A ureteropelvic junction (UPJ) obstruction is a blockage in the upper end of your ureter (renal pelvis). In most cases, it occurs during fetal development. But it can occur in adults, too, sometimes after a kidney stone or surgery in the area. In some infants, it may get better without treatment. But others may need surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
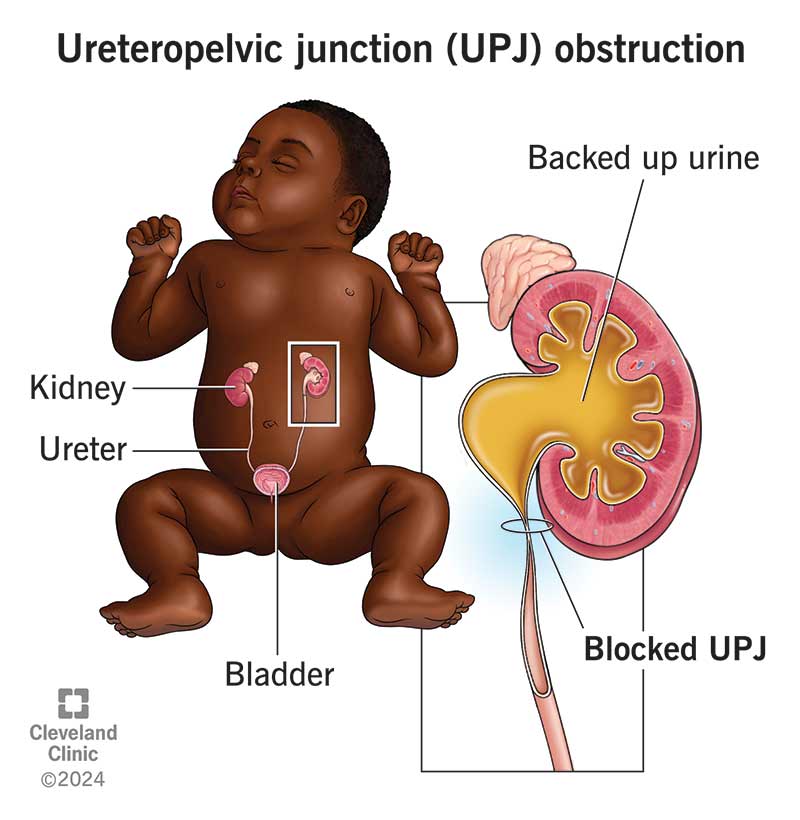
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/ureteropelvic-junction-obstruction)
Ureteropelvic junction (UPJ) obstruction is a blockage in the renal pelvis of your kidney. Each of your kidneys has a renal pelvis. The renal pelvis is located at the upper end of each tube that drains pee from your kidneys to your bladder (ureter). The renal pelvis has a funnel-like shape, and it collects pee.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Typically, each kidney has one ureter. Your kidneys filter fluids and waste out of your blood and create pee. Pee collects in your renal pelvis, flows through the UPJ and then flows from your ureters to your bladder.
If you have a UPJ obstruction, your pee flow is slow or stops completely. This increases your risk of kidney damage.
In most cases, a UPJ obstruction is present at birth (congenital urinary abnormality). It also typically affects only one kidney.
Other names for ureteropelvic junction obstruction include:
Yes, a UPJ obstruction is serious. Without treatment, a UPJ obstruction can cause kidney failure.
UPJ obstruction occurs in about 1 of every 1,500 births.
Common symptoms of ureteropelvic junction obstruction include:
Most ureteropelvic junction obstructions are present at birth. That means the structures of the ureter or kidney didn’t form as expected during fetal development. The other reason is that there’s a blood vessel going across the UPJ and causing compression. They typically occur randomly. But sometimes, you may be more likely to have a UPJ obstruction if someone else in your family has one.
Advertisement
UPJ obstruction is rare in adults. But it can happen after:
Men are more than twice as likely to have UPJ obstruction as women. Your left kidney is also about twice as likely to have a UPJ obstruction than your right kidney.
Ureteropelvic junction obstruction complications may include:
Without treatment, a prolonged UPJ obstruction can cause kidney damage or kidney failure.
In most cases, healthcare providers can diagnose ureteropelvic junction obstruction during prenatal imaging (ultrasound). As pee backs up due to the blockage, the kidney will swell beyond its typical size (hydronephrosis).
After birth, providers can order tests that measure how well your kidneys are making and draining pee. These tests may include:
It depends. If your infant has a ureteropelvic junction obstruction, it may improve on its own within the first 18 months of life. During this time, your child’s healthcare provider will schedule regular ultrasounds and scans to make sure the UPJ obstruction isn’t causing any harm.
If your child’s pee flow doesn’t improve and the obstruction is still there after your child is 18 months old, they’ll likely need an open pyeloplasty. During this surgical procedure, a pediatric urologist will use a surgical knife (scalpel) to make one large cut (incision), remove the obstruction and reattach your child’s ureter to their kidney with a wider opening. An open pyeloplasty usually takes a few hours to complete and has about a 95% success rate.
In some cases, the surgeon may be able to perform a minimally invasive pyeloplasty with a surgical robot to treat UPJ obstruction. They’ll make one small incision and use a surgical robot to operate a laparoscope and other surgical tools. A minimally invasive pyeloplasty has a comparable success rate to an open pyeloplasty. But it’s more technically demanding of a surgeon. It also depends on a child’s age and size.
Another option is an endopyelotomy. The surgeon will insert an endoscope through your urethra, past your ureter, to see the obstruction. They’ll then insert a wire through a channel in the endoscope and use it to cut the obstruction and insert a drain. The drain will remain for a few weeks while you heal. An endopyelotomy doesn’t require any incisions and is more comfortable than an open or robotic-assisted laparoscopic pyeloplasty. But it has a lower success rate. You may need an endopyelotomy more than once.
Advertisement
It depends on the type of procedure you have to treat ureteropelvic junction obstruction. Most people recover in two to four weeks. But your body is unique, and how you recover from UPJ treatment may be different from others. A healthcare provider will give you a better idea of what to expect.
With early diagnosis and treatment, the outlook for ureteropelvic junction obstruction is good. Most children don’t have long-term complications. And if a healthcare provider diagnoses it before birth, it may go away without treatment.
If a provider diagnoses you with UPJ obstruction later in life, you may be more likely to have kidney damage. In severe cases, untreated UPJ obstruction can cause kidney failure and death.
Medical researchers haven’t found a link between diet and nutrition during pregnancy and the formation of UPJ obstruction in a developing fetus. You can’t prevent UPJ obstructions that are present at birth.
In adults without a congenital history of UPJ obstruction, you can help reduce your chances by avoiding:
Reach out to a healthcare provider if you or your infant has the following symptoms:
Advertisement
Go to the nearest emergency room if you can’t pee.
You may want to ask your provider:
Ureteropelvic junction obstructions and ureterovesical junction (UVJ) obstructions happen at opposite ends of your ureter. The UVJ is where your ureter connects to your bladder. A UVJ obstruction occurs in this area. A ureteropelvic junction obstruction occurs in the renal pelvis, where your ureter connects to your kidney.
It can be very scary to hear that there might be a problem during a prenatal imaging test or shortly after your baby’s birth. It’s easy to blame yourself or wonder what you did wrong or what you could have done to prevent it. But ureteropelvic junction obstruction is a condition that just sometimes happens, and healthcare providers aren’t sure why. The outlook for most people who have a UPJ obstruction is good. But talk to a healthcare provider. They understand how you’re feeling and your concerns. They’ll answer all your questions.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.