Granulocytes — the most common type of white blood cell — have small granules that release enzymes when your immune system is under attack. This can happen during an infection, allergic reaction or asthma episode. Granulocytes form in your bone marrow and only live for a few days.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
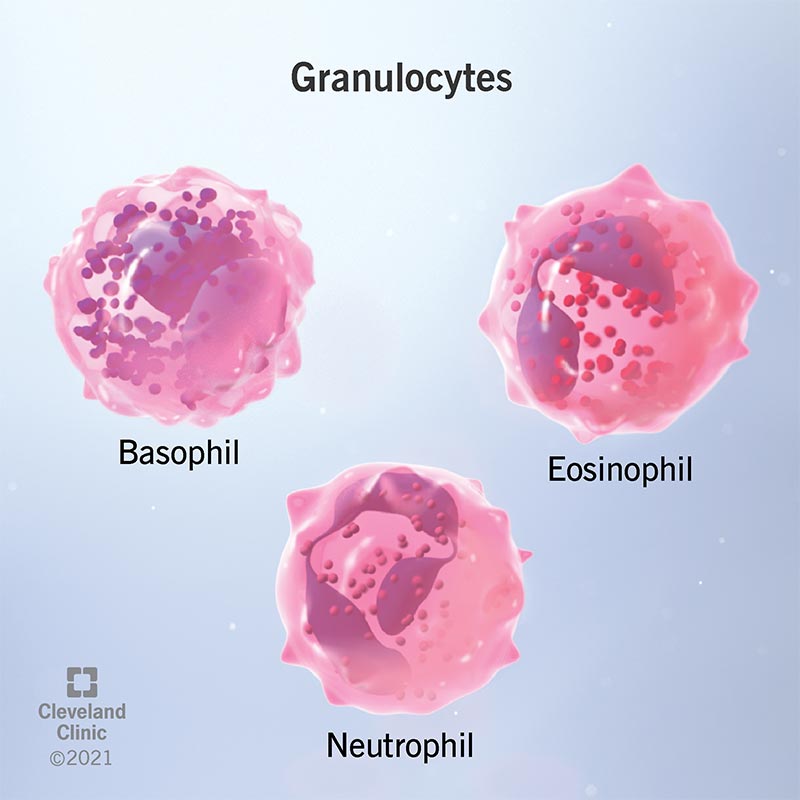
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/22016-granulocytes)
Granulocytes are the most common type of white blood cell. They contain enzyme granules, which form in the cytoplasm (a thick, semi-fluid solution that fills each cell). When inflammation enters your body, granulocytes rush to the area and release their granules to fight infection.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A blood test is the only way to check your granulocyte levels. A high granulocyte count could mean you have some type of infection. A low granulocyte count might point to bone marrow disorders like leukemia or aplastic anemia.
Other names for granulocytes include granular leukocytes, polymorphonuclear leukocytes or PMN cells.
Typically, granulocytes fully develop in your bone marrow before traveling into your bloodstream. If there are immature granulocytes in your bloodstream, it could mean there’s a problem with your bone marrow. Or it could simply indicate an early-stage response to infection. Healthcare providers get concerned when immature granulocytes make up 2% of your total white blood cell count.
Pregnant women and newborn babies may naturally have immature granulocytes in their bloodstream. In these cases, immature granulocytes indicate a healthy bone marrow response and it’s not a cause for concern.
Granulocytes work together to rid your body of infection or allergens.
There are four types of granulocytes. Each type has its own combination of chemicals and enzymes in its granules. As a result, each type of granulocyte has a different function:
Advertisement
Granulocytes form in your bone marrow and enter your bloodstream when necessary.
The normal range for granulocytes is between 1,500 and 8,500 cells per microliter of blood. On a blood test, this might look something like: 1.5 – 8.5 x 10^9/L. This range varies slightly depending on the lab that does the testing.
About 50% to 70% of all the white blood cells in your body should be neutrophils. Eosinophils should account for 1% to 3%, and basophils should make up approximately 0.4% to 1%.
Conditions that affect your granulocytes include:
Symptoms vary depending on the type of condition you have. But people commonly experience:
Your provider can determine your granulocyte count with a complete blood count (CBC), a routine blood test. To find granulocyte levels on your CBC test results, look for the words:
These words are often followed by “abs” which is short for “absolute.” This refers to the absolute number of the cells per unit volume.
Treatment depends on your situation but could include:
If you have cancer that’s affecting your granulocytes, treatment options may include:
If immature granulocytes show up in your bloodwork, your healthcare provider may run more tests to find out why.
If you have an infection, then your provider will prescribe the appropriate medications. If cancer is the culprit, then your provider will talk with you about treatment options, which may include surgery, chemotherapy or radiation therapy.
Advertisement
If you have a condition affecting your granulocyte count, it’s important to protect yourself from infection. Here are some recommendations:
Both are white blood cells, but agranulocytes don’t have any granules in their cytoplasm. (Monocytes and lymphocytes are two examples of agranulocytes.)
Granulocytes play a major role in attacking infection, allergens and other irritants that invade your body. When these white blood cells work as they should, your body can effectively protect itself. But if your body doesn’t make enough granulocytes — or if your granulocyte count is too low or too high — it could mean there’s something more significant going on. If you get sick often or are prone to infections, schedule an appointment with a healthcare provider. They can run tests to find the underlying cause and plan appropriate treatment.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Living with a noncancerous blood disorder can be exhausting. But there’s hope. Cleveland Clinic’s classical hematology experts provide personalized care and support.
