A breast biopsy is a common procedure that healthcare providers use to determine if a suspicious area in your breast could be cancer. There are several types of breast biopsies. They typically involve a biopsy needle or surgery. Having a breast biopsy doesn’t mean you have cancer: approximately 20% of biopsies result in cancer diagnoses.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_no1phb57/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
A step-by-step explanation of a breast biopsy.
A breast biopsy is when a healthcare provider takes a sample of your breast tissue to examine under a microscope. You may have this procedure if a healthcare provider believes changes in your breasts could be breast cancer.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A breast biopsy is the only way a provider can rule out breast cancer. You may feel anxious or fearful about having the procedure. But it’s important to remember that having a biopsy doesn’t mean you have breast cancer. In fact, 80% of females who have a breast biopsy don’t have cancer.
Healthcare providers usually order breast biopsies after imaging tests show results that might be signs of breast cancer. For example, a provider may order a breast biopsy if:
Different types of breast biopsies involve different procedures. Your healthcare provider will recommend the type that’s best for you, given what they already know about the changes in your breast. The different types are:
Advertisement
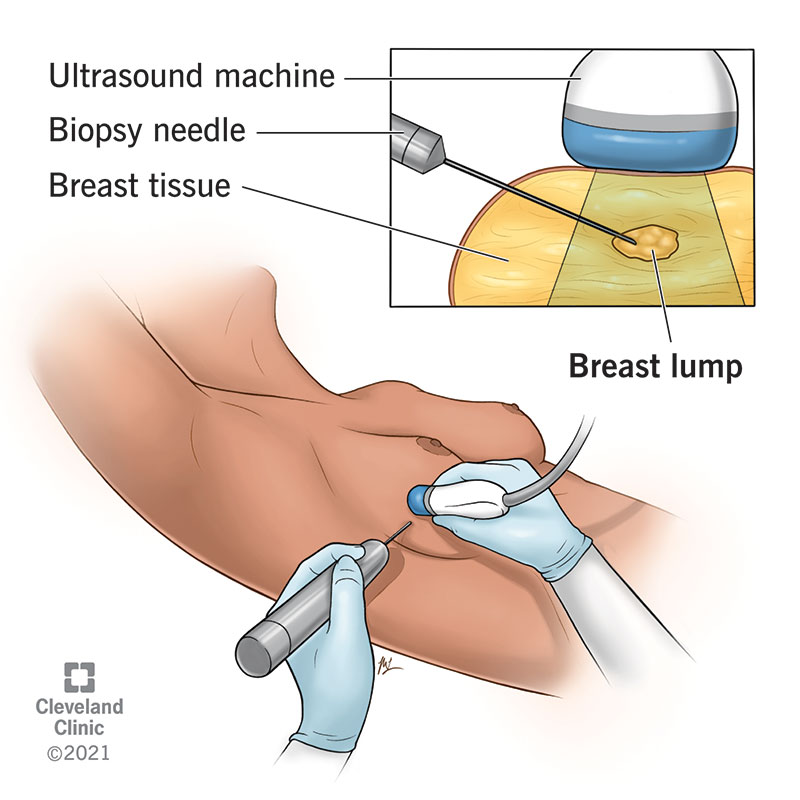
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/24204-breast-biopsy)
If you’re undergoing a breast biopsy, it’s important to let your healthcare provider, surgeon and/or radiologist know if:
Your care team will explain other steps, like whether you should use deodorant on the day of your surgery or if you’ll need someone to take you home after the biopsy.
Your provider may do procedures to pinpoint the area of your breast that they’ll check for signs of cancer. For example, they may do image-guided procedures or a wire localization procedure.
You may have different types of imaging tests just before your breast biopsy. Your provider may refer to this as image-guided procedures since they’ll use the imaging machines during the biopsy. Types of image-guided procedures are:
If you’re having a surgical biopsy, your surgeon may do a wire localization procedure. This involves placing a thin wire in your breast that your surgeon uses to guide the biopsy. They may do this procedure the day of your surgery. A wire localization involves the following:
Your surgeon may use other preoperative localization procedures. These procedures involve placing tiny devices into the targeted area of your breast. They may use:
Advertisement
Your surgeon will use a handheld detector to guide excision.
Your experience will be different depending on the type of breast biopsy that your healthcare provider does:
The procedure times vary depending on the biopsy type:
Advertisement
Everyone is a bit different, but in general, if you had fine-needle aspiration with local anesthesia, the biopsy area may hurt, and you may want to take it easy for the rest of the day. You should be able to get back to your normal activities the next day.
If you have a core needle breast biopsy, your provider may recommend that you avoid strenuous activity for at least two days.
If you’ve had a surgical biopsy, you may have pain in the biopsy area that lasts for a few days. It could take a couple of days to a week before you can return to your normal activities. The recovery time depends on factors like the size of the incision and how much breast tissue your surgeon removed.
There are some common risks and side effects, including:
Contact your surgeon if you experience surgical wound infection symptoms. For example, a fever that’s greater than 101 degrees Fahrenheit (38.4 degrees Celsius) is a reason to call your surgeon.
Breast biopsy complications are very rare. Potential complications are:
Advertisement
If you had a fine-needle aspiration biopsy, a medical pathologist will do cytology tests. The tests help the pathologist rule out cancer or determine if there are cancerous cells in the abnormal area of your breast. The possible results range from no evidence of abnormal cells to precancerous cells or cancerous cells.
If you had a core needle biopsy, excisional biopsy or incisional biopsy, the pathologist will determine if you have a noncancerous (benign) breast disorder, if some tissue is cancerous or if a lump of tissue removed during the biopsy is a cancerous tumor.
If tests detect a cancerous tumor, the pathologist will give your provider a report that notes:
Your provider will share the test results with you and explain what they mean. They may discuss treatment options.
It usually takes one to two weeks for your biopsy results to come back. Waiting for biopsy results can be stressful. Your healthcare team understands that and will be glad to answer your questions. Following your regular routine, doing things that you enjoy and sharing your feelings with others may help.
Call your surgeon if you experience infection symptoms like:
No, but you may feel:
Several types of benign breast disease may cause symptoms that look and feel like breast cancer, including:
If your provider recommends that you have a breast biopsy, it’s important to remember that many things may cause changes in your breasts, and cancer isn’t always the cause. But a biopsy is the only way for your provider and you to know for sure. Preparing for a breast biopsy and waiting for results can be stressful. You may have many questions about what to expect. Your healthcare team understands that you may be anxious or fearful. Don’t hesitate to share your concerns and ask questions about the process.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
A breast cancer diagnosis can turn your world upside down. At Cleveland Clinic, we offer expertise, compassion and personalized treatment plans.
