Having an illness or infection can make life a little bumpy. It can also make parts of your body swell into bumps you can feel, too. Swollen lymph nodes are normal and a sign that you are or were recently sick. If you have swollen lymph nodes but can’t find an obvious cause, talk to a healthcare provider.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
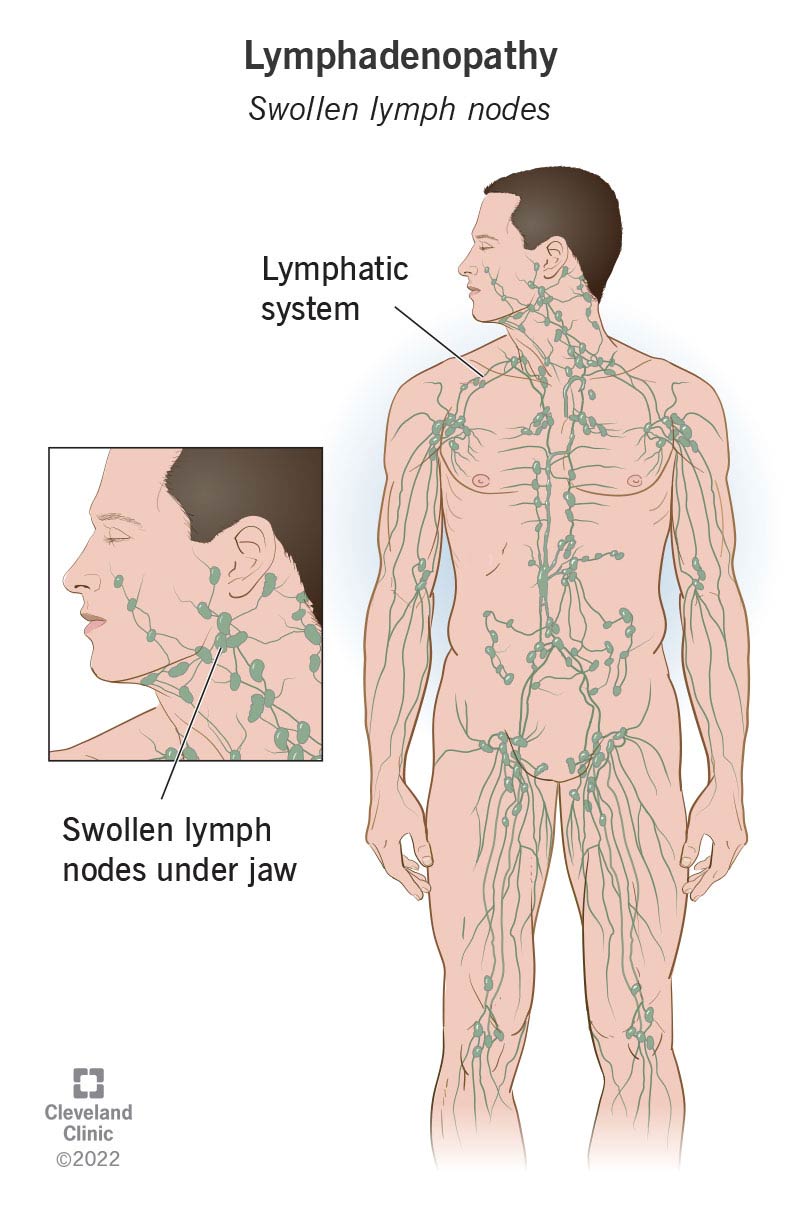
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15219-swollen-lymph-nodes)
When you feel like you’re coming down with something, you might notice some swelling on the sides of your neck. Those bumps on your neck are usually swollen lymph nodes. They probably feel soft, tender to the touch and may even hurt without you touching them.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Swollen lymph nodes (lymphadenopathy) are common. And that’s actually a good thing. These pea- or bean-sized tissues swell when your body fights illness. It’s a normal immune response. It means your immune system is trying to manage whatever’s making you sick, like invading viruses or bacteria.
People often call lymph nodes “glands.” But they’re not. These nodes are part of your lymphatic system. They work like filters, clearing germs and waste from your lymph fluid. This clear or yellowish fluid consists of white blood cells, proteins and fatty compounds called lipids.
Lymph nodes come in groups or clusters, usually around major blood vessel junctions. While some groups are just underneath your skin, others are too deep to feel. Your body has about 800 lymph nodes. They’re found in places like your:
When you have lymph node swelling, your healthcare provider may press the area around the nodes. They’re feeling for things like:
Advertisement
The distribution of lymph node swelling also matters. Some examples of this include:
Your lymph nodes swell when immune cells meet up before your body sends the cells where they’re needed. The immune cells all essentially pile in, causing pressure and swelling. Upper respiratory infections are the leading cause of swollen lymph nodes.
You can also have swollen lymph nodes with:
Less commonly, swollen lymph nodes can happen with serious conditions like:
Treating swollen lymph nodes can depend on a few factors:
Only your provider can tell you what treatment is right for you. They may recommend running blood tests or other lab tests. Some examples include throat cultures for strep throat or wound cultures for an infected wound. They may also ask to take a tissue biopsy. The information your provider offers will be the most relevant to your case and will guide your treatment.
There are a few things you can do to treat swollen lymph nodes at home. They won’t stop the swelling, but may help you feel better. Some treatments you can use include:
Advertisement
You don’t want to prevent swollen lymph nodes. They’re part of how your body defends itself and recovers from infections and illnesses. But you can protect yourself or lower your odds of catching conditions that can cause swollen lymph nodes. Some examples include:
Most swollen lymph nodes aren’t a cause for concern. They’ll go back to their usual size as your body clears the infection affecting them. But if your symptoms are very severe, make you feel concerned or aren’t getting better after a few days, talk to a healthcare provider. They can try to find the cause of your lymph node swelling and determine what to do about it.
You should also talk to a healthcare provider if you have swollen lymph nodes that are:
Advertisement
Yes, swollen lymph nodes are a possible side effect of some vaccines. It’s usually temporary and not serious. If you have concerns about swollen lymph nodes after receiving a vaccine, check with your provider. They can tell you whether you need medical treatment for it.
Swollen lymph nodes can be a literal pain in the neck (or a few other places). But usually, a minor infection or illness is the cause. The swelling should go away once you recover. See a provider if you have swollen lymph nodes that don’t go away, grow over time or cause severe pain. You may have a more serious condition that needs proper diagnosis and treatment.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
