Arginine vasopressin disorders — formerly known as diabetes insipidus — are two rare and treatable conditions in which your body lets go of too much pee. They mainly happen due to an issue with how your body makes or uses arginine vasopressin, a hormone.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Arginine vasopressin disorder, formerly known as diabetes insipidus, represents two conditions that happen when your body lets go of too much urine (pee). It can’t keep (retain) water properly. These conditions are rare but treatable.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
An issue with arginine vasopressin (AVP) — a hormone — mainly causes these conditions:
Healthcare providers may also call AVP antidiuretic hormone (ADH). AVP plays a large role in helping your kidneys balance the amount of fluid in your body.
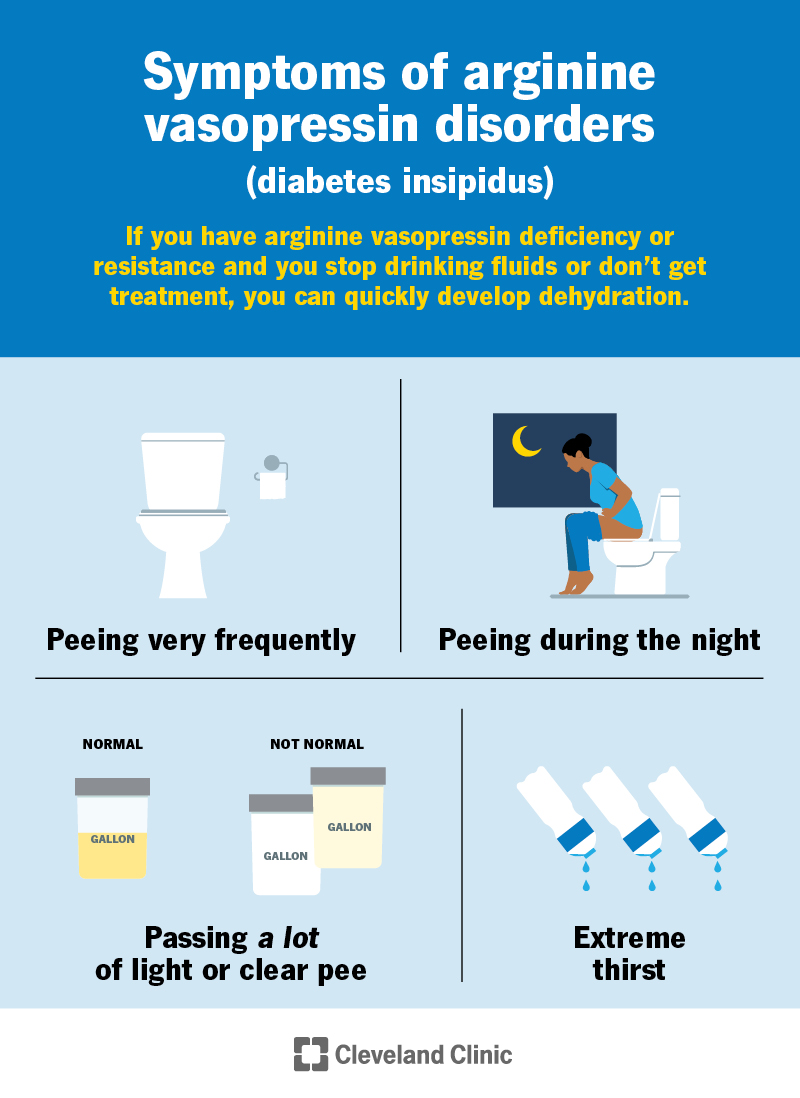
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/16618-diabetes-insipidus)
The main symptoms of arginine vasopressin deficiency and resistance include:
Most people make 1 to 3 quarts of pee a day. People with AVP-D or AVP-R can make up to 20 quarts of pee a day.
If you stop drinking fluids or don’t get treatment, you can quickly develop dehydration.
These symptoms are a significant sign that something in your body isn’t working as it should. It’s essential to get medical help as soon as possible.
Symptoms of arginine vasopressin deficiency or arginine vasopressin resistance in children may include:
The causes vary based on the type:
Advertisement
One other type is a rare pregnancy-related form known as gestational arginine vasopressin disorder (gAVP-d). During pregnancy, the placenta may make too much of an enzyme that breaks down AVP. You’re more likely to get gAVP-D if you:
gAVP-d usually goes away two to three weeks after the pregnancy is over.
AVP-D happens when there’s an issue with your hypothalamus or pituitary gland. Specific causes include:
Up to half of AVP-D cases have an unknown cause (idiopathic).
Specific causes of AVP-R include:
The main complication of arginine vasopressin disorders is dehydration. This happens when your body loses too much fluid and electrolytes to function as it’s meant to.
You can usually make up for all the fluids you pass in your pee by drinking more liquids. But if you don’t, you could quickly become dehydrated.
Dehydration can be life-threatening. If you have symptoms of dehydration — like dizziness, nausea and fatigue — get to the nearest hospital as soon as possible.
Other, more common conditions cause frequent thirst and peeing. So, part of the process of diagnosing AVP-D or AVP-R involves ruling out those conditions. Your healthcare provider may order several tests if you have these symptoms.
A diagnosis of AVP-D or AVP-R involves finding the type and cause.
A water deprivation test is the most reliable way to diagnose either AVP-D or AVP-R. If you get this test, you’ll be under constant supervision during the process. This is because it can cause dehydration.
A water deprivation test involves not drinking any liquid for several hours to see how your body responds. If you have AVP-D or AVP-R, you’ll continue to pee large amounts of watery, light-colored urine. Without the condition, you’ll only pee a small amount of concentrated, dark yellow urine.
Your provider may also recommend the following tests:
Advertisement
Treatment depends on whether you have AVP-D or AVP-R. Even with medical treatment, it’s important to drink water regularly to prevent dehydration.
Desmopressin is the first-line treatment for arginine vasopressin deficiency (AVP-D). It’s a medication that works like AVP. It comes in different forms.
Healthcare providers may also use desmopressin to treat the rare gestational form known as gAVP-d. Drinking more water alone may be enough for the gestational form.
Treatment for arginine vasopressin resistance (AVP-R) is more complicated. It sometimes involves a combination of approaches, like taking the following medications:
If a medication you take causes AVP-R, your provider can sometimes treat AVP-R by switching to a different one.
If you have AVP-D or AVP-R, it’s important to see your healthcare provider regularly. They’ll want to run tests to monitor the condition and make sure your treatment is working.
It may be helpful to ask your provider the following questions:
Advertisement
The outlook (prognosis) for AVP-D and AVP-R is generally good. It usually doesn’t cause serious problems as long as you get treatment and drink enough water.
The risk of complications is higher for:
These groups of people may have difficulty recognizing their thirst, or they may not be able to act on it.
In 2022, several medical organizations decided to change the name of diabetes insipidus to arginine vasopressin deficiency and arginine vasopressin resistance. The main reason for this change is that the shared term of “diabetes” was causing confusion and leading to harmful health effects.
What most people just call “diabetes” is diabetes mellitus. It happens when you have high blood sugar, which causes frequent thirst and urination. It’s much more common than AVP-D and AVP-R (diabetes insipidus). The treatment for diabetes mellitus is very different from that for AVP-D and AVP-R.
The word “diabetes” comes from the Greek word “diabainein,” which means “go through.” This is much like the liquids that quickly go through your body in diabetes mellitus and the arginine vasopressin disorders.
If you have AVP-D (arginine vasopressin deficiency) or AVP-R (arginine vasopressin resistance), you may feel like you live in the bathroom and can never quench your thirst. The good news is that these conditions are manageable.
Advertisement
Your healthcare provider will help you develop a treatment plan and let you know how much water you should drink in a day to keep dehydration at bay. Lean on them for support and guidance.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic offers diabetes insipidus treatment from experienced healthcare providers. Learn how we diagnose and manage this rare endocrine condition.
