Your cervix is a small canal that connects your uterus and vagina. It allows fluids to leave and enter your uterus. During childbirth, your cervix widens so a baby can be born. Your cervix is vulnerable to HPV infections that can cause cervical cancer. Getting vaccinated for HPV and having regular Pap smears can help prevent disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
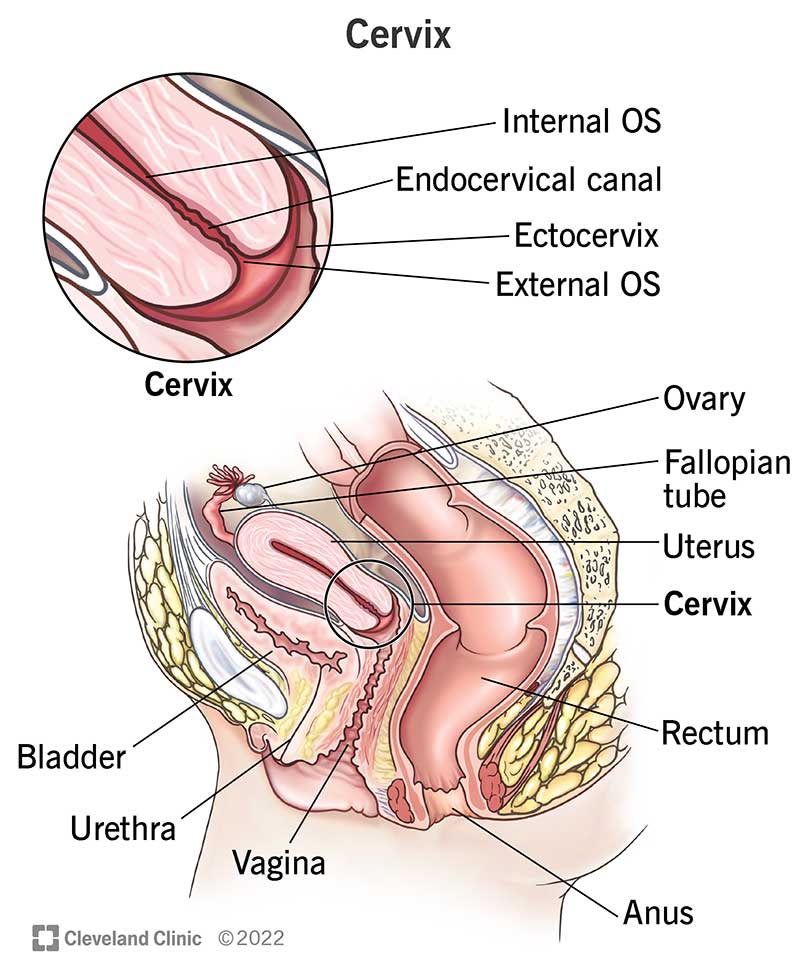
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23279-cervix)
Your cervix is a muscular, tunnel-like organ that connects your uterus and vagina. It’s an important part of the female reproductive system.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your cervix allows fluids to pass between your uterus and vagina. It’s also a powerful gatekeeper. It can open and close in ways that make pregnancy and vaginal delivery possible.
A gynecologist can help make sure your cervix is healthy. Regular Pap smears allow your provider to check for issues that may be signs of disease.
Your cervix plays important roles in the following:
Advertisement
Your cervix is anywhere from 3 to 6 inches deep inside your vaginal canal. It begins at the base of your uterus. It extends downward onto the top part of your vagina.
Yes, depending on the timing of your menstrual cycle. When inserting your longest finger into your vaginal canal, you should eventually reach a barrier that prevents your finger from going further. This barrier is your cervix. It may feel firm and tight, or soft and spongy.
The location and texture of your cervix change depending on whether you’re ovulating. It’s the softest and most difficult to reach during ovulation.
Be sure to wash your hands thoroughly with mild soap and warm water before touching your cervix. Otherwise, you could expose your cervix to bacteria and cause an infection.
Your cervix is shaped roughly like a cylinder or tube. It’s wider in the middle and narrows at both ends, where it opens into your uterus (top) and vagina (bottom).
During a pelvic exam, your gynecologist can see the part of your cervix that’s at the top of your vaginal canal. It looks like a firm, rounded structure. It has a small, slit-like opening in the center. It’s usually pinkish in color. But it may look red or discolored if there’s an issue.
The cervix is usually about an inch long. Cervical sizes vary, though. It depends on your age and whether you’ve given birth.
During pregnancy, the length of your cervix changes. It’s normally longer in the first and second trimesters. It shortens in the third trimester as you get closer to delivery.
Your cervix consists of the following parts:
Your cervix is made of strong fibromuscular tissue. Two main types of cells line your cervix:
These different cell types meet at an area called the transformation zone (TZ). This is where cell changes often happen. Your provider especially looks at the TZ during screenings for cervical cancer.
The most concerning cervical conditions involve the human papillomavirus, or HPV. HPV is a sexually transmitted infection (STI) that sometimes leads to cervical cancer.
Advertisement
Conditions that affect your cervix include:
Pregnancy conditions involving your cervix include:
Many conditions affecting your cervix don’t cause symptoms. You may not know that something is wrong. For example, cervical dysplasia and early-stage cervical cancer often don’t have noticeable signs.
Advertisement
This is why it’s so important to get regular Pap smears. They check for any irregular cell growth. Only a healthcare provider can tell you if your cervix is normal and healthy.
If you do notice signs, they may include:
To keep your cervix healthy, you can:
Advertisement
Your cervix is a tiny organ that plays a big part in pregnancy and your overall health. Take care of your cervix by seeing a provider for regular Pap smears. Usually, your body doesn’t show signs or symptoms to alert you that your cervix has abnormal growths. Getting screened regularly can ensure that your provider catches any issues early.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
