear in adulthood.
Early puberty can affect a child’s physical and mental health if their body is changing faster than their peers. It may result in short stature, for example. In addition, your child may not fully understand the changes that are taking place, which may affect their self-esteem and emotional well-being. Your child’s care team can help them manage any possible complications that may arise.
Advertisement
Your provider will offer imaging tests to diagnose HH. An MRI creates highly detailed images of your brain. Children usually need light sedation so they stay still during an MRI. If they move, the images might not be clear.
Your provider may also recommend an electroencephalogram (EEG) if you have seizures. This test monitors the electrical activity in your brain.
Neurological testing can measure the extent of cognitive problems, such as thinking, learning and remembering. Your provider may also recommend blood tests to check hormone levels. These tests may help guide treatment.
HH may be difficult to diagnose because symptoms may resemble other neurological conditions.
Treatment for HH may include:
Your child’s provider may recommend other treatment options like educational support in school and therapy or medications for different types of mood, behavioral and psychological disorders.
A provider may recommend epilepsy surgery or another procedure to remove or destroy the hamartoma and manage seizures. Antiseizure medications usually don’t work well to treat gelastic seizures but may help manage other seizure types.
Advertisement
Common procedure types may include:
The prognosis (outlook) is usually good for hypothalamic hamartoma because treatment options are effective at managing symptoms.
Surgery may reduce the frequency or severity of seizures. Some people are seizure-free after surgery. In some cases, surgically removing the hamartoma may cure the condition if it can be done safely. But there’s a risk that seizures may return.
Monthly injections of a drug that suppresses the release of certain hormones help keep early puberty symptoms in check. Your child’s provider may stop the medication when they reach the normal age for puberty to occur. Most children and teens have an expected puberty and sexual development at this time.
Advertisement
Your child’s provider can give you the best information on what you can expect for your situation.
A healthcare provider will let you know what your life expectancy may look like, as this can vary from person to person and depend on many factors, including:
There’s a risk of sudden unexpected death in epilepsy (SUDEP) with hypothalamic hamartomas. A provider will help you stay safe and create a treatment plan to manage seizures.
If you suspect something is wrong, you know your child best, so don’t hesitate to contact a healthcare provider. Look out for signs or symptoms that affect their behavior, cognitive function and hormone regulation, which may include:
If your child has HH, you may want to ask their provider:
It might be scary to learn that you have a tumor in your brain. Seizures are unpleasant and your body wants to kickstart puberty faster than you were expecting. This can be a lot to handle emotionally.
Fortunately, treatment is effective at managing hypothalamic hamartoma symptoms. You’ll get to know your care team well, as you’ll visit them regularly for treatment. They’ll make sure your symptoms don’t interrupt your physical or mental health. Surgery may reduce how often and how severe symptoms affect you, so talk to your provider to see if you’re a good candidate.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
