Cervicitis is inflammation of your cervix. Cervicitis often doesn’t cause symptoms, but if they do happen, they may include abnormal vaginal discharge, painful sex or irregular vaginal bleeding. The most common cause of cervicitis is sexually transmitted infections (STIs). Antibiotics successfully treat cervicitis in most cases.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
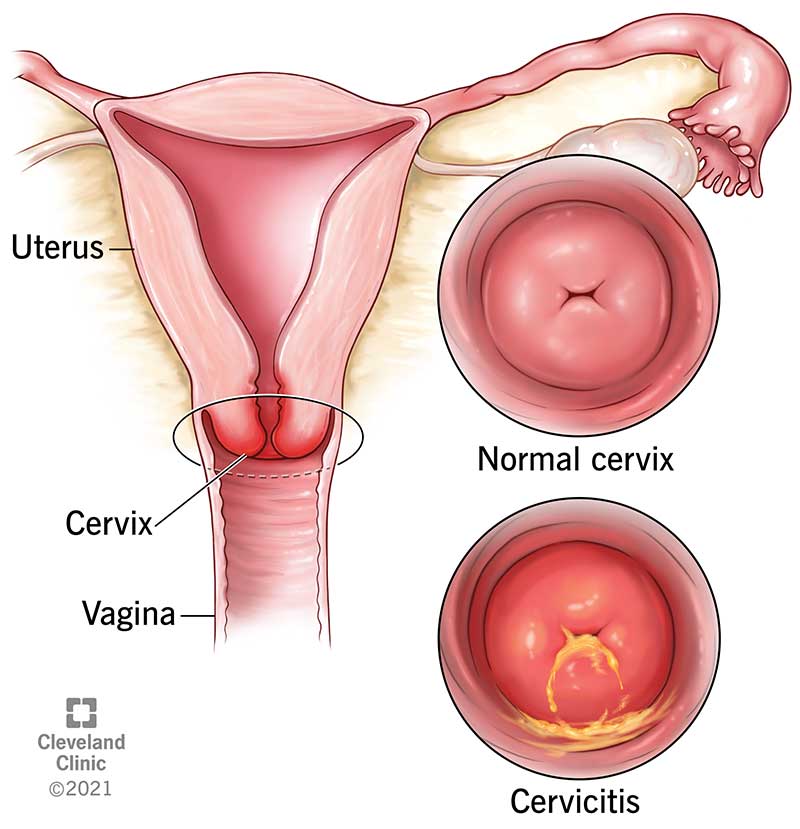
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15360-cervicitis)
Cervicitis is inflammation of your cervix due to infection or other irritants. When the tissue of your cervix is inflamed, it becomes swollen and may bleed more easily. It can cause symptoms like a pus-like vaginal discharge, irregular vaginal bleeding or pain during sex. Some people don’t experience any symptoms at all. Most cases of cervicitis happen due to a bacterial infection, but you can get it anytime something irritates your cervix.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Keeping tabs on what’s normal for vaginal health may feel weird. But it’s important because it helps you notice when something is unusual. Since cervicitis is a common condition, healthcare providers can usually identify it easily during an examination. And because cervicitis may not give you symptoms, seeing your provider regularly for exams (even when you think nothing is wrong) is important.
Cervicitis can be acute or chronic:
It’s hard to say exactly how common cervicitis is, but healthcare providers know it’s very common. Some studies suggest that up to half of all women will have cervicitis at some point in their lives.
The only way to know for sure if you have cervicitis is to have an evaluation from your healthcare provider. Cervicitis symptoms to watch for include:
Advertisement
Not everyone gets symptoms of cervicitis or knows they have it. That’s why regular gynecological exams and testing for STIs (if necessary) are essential so that your healthcare provider can detect cervicitis.
Infections that pass from person to person through sexual activity cause most cases of acute cervicitis. Common causes of acute or infectious cervicitis include:
Causes of noninfectious or chronic cervicitis have little or nothing to do with sexual activity. Common causes are:
Yes. You can pass acute (infectious) cervicitis to your sexual partners. You can avoid spreading it by not having sex for at least seven days after receiving treatment or being completely symptom-free.
Yes. An STI isn’t the only cause of cervicitis. Allergies, irritants and bacteria that naturally occur in your vagina (noninfectious cervicitis) can cause some cases.
No. But HPV (human papillomavirus) can cause cervicitis.
People who have multiple partners or who don’t use condoms or dental dams during sex are at a higher risk for cervicitis. Those with a history of sexually transmitted infections (STIs), or who have partners with a history of STIs, are also more likely to get cervicitis.
Cervicitis isn’t usually life-threatening, but getting proper medical care can help you avoid complications.
Pelvic inflammatory disease (PID) is one of the more serious complications of cervicitis. This type of infection can cause scarring in your uterus, ovaries or fallopian tubes. Scarring can cause complications like pelvic pain, infertility or ectopic pregnancy.
Your risk of STIs (including HIV/AIDS) also increases if you have untreated cervicitis. This is mostly because an irritated or inflamed cervix may let viruses and bacteria into your body and bloodstream more easily.
Your healthcare provider can diagnose cervicitis during a pelvic exam. During your appointment, your healthcare provider will look for:
Advertisement
Your provider will also take a sample of your vaginal discharge and send it to a lab for analysis. To do this, they place a cotton swab into your vagina and collect fluid. Then, a pathologist tests the discharge for infection.
A Pap test can offer clues that could lead to diagnosis, but it’s not a test for cervicitis. A Pap smear is helpful in that it allows your healthcare provider to see changes in the cells of your cervix that may point to dysplasia or cancer. But it can’t diagnose cervicitis or what’s causing it.
Many other conditions have similar symptoms to those of cervicitis like inflammation, irregular discharge, odor and itching. Some of these conditions are:
Cervicitis treatment usually includes antibiotics to eliminate any bacterial infections or STIs that may be causing the condition. Antibiotics successfully treat cervicitis in most cases. Antivirals may be helpful in managing symptoms of cervicitis if genital herpes is the cause. If an STI was the cause, be sure to tell your sexual partners so they can also receive treatment.
Advertisement
You may not need any treatment if allergens or other irritants are the cause of cervicitis. Simply eliminating the product or irritant is usually enough. If the cause was due to leaving something inside your vagina, your healthcare provider will remove the object and recommend further treatment if necessary.
The antibiotic your provider prescribes depends on the cause of cervicitis. For example, doxycycline treats chlamydia. Ceftriaxone treats gonorrhea. A medication called metronidazole is effective when the cause is due to bacterial vaginosis or trichomoniasis.
It can take up to two weeks for cervicitis to clear up. You should take your antibiotics exactly as prescribed by your healthcare provider to ensure the infection is completely gone. Follow your provider’s instructions about when you can engage in sexual activity again.
Cervicitis is a common and treatable condition that goes away within a few weeks with proper treatment. Noninfectious causes may not need any treatment. Follow your healthcare provider’s treatment instructions, even if you don’t have symptoms or your symptoms go away. While receiving treatment, avoid having sex so that you don’t spread the infection to your partner. To prevent cervicitis in the future, practice safe sex and be diligent about visiting your gynecologist for routine exams and STI testing.
Advertisement
Though you can’t always prevent cervicitis, you can reduce your risk by practicing safe sex. Using condoms every time you have intercourse will drastically reduce your risk of sexually transmitted infections. You can also make sure to visit your healthcare provider on a regular basis for a gynecological exam and STI testing (if you’re sexually active).
If you insert things like tampons or diaphragms into your vagina, be sure to remove them when it’s time (according to the directions). You should also avoid using any personal care products that irritate your vagina.
Anytime you notice unusual symptoms, such as unusual vaginal discharge, irritation or painful sex, you should make an appointment with your healthcare provider. Additionally, be sure you’re scheduling routine exams with your gynecologist. Some people don’t experience cervicitis symptoms, so regular checkups are important.
You know your body and what’s normal for you. If you think you may have cervicitis, schedule an appointment with your healthcare provider right away. Not everyone has symptoms, though. For this reason, prioritize seeing your healthcare provider regularly so they can detect signs of cervicitis or other conditions that affect your vagina. Left untreated, cervicitis can cause complications. The good news is that cervicitis is treatable with antibiotics. You can reduce your risk of getting cervicitis by practicing safe sex.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
