Your vagina is an important part of both your internal and external reproductive anatomy. It’s a powerful passage that plays a role in sex, menstruation, conception and childbirth. Regular pelvic exams and safer sex practices can help keep your vagina healthy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
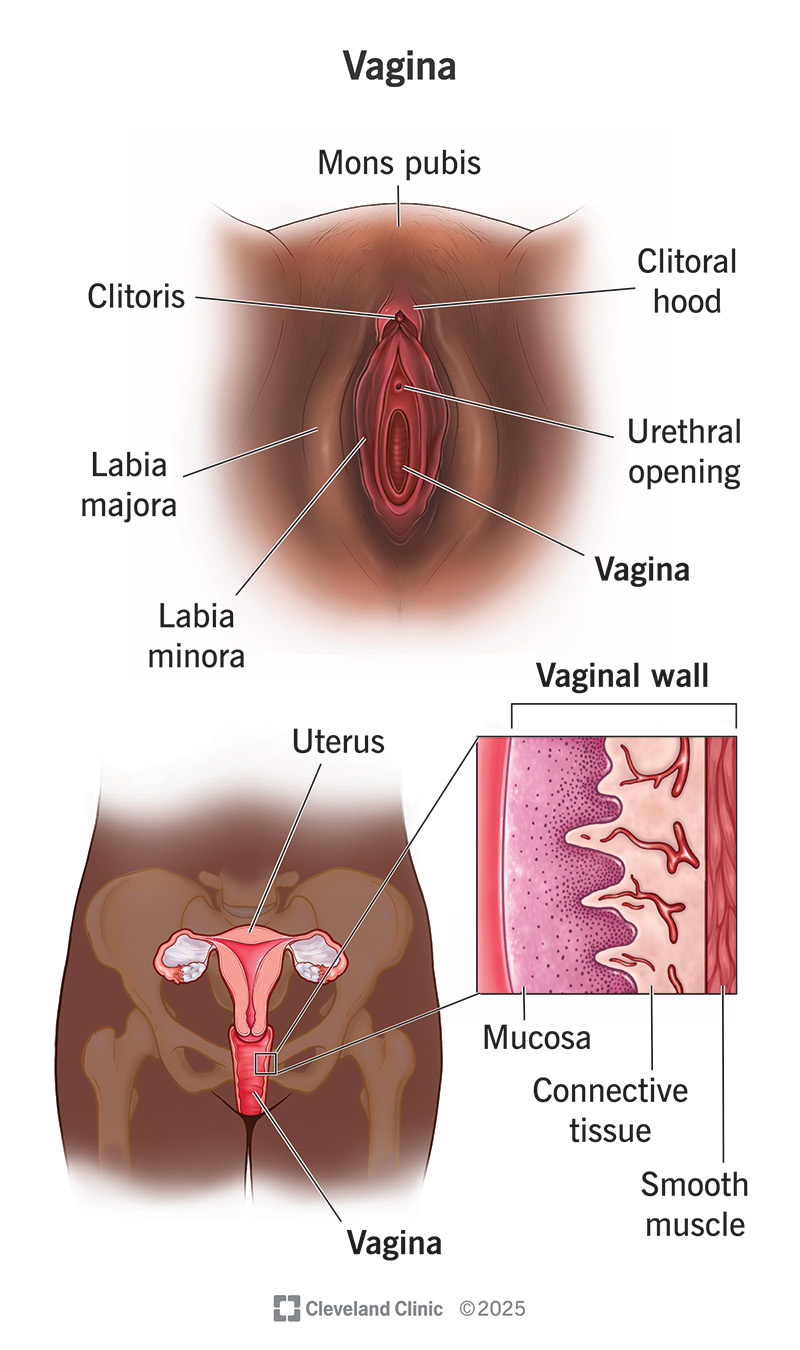
Your vagina is a stretchy, muscular tube that’s an important part of your reproductive anatomy. Many people refer to vaginas as a stand-in for all the reproductive parts associated with being female. But your vagina is just one organ that’s part of your reproductive and sexual health.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Overall, vaginas have a similar shape. But they can vary considerably in:
There’s no one way a vagina can look “normal” — every vagina is different. But certain signs can point to a medical issue with your vagina, like abnormal discharge and bleeding. Talk to a healthcare provider if something seems off. There’s no shame in talking about your vagina — it’s an important part of your health.
Your vagina plays important roles in:
Advertisement
Your vagina changes over your life in response to hormonal changes. This includes life stages like:
The cells in your vagina are especially responsive to the hormone estrogen. Your body produces higher amounts of estrogen in your reproductive years than during menopause.
Your vagina is positioned in your pelvis between your bladder (which holds pee) and your rectum (which holds poop). It has an opening at the “bottom” and connects to your cervix and uterus at the “top.” Certain pelvic floor muscles and uterine ligaments help keep your vagina in its position.
Many people confuse vaginas and vulvas. But they aren’t the same. Your vagina is a canal-like organ located inside of your body that opens outside of your body. Your vulva is the part of your genitals on the outside of your body. Your vulva includes your vaginal opening, as well as your labia, clitoris and the opening to your urethra.
You can think of your vagina as having three main parts:
Your vagina extends from your cervix, a neck-like piece of tissue that connects your vagina to your uterus. Your vagina is slightly wider at the top (near your cervix) than it is at the bottom.
The walls of your vagina (the inside) have three layers:
The walls of your vagina have significant blood supply and nerve endings. These aid in the dynamic changes in size and shape your vagina can go through. They also aid in sexual pleasure and lubrication.
Your vagina ends at a hole called your vaginal opening (vaginal introitus). It’s one part of your vulva. There are folds of skin on both sides of your vaginal opening. The inner folds are called your labia minora (inner lips). The outer folds are called your labia majora.
Advertisement
Sometimes, your inner lips wholly or partially cover your vaginal opening. You may have to part your inner lips with your fingers to feel your vaginal opening.
Your vaginal opening is one of three essential holes in your vulva area that link your body’s internal and external functions. Your urethral opening (pee hole) is at the top. Your vaginal opening is in the middle. And your anus (butthole) is at the bottom.
The vaginal opening also has a hymen. The hymen is a small, thin piece of tissue at the opening of your vagina. It’s formed by fragments of tissue left over from fetal development. The size, shape and thickness of your hymen are unique to you and can change over time.
A vagina looks like a hollow tube with ridges or folds. It’s slightly wider at the top than at the bottom (the opening). Your vagina doesn’t run straight up and down. It’s typically slanted back toward your rectum.
During fetal development, the vagina can develop differently. So, you can be born with a vaginal variant like:
Advertisement
Surgery may help treat these differences.
Vaginas tend to be about 3 to 4 inches (7 to 10 centimeters) deep in an unaroused state. In an aroused state, your vagina can stretch to be about 4 to 8 inches deep. When you’re aroused, blood flow increases in your vulva area, causing it to expand. In a sense, this helps “lengthen” your vagina. Your cervix also lifts slightly when you’re aroused to lengthen your vagina.
But the size of vaginas can vary considerably. It depends on various factors, like your age, genes and if you’ve gone through menopause. Surgeries involving your pelvic cavity may shorten the overall length of your vagina, too.
Vaginas can also change drastically in width from an unaroused to an aroused state and during vaginal childbirth.
Many conditions can affect your vagina. But the most common one is vaginitis, which is vaginal inflammation and/or infection. Several things can cause vaginitis. Some include:
Other vaginal conditions include:
Advertisement
Vaginal conditions cause a range of symptoms. They vary based on the type. Common symptoms include:
You should see a healthcare provider or a gynecologist if you have these symptoms.
Depending on your symptoms, a healthcare provider (usually a gynecologist) can offer the following tests to check your vagina:
To keep your vagina healthy:
Learning about your vagina and what’s normal for you is one of the best things you can do for your reproductive and sexual health. If something changes or doesn’t feel right, reach out to a healthcare provider or gynecologist. It can feel awkward to talk about your vagina. But it’s just as important as any other part of your body. Your provider is there to help you, not judge you.
Your Ob/Gyn is there for you throughout many different parts of your life. At Cleveland Clinic, our experts can help you throughout your entire journey.

Last reviewed on 04/16/2025.
Learn more about the Health Library and our editorial process.