An ectopic pregnancy happens when a fertilized egg implants outside of your uterus, most commonly in your fallopian tube. The fallopian tube isn’t made to hold a growing embryo. This condition can lead to bleeding in the birth mother. An ectopic pregnancy is a life-threatening condition that requires emergency treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_0js4px05/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
What is Ectopic Pregnancy?
An ectopic pregnancy is a pregnancy that happens outside of your uterus. This occurs when a fertilized egg implants in a location that can’t support its growth. An ectopic pregnancy most often happens in your fallopian tube (a structure that connects your ovaries and uterus). Ectopic pregnancies more rarely can occur in your ovary, abdominal cavity or cervix. Pregnancies can’t continue if they’re ectopic because only your uterus is meant to carry a pregnancy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Ectopic pregnancies can become life-threatening, especially if your fallopian tube breaks (ruptures). This is a ruptured ectopic pregnancy, and it can cause severe bleeding, infection and sometimes, death. This is a medical emergency. Healthcare providers must treat ectopic pregnancies quickly.
An ectopic pregnancy happens when a fertilized egg implants outside of your uterus. The egg is meant to travel down your fallopian tubes and embed itself into the wall of your uterus, where it can develop. In an ectopic pregnancy, the egg implants in one of the structures along the way. The most common place this can happen is inside your fallopian tubes. The majority of ectopic pregnancies happen here — about 90%.
Ectopic pregnancies occur in about 2% of all pregnancies.
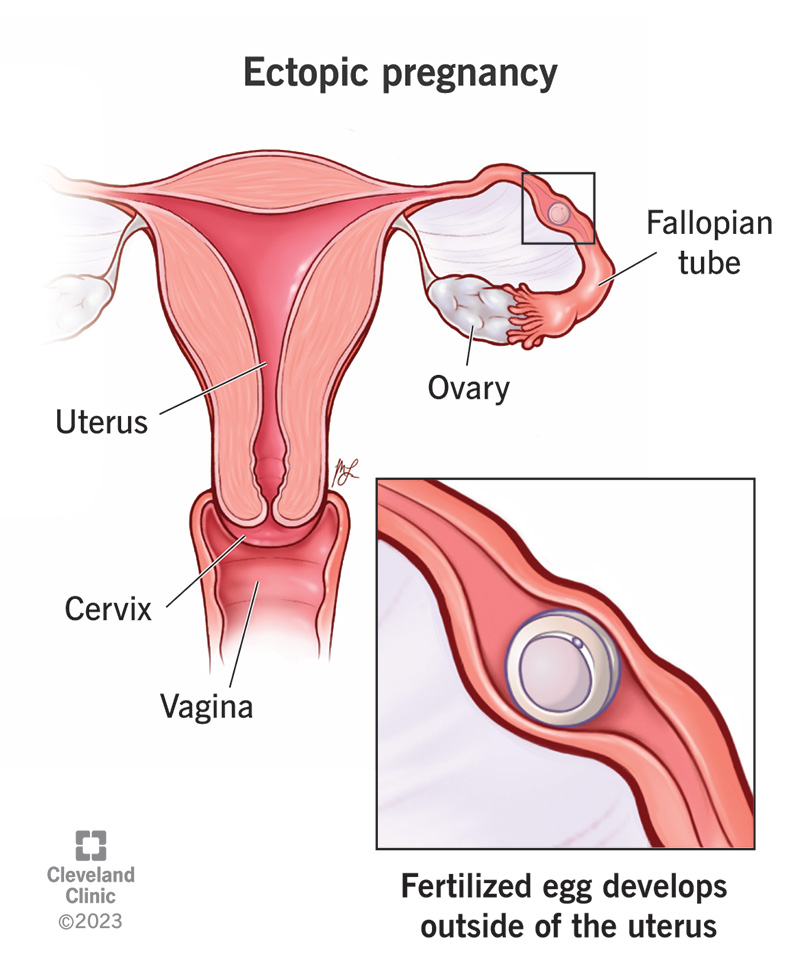
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/9687-ectopic-pregnancy)
The early symptoms of an ectopic pregnancy can be very similar to typical pregnancy symptoms. However, you may experience additional symptoms during an ectopic pregnancy, including:
If your fallopian tube ruptures, the pain and bleeding could be severe enough to cause additional symptoms. These can include:
Advertisement
When a tube bursts, you may feel sudden, sharp lower abdominal pain. This is a medical emergency. You should contact your healthcare provider or go to the emergency room immediately.
In most cases, conditions that slow down or block the movement of the egg down your fallopian tube cause ectopic pregnancy. This could happen because:
There are several risk factors that could increase your chance of developing an ectopic pregnancy. You may be at a higher risk of developing an ectopic pregnancy if you’ve had:
If you realize that you’re pregnant and have an IUD (intrauterine device) in place, or have a history of a tubal ligation (having your tubes tied), contact your healthcare provider right away. Ectopic pregnancy is more common in these situations.
Your risk can also increase with age. Women over age 35 have a higher risk than those under 35.
Up to 50% of women who experience an ectopic pregnancy don’t have any of the above risk factors.
An ectopic pregnancy is a medical emergency. Your uterus is the only organ that can hold a growing fetus. It can stretch and expand as the fetus grows. Your fallopian tubes aren’t as flexible. They can burst as the fertilized egg develops. If this happens, it can cause severe, life-threatening internal bleeding. This is dangerous. An ectopic pregnancy needs to be treated right away to avoid injury to your fallopian tube and other organs, internal bleeding and possibly, death.
Most women don’t know that their pregnancy is ectopic until they visit their pregnancy care provider for a prenatal appointment, bloodwork or ultrasound. Your provider may suspect an ectopic pregnancy based on what happens at this appointment.
To diagnose an ectopic pregnancy, your provider will perform several tests. This may include a pelvic exam and confirmation of pregnancy. These tests include:
Advertisement
If your provider suspects the ectopic pregnancy has ruptured, they can also perform culdocentesis, but this is rarely used.
Once your provider has confirmed an ectopic pregnancy and determined where the fertilized egg has implanted, they’ll discuss a treatment plan with you. An ectopic pregnancy is an emergency and treatment is very important.
Ectopic pregnancy is typically discovered early in pregnancy. Healthcare providers usually diagnose ectopic pregnancies in the first trimester (up to 12 weeks of pregnancy). However, most women discover they have an ectopic pregnancy around eight weeks of pregnancy.
Advertisement
Healthcare providers treat ectopic pregnancies with medication or surgery.
In some cases, your provider may suggest using a medication called methotrexate to stop the fertilized egg from growing, ending the pregnancy. The medication shouldn’t damage your fallopian tubes. You can’t use this medication if your fallopian tube has already ruptured.
Your healthcare provider gives you methotrexate as a single injection. This option is less invasive than surgery, but it does require follow-up appointments so your provider can monitor your HCG levels. It’s important to have consistent follow-up in these cases. In rare cases, a second injection of methotrexate is necessary if HCG levels don’t decrease enough with one dose. Talk to your healthcare provider about the possible side effects and risks of methotrexate so you know what to expect.
Your provider will want to remove the ectopic pregnancy with surgery if your fallopian tube has ruptured or if you’re at risk of rupture. This is an emergency surgery and a life-saving treatment. The procedure is typically done laparoscopically (through several small incisions in your abdomen) while you’re asleep under anesthesia. The surgeon may remove your entire fallopian tube with the egg still inside it or remove the egg from the tube (preserving your fallopian tube).
Advertisement
Most women with a past ectopic pregnancy can have future successful pregnancies. There’s a higher risk of having ectopic pregnancies after you’ve had one. It’s important to talk to your healthcare provider about the causes of your ectopic pregnancy and what risk factors you may have that could cause a future ectopic pregnancy.
You should talk to your healthcare provider about future pregnancies after being treated for an ectopic pregnancy. Although pregnancy may happen quickly after treatment, it’s often best to wait about three months. This gives your fallopian tube time to heal and decreases the risk of another ectopic pregnancy.
In most cases, you can still have a baby if you’ve had one of your fallopian tubes removed. Most females are born with two fallopian tubes. Only one fallopian tube is necessary for a pregnancy. Eggs can still travel down your remaining fallopian tube. There are also assisted fertility procedures like IVF that don’t involve your fallopian tubes. Have an open conversation about your thoughts on future pregnancies with your healthcare provider. Together, you can form a plan and discuss ways to decrease any risk factors you may have.
You can’t prevent an ectopic pregnancy. However, you can try to reduce your risk by following good lifestyle habits. These can include not smoking, reaching and maintaining a healthy weight and preventing any sexually transmitted infections (STIs). Talk to your healthcare provider about any risk factors you may have before trying to become pregnant.
Unfortunately, an ectopic pregnancy is fatal for the fetus and your pregnancy can’t continue. Once an egg implants outside your uterus, you can’t move it to your uterus. Prompt treatment for an ectopic pregnancy is important. If the egg has implanted in your fallopian tube and the tube bursts, there can be severe internal bleeding.
An ectopic pregnancy can be unexpected and scary. You’re probably feeling many emotions, including grief, shock and anxiety. Even if your pregnancy was unplanned, going through an ectopic pregnancy can cause trauma. Talking to your partner, healthcare provider or a mental health professional may be helpful as you navigate your feelings. In time, you’ll heal from an ectopic pregnancy. If a future pregnancy is in your plans, be sure to talk to your healthcare provider about your risk for another ectopic pregnancy.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
