Pessaries are removable devices that go inside your vagina. They provide support to your pelvic organs if you have pelvic organ prolapse or stress incontinence. They’re usually made of soft silicone. The most common types include ring pessaries and the Gellhorn pessary. Your healthcare provider can show you how to insert and care for them.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
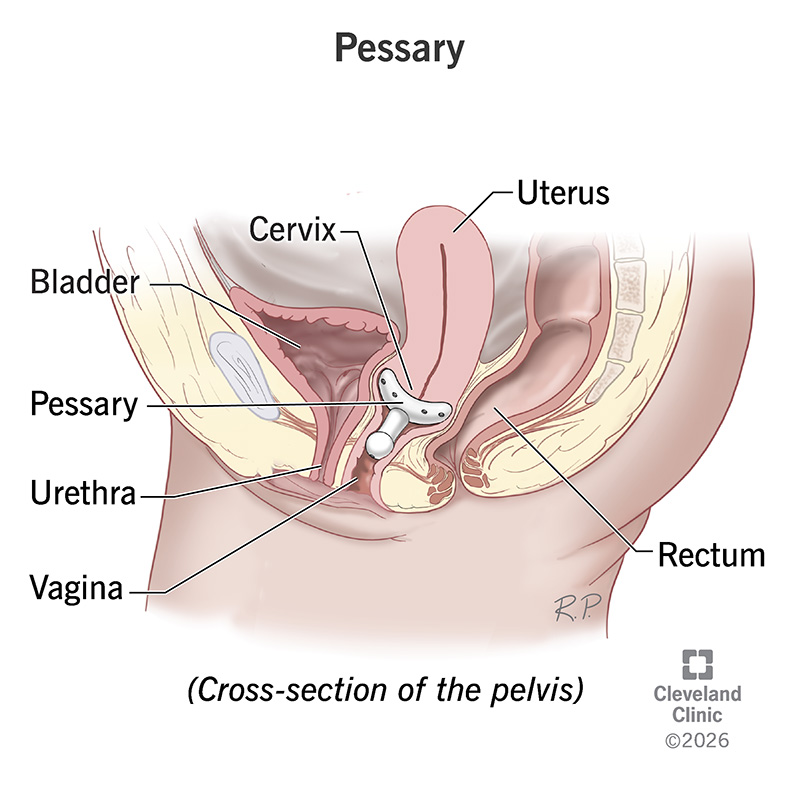
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/16036-pessaries)
A pessary is a removable device that you or your healthcare provider can insert into your vagina to support your pelvic organs. Your pelvic floor muscles provide the structural support necessary to hold your pelvic organs in place. These organs include your uterus, bladder, urethra (the tube that your pee comes out through) and rectum.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If your pelvic floor muscles become injured or weak, the organs can slip out of place and cause uncomfortable symptoms. This is what happens if you have pelvic organ prolapse (POP).
Even common experiences — ranging from pregnancy and childbirth to repetitive heavy lifting — can lead to muscle weakness and slippage over time.
A pessary is one potential treatment option that can help.
A pessary can help manage the symptoms of pelvic organ prolapse and stress incontinence.
In most cases, people choose a pessary when they want symptom relief but want to avoid surgery to fix their pelvic floor muscles. Or, you may choose a pessary if you have medical problems that make surgery too risky.
Sometimes, a pessary is an option after other conservative treatments, like pelvic floor exercises and physical therapy, haven’t helped.
Pessaries come in different shapes and sizes. Most are made of safe, nonabsorbent soft silicone.
Advertisement
The two most common types of pessaries are the:
Your healthcare provider may fit you for other types of pessaries, including the:
Most pessaries require an in-office fitting with your healthcare provider, but some pessaries that treat stress incontinence are available over the counter (OTC). Once inside your vagina, they support your urethra so that pee doesn’t dribble out.
Over-the-counter pessaries include:
During your visit, your healthcare provider will fit you with a pessary. On the day of your appointment, they’ll:
Advertisement
They’ll also tell you what to do if your pessary slips out of place or isn’t working. Don’t feel frustrated if your first pessary fitting isn’t your last. It may take two or three fitting attempts to get things right. Your provider will work with you to find the right device and fit.
The ring pessary is the easiest to take care of on your own. If you have a ring pessary (or another type that you can remove and reinsert), you can remove and clean it weekly or even nightly. Caring for it is simple:
You’ll need follow-up visits every six to 12 months in your provider’s office. During the visit, your provider will examine your vagina to ensure the pessary isn’t scraping or bruising your vaginal walls. They’ll ensure the pessary’s still in perfect working condition.
If you can’t remove the pessary on your own, you’ll need to see your healthcare provider every three to six months for cleaning and checkups.
It depends on the type. Hard-to-remove pessaries can be left in for a few months. You won’t need to remove it until your next provider visit to have it cleaned.
Advertisement
If you can remove your pessary yourself, you may choose to clean it nightly or weekly. Some people prefer to clean it before bed, sleep without it and reinsert it the next morning.
Although you can wear smaller ring pessaries during intercourse, some people choose to remove them before sex.
Follow your provider’s guidance on inserting and removing your pessary based on the type you use.
A pessary can reduce (and often resolve) symptoms of pelvic organ prolapse and stress incontinence without surgery. Also, pessaries are inexpensive and safe to use.
A pessary is a safe treatment, with minimal risks. But pay attention to changes in your body. If something seems off, contact your provider. There are often straightforward solutions to fix the issue.
Signs to look out for include:
Advertisement
Pessaries aren’t for everyone. The downsides of getting one include:
Contact your healthcare provider if you’re experiencing pain or discomfort, or if you’re noticing an abnormal, foul-smelling discharge. You may need to be refitted for a pessary, or you may need treatment for an infection.
The short answer is: it depends.
Often, a pessary provides symptom relief so you can avoid more invasive treatments. But if your prolapse is severe, a pessary may not work for you. Some studies show that while pessaries and surgery both improve symptoms for advanced-stage pelvic organ prolapse, surgery may provide more long-term satisfaction.
Surgery may be a better option if you’re unable to attend the follow-up appointments needed to check on your pessary’s placement and the health of your vagina. These visits are essential.
Your healthcare provider can help you weigh the pros and cons of choosing a pessary over surgery.
A pessary can help you regain the feeling of control that pelvic organ prolapse and stress incontinence can take away. If you’re experiencing symptoms that interfere with your quality of life, contact your healthcare provider. They can explain the benefits of a pessary compared to other treatments. As with most conditions, the treatment that works best is the one that’s tailored to fit your health and lifestyle.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
