Tuberculosis (TB) is a bacterial infection that usually affects your lungs. It can also spread to other organs. It’s treatable with medications but can be fatal if not treated.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
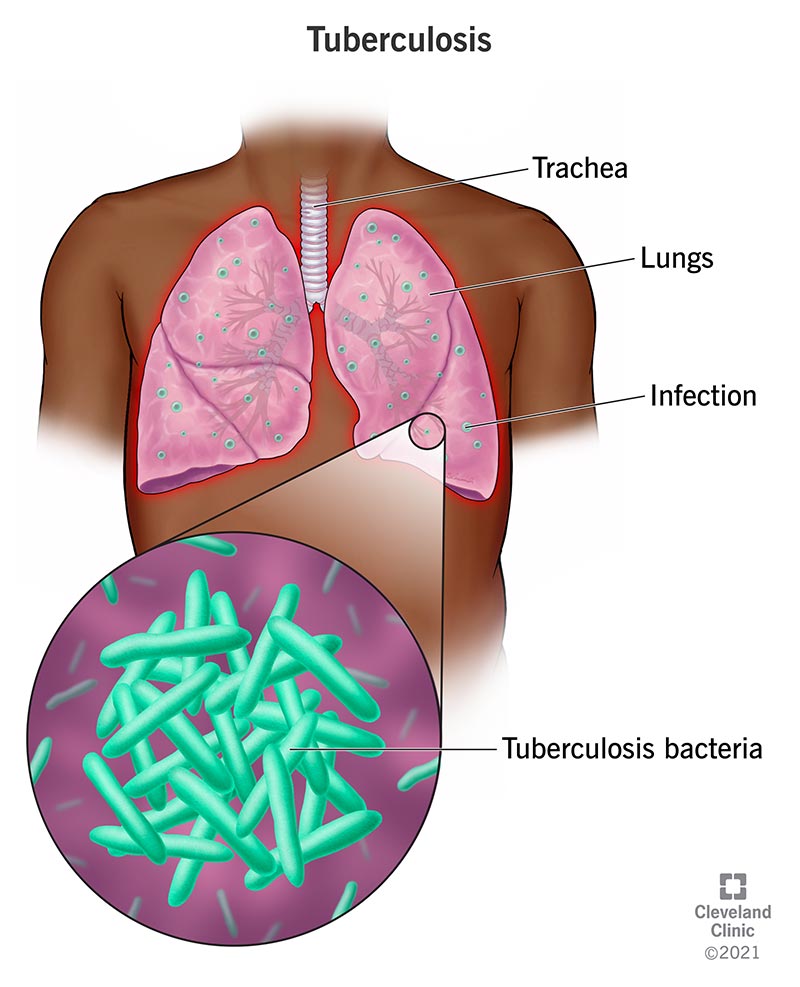
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/11301-tuberculosis)
Tuberculosis (TB) is an illness caused by a bacterial infection. It commonly affects your lungs, but it can also affect other areas of your body like your spine, brain or kidneys.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Not everyone who’s infected with TB gets sick. If you’re infected but have no symptoms, it’s called inactive tuberculosis, or latent TB. TB is dormant (sleeping) inside your body. As many as 13 million people in the U.S. have latent TB. Some people can have a latent TB infection for a lifetime, without ever developing symptoms (active TB).
But TB can become active if your immune system becomes weakened. A weakened immune system may not be able to stop the bacteria from growing.
Active TB symptoms include:
You won’t have symptoms if you have inactive TB. But you might have a positive TB test.
Mycobacterium tuberculosis bacteria cause TB. The germs spread through the air and can infect your lungs when you breathe them in. Sometimes, they also infect other parts of your body.
The most common type of TB is pulmonary (lung) tuberculosis. But the bacterium can also affect other parts of your body (extrapulmonary tuberculosis). You might also hear about miliary tuberculosis, which can spread throughout your body and cause:
Advertisement
TB can spread when a person with active TB coughs, sneezes, talks, sings or laughs. Only people with an active lung infection are contagious. You usually have to spend a lot of time in contact with someone who’s contagious to catch TB. Most people who breathe in TB bacteria can fight the bacteria and stop it from growing. This causes a latent TB infection.
You might be at a higher risk for TB exposure if you:
You might be at a higher risk for getting active TB if you:
Healthcare providers use a skin or blood test to diagnose TB. You might also need:
Healthcare providers treat both active and inactive tuberculosis with specific kinds of antibiotics. You’ll likely need to take a combination of medications to get rid of the infection.
You’ll have to take these medications for a long time — several months. You must take them exactly as your provider prescribes to get rid of all the bacteria. It’s very important to finish your entire prescription.
Specific medications your provider might prescribe include:
You might start having more energy and fewer symptoms within a few weeks of starting treatment. But it’ll take longer than that to complete it. You’ll need to take your medications for at least six to nine months.
If you’ve been exposed to TB, you should talk to your healthcare provider right away. They can talk to you about options for getting tested. It’s important to get tested if you’ve developed any symptoms — you could pass TB on to others.
If you’re taking medications to treat TB, talk to your provider about any side effects. Some side effects can be serious.
You can reduce your risk of contracting and spreading TB by:
Advertisement
In the hospital, the most important measures to stop the spread of TB are having proper ventilation and using personal protective equipment.
Some countries (but not the U.S.) use a TB vaccine called Bacillus Calmette-Guerin (BCG). It’s mostly given to children in countries with high rates of TB.
In 2020, about 10 million people became ill with TB throughout the world, and about 1.5 million people died from it. TB was once the leading cause of death in the U.S., but with new treatments, the number of cases fell rapidly in the 1940s and 1950s. There were 7,860 tuberculosis cases reported in the U.S. in 2021.
TB is responsible for many deaths around the world. But it’s treatable if you take medications as your healthcare provider directs. Make sure you contact your healthcare provider if you think you’ve been exposed to, or have symptoms of, TB.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Have a virus, fungus or bacteria? Some of these “bugs” won’t go away on their own. Cleveland Clinic’s infectious disease experts are here to help.
