MRSA (methicillin-resistant Staphylococcus aureus) is a type of bacteria that many antibiotics don’t work on. MRSA most often causes skin infections, but it can also cause serious illnesses that are hard to treat.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
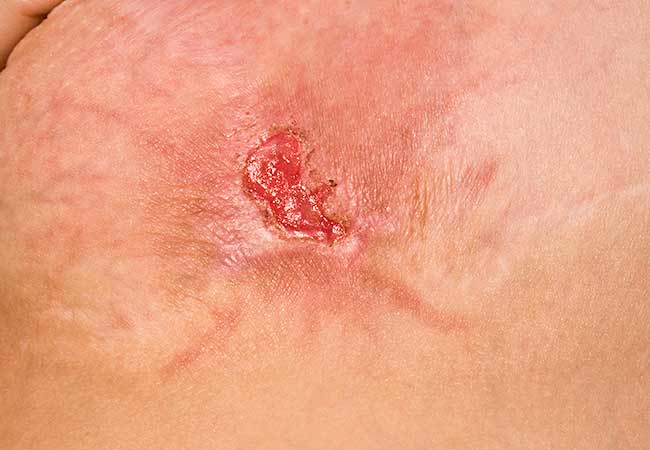
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/mrsa)
MRSA (methicillin-resistant Staphylococcus aureus) is a type of bacteria that’s developed defense mechanisms (resistance) to antibiotics. MRSA infections are hard to treat because very few antibiotics are effective against them. MRSA most often causes skin infections but it can also cause serious infections in your lungs, heart and bloodstream.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
MRSA used to spread mostly in healthcare settings — among people in hospitals or long-term care facilities (healthcare-acquired MRSA or HA-MRSA). But since the 1980s, cases of community-acquired MRSA (CA-MRSA), have been going up. CA-MRSA affects healthy people who haven’t been in a healthcare facility.
Types of MRSA infections include:
Staph infections are any infections caused by the group of bacteria Staphylococcus aureus. MRSA is a specific type of staph infection that’s resistant to antibiotics. Staph infections, in general, are much more common and treatable than MRSA.
MRSA symptoms vary by where you’re infected. Some symptoms common to many types of MRSA infections include:
Strains of Staphylococcus aureus develop antibiotic resistance for many reasons. Sometimes, it happens naturally in the environment. Other times, it happens when the bacteria develop defense mechanisms to block or destroy antibiotic drugs. In hospitals and other healthcare settings, bacteria can become resistant to antibiotics that are used often.
Advertisement
Methicillin is a type of antibiotic related to penicillin. But despite MRSA’s name (methicillin-resistant Staphylococcus aureus), MRSA strains are usually resistant to many types of antibiotics, including:
HA-MRSA is usually resistant to more types of antibiotics than CA-MRSA.
Some people naturally carry MRSA on their skin or in their noses and never get sick from it (colonization). If you’re colonized with MRSA, you’ll test positive on nasal or skin swabs, even if you don’t have symptoms of an infection. You can still spread MRSA to others.
You can get MRSA through:
Yes, MRSA is contagious. It can spread through skin-to-skin contact or on surfaces. Sometimes, people in the same family or living in the same household get it from each other.
You might be at a higher risk for a MRSA infection if you:
If providers can’t get rid of a MRSA infection with antibiotics, it can cause serious complications, including:
A healthcare provider diagnoses MRSA by sending a sample of body tissue or fluid to a lab to be tested. They might try to grow (culture) bacteria from the sample. Examples of samples they could test include:
Providers sometimes test for MRSA colonization with a skin or nasal swab.
Providers treat MRSA infections by caring for open wounds and finding antibiotics that are effective against the strain of MRSA you have. Wound treatment includes draining fluid and surgically removing infected tissue. They also might remove infected medical devices, including prosthetics. Providers treat severe MRSA infections with intravenous (through your vein) antibiotics in the hospital.
Advertisement
Antibiotics a provider might use to treat MRSA include:
Sometimes, MRSA is called a “superbug” because its defense mechanisms against so many antibiotics make it hard to treat. One strategy providers might use is to treat you with more than one type of antibiotic at a time.
If you have a skin infection, your provider will surgically treat and drain your wounds. They might give you topical or oral antibiotics. You’ll need to be treated in the hospital if you have a severe or invasive MRSA infection.
CA-MRSA, especially skin infections, can be easier to treat than HA-MRSA. But up to 70% of MRSA skin infections come back (recur) after successful treatment. This might be because other people you live with or are around a lot are colonized with MRSA, or because MRSA lives on objects and surfaces for a long time, where it can reinfect you.
If you’re being treated in a hospital, you might be in a room by yourself or with special restrictions to prevent spreading MRSA. Your providers may ask any visitors to take precautions, like wearing medical gloves, gowns or masks.
Advertisement
MRSA is contagious as long as tests can detect the bacteria on or in your body. Your provider will swab your nose or skin to test for MRSA to determine if you’re still contagious.
Yes, more than half of all MRSA cases are cured with antibiotics, and providers successfully treat most MRSA skin infections. But serious infections — like pneumonia, endocarditis and bacteremia — can quickly get worse before a provider can find a treatment that works.
The mortality (death) rate of MRSA depends on where you’re infected. For MRSA bacteremia — one of the more serious forms — the mortality rate is between 20% and 50%.
Healthcare providers follow safety and sterilization rules to prevent healthcare-acquired infections like MRSA. These include:
Some steps you can take to prevent CA-MRSA include:
Advertisement
Ask your provider how long you need to use invasive medical devices like catheters and how to prevent infection while you need the device.
If you have an implanted medical device or a weakened immune system, ask your healthcare provider what signs of infection you should look out for. Follow up with them if you have any concerning symptoms. Always see a provider if you have a large wound or one that’s not healing.
Even when you’re in the hospital, communication with your healthcare team is important. Let them know if you’re experiencing symptoms of an infection, like pain, rapid heart rate, weakness or fever.
Go to the emergency room if you have any signs of severe illness, including:
It might be helpful to ask your healthcare provider:
You might hear about MRSA in scary-sounding headlines. But healthcare providers work hard to prevent its spread in hospitals and other facilities, and cases of HA-MRSA have declined in both the U.S. and Europe. Still, all types of MRSA can cause potentially fatal infections.
If you have symptoms of a serious infection or a wound that’s not healing, especially if you have an implanted medical device or weakened immune system, get immediate medical attention. Tell your providers about any medical conditions or devices you have, or if you’ve spent a lot of time in hospitals recently. This information can help them get to the bottom of your symptoms more quickly and treat any infections as soon as possible.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Have a virus, fungus or bacteria? Some of these “bugs” won’t go away on their own. Cleveland Clinic’s infectious disease experts are here to help.
