Complex regional pain syndrome (CRPS) is a neurological condition that causes pain and other symptoms in your extremities — most commonly your hand. There are several treatment options for CRPS. The sooner you receive a diagnosis and treatment, the more likely your symptoms will improve.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
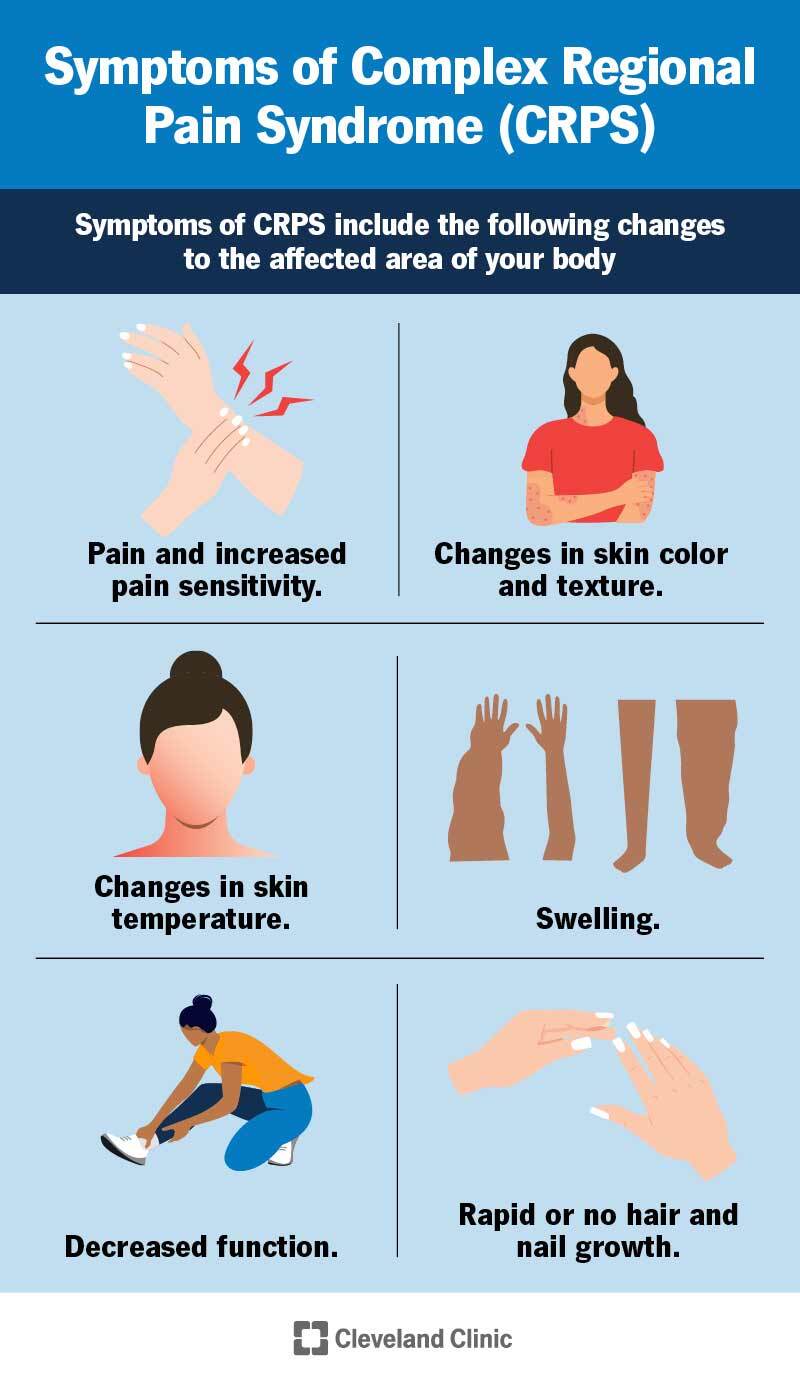
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12085-complex-regional-pain-syndrome-crps)
Complex regional pain syndrome (CRPS) is a condition that causes pain, changes in skin color and other symptoms in a certain part of your body — usually in your extremities. Your extremities include your arm, leg, hand or foot.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The symptoms of CRPS can greatly impact the function of your affected limb, sleep, daily activities and your mental health.
Experts believe that CRPS occurs as a result of dysfunction in your central or peripheral nervous systems. Your central nervous system consists of your brain and spinal cord. Your peripheral nervous system relays information from your brain and spinal cord to your organs, arms, legs, fingers and toes. The abnormal functioning results in an overreaction to pain signals that your nervous system can’t shut off.
There are two subtypes of CRPS:
CRPS can also either be acute (short-term) or chronic (lasting longer than six months). It’s usually treatable.
CRPS more commonly affects adults than children. The peak onset is around 40 years of age. CRPS affects females more often than males.
About 66% to 80% of cases occur in people of European ancestry.
CRPS is relatively rare. It affects about 200,000 people every year in the United States.
Advertisement
How severe and how long symptoms of complex regional pain syndrome (CRPS) last varies from person to person.
Symptoms of CRPS typically start within four to six weeks after an injury, fracture or surgery, but they can develop without a known cause.
The most common and prominent symptom of CRPS is pain. The pain is constant or intermittent and is a burning, stinging or tearing sensation. It’s often deep inside your affected limb.
Sensory changes are also common in the affected area and may include:
Other symptoms of CRPS in the affected area include:
Since the symptoms of CRPS usually improve over time, it’s easiest for healthcare providers to diagnose it in the early stages. It’s important to see a provider soon after you experience symptoms of CRPS.
Researchers aren’t sure why some people develop CRPS while others with similar injuries don’t. They think it’s due to an inflammatory or immune reaction in both your peripheral and central nervous systems.
In more than 90% of cases, CRPS results from nerve trauma or injury to the affected limb that damages the thinnest sensory and autonomic nerve fibers. These small fibers transmit pain, itch and temperature sensations. They also control the small blood vessels and the overall health of surrounding cells.
The most common injury associated with developing CRPS is a bone fracture, especially a wrist fracture. A displaced or splintered bone or pressure from a tight cast can damage nerves.
Other common injuries that can lead to CRPS include:
Advertisement
CRPS can also develop without an obvious injury or due to periods of prolonged immobilization.
Certain factors that may increase your risk of developing CRPS include:
Since CRPS is rare and healthcare providers don’t totally understand it, it’s often misdiagnosed.
There’s no specific test to diagnose CRPS. Healthcare providers mainly diagnose it through a careful medical history, physical examination and review of your symptoms. Your provider will ask you if you’ve had a recent injury or surgery.
Advertisement
They will look for:
They may order imaging tests, such as an ultrasound or magnetic resonance imaging (MRI), to look for underlying nerve damage. But it’s not always possible to find the nerve damage.
Your provider may also order other tests to rule out conditions that cause similar symptoms. For example, electromyography (EMG) may reveal other causes of neuropathy, which may result in some similar pain scenarios.
The goal of treatment is to decrease your pain and other symptoms, restore function to the affected limb and maintain the quality of your life.
It’s important to start treatment early in the course of CRPS. This is because CRPS can cause the affected limb to stiffen over time. In addition, the pain usually worsens without treatment and movement becomes more and more difficult.
It’s best to see healthcare providers who have experience in treating CRPS, if possible. Treatment requires a combination of carefully managed approaches, including:
Advertisement
For young children with CRPS, psychosocial and rehabilitation therapies are the mainstay treatment. Healthcare providers typically only suggest pain-reducing medical procedures for older adolescents who have symptoms that aren’t responding to other therapies.
Physical therapy is one of the most important methods of treatment for CRPS.
A physical therapist can help improve blood flow to your affected limb as well as increase your flexibility, strength, muscle tone and function with certain exercises. An occupational therapist can teach you new ways to accomplish everyday tasks.
Other aspects of physical therapy for CRPS include:
Removing certain barriers that can prevent your nerves from healing can help increase the chance of recovery and the speed of recovery, including:
Other simple steps you can take at home to help your symptoms include:
Having CRPS is associated with worsening anxiety, depression and stress, which can increase pain. Psychotherapy can help. Psychotherapy, also called talk therapy, is a term for a variety of treatment techniques that aim to help a person identify and change unhealthy emotions, thoughts and behaviors.
If possible, it’s best to see a pain management clinical psychologist with training in treating CRPS. During psychotherapy, you talk to the psychologist to learn ways to better cope with factors that contribute to your pain and other symptoms.
No medications are specifically approved for CRPS in the U.S. However, your healthcare provider may recommend certain medications to manage your symptoms.
Medications that have pain-reducing effects include:
The choice of medication(s) to begin with varies from person to person. Your healthcare provider will consider certain factors, including:
Alternative therapies for pain management may include:
If your CRPS hasn’t responded well to the therapies mentioned above or you have severe pain or ongoing CRPS, your provider may recommend the following more invasive treatments:
Each person’s experience with CRPS is different. CRPS usually improves over time and eventually goes away (goes into remission) in most people.
Severe or prolonged cases, which are rare, can greatly affect your life. In some people, CRPS gets worse and even spreads to other areas of their body. Experiencing increased psychological distress during the injury that led to CRPS may affect its severity and prognosis.
CRPS recurs (happens again) in about 10% to 30% of people. Most recurrences are due to unknown reasons.
The most important goals are to relieve pain and restore movement and strength in the affected limb. By achieving pain relief, you increase the odds of improving its function and your quality of life. Carefully selected treatment plans allow some people with CRPS to successfully manage their pain and lead active lives.
Since researchers don’t know the exact cause of CRPS, there’s no conclusive way to prevent it. Some studies have revealed that taking vitamin C before a future surgery might prevent CRPS.
Because of the complexity of this condition and the fact that it’s often misdiagnosed, seek out a pain management specialist or a specialty pain center with knowledge of CRPS if:
In the United States, the Social Security Administration recognizes CRPS as a potential cause of disability depending on its severity and impact on your life. Consult government officials for more information on the Social Security Administration’s eligibility requirements.
No, CRPS isn’t a mental health condition. It’s a neurological condition. CRPS can, however, cause or worsen anxiety, depression and stress. It can sometimes lead to post-traumatic stress disorder (PTSD).
Complex regional pain syndrome (CRPS) can greatly affect your quality of life. The good news is that there are many treatment options and many combinations of options that you can try. The earlier you receive a CRPS diagnosis and start treatment, the better the chance that your symptoms will respond to treatment. If you think you may have CRPS, talk to your healthcare provider. They’re available to help you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Comprehensive pain recovery treatment plans can help you manage your pain levels and symptoms more easily.
