Sinusitis is an inflammation of the tissues in your sinuses (spaces in your forehead, cheeks and nose usually filled with air). It causes facial pain, a stuffy or runny nose, and sometimes a fever and other symptoms. It’s usually caused by the common cold, but other viruses, bacteria, fungi and allergies can also cause sinusitis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
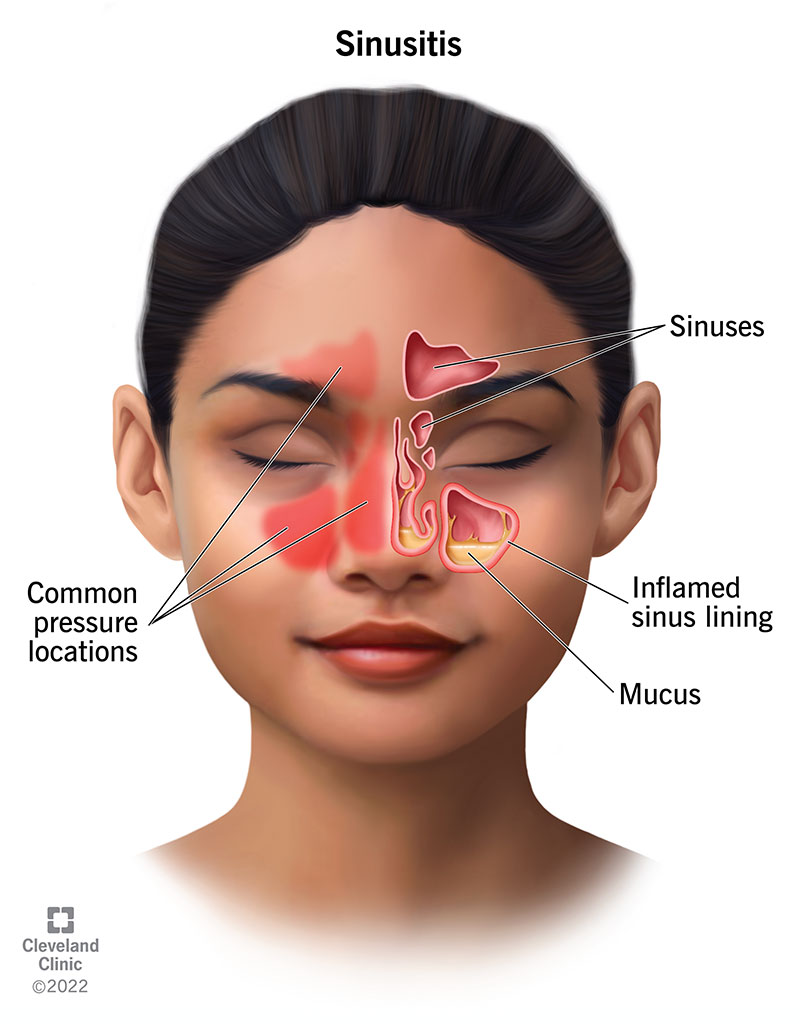
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17701-sinusitis)
Sinusitis is an inflammation, or swelling, of the tissue lining your sinuses. Sinuses are structures inside your face that are normally filled with air. Bacterial infections, viral infections and allergies can irritate them, causing them to get blocked and filled with fluid. This can cause pressure and pain in your face, nasal congestion (a stuffy nose) and other symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Sinusitis is also sometimes called rhinosinusitis.
Your sinuses are four paired cavities (spaces) in your head. Narrow passages connect them. Sinuses make mucus that drains out of the passages in your nose. This drainage helps keep your nose clean and free of bacteria, allergens and other germs (pathogens).
We describe types of sinusitis based on how long it’s been going on (acute, subacute, chronic or recurrent) and what’s causing it (bacteria, virus or fungus).
Viruses, like the ones that cause the common cold, cause most cases of sinusitis. Bacteria can cause sinusitis, or they can infect you after a case of viral sinusitis. If you have a runny nose, stuffy nose and facial pain that don’t go away after ten days, you might have bacterial sinusitis. Your symptoms may seem to improve but then return and are worse than the initial symptoms. Antibiotics and decongestants usually work well on bacterial sinusitis.
Advertisement
Sinus infections caused by fungus are usually more serious than other forms of sinusitis. They’re more likely to happen if you have a weakened immune system.
Colds, COVID-19, allergies and sinus infections all have similar symptoms. It can be difficult to tell them apart. The common cold typically builds, peaks and slowly disappears. It lasts a few days to a week. Nasal allergies cause sneezing, itchy nose and eyes, congestion, runny nose and postnasal drip (mucus in your throat). They usually don’t cause the facial pain that sinus infections do. COVID-19 can cause additional symptoms, like fever and shortness of breath.
A cold, COVID or allergies can all cause sinus infections. You can test yourself or have a provider test you for some viral infections, like COVID-19 and the flu.
Common symptoms of a sinus infection include:
Viruses, bacteria, fungi and allergens can cause sinusitis. Specific triggers for sinusitis include:
Some people are more likely to get sinusitis than others. Risk factors include:
Sinusitis itself isn’t contagious. But the viruses and bacteria that can cause it are. Remember to follow good handwashing practices, avoid other people if you’re sick and sneeze or cough into your elbow.
You don’t necessarily need to treat sinusitis — it often goes away on its own. Very rarely, untreated sinus infections can lead to life-threatening infections. This happens if bacteria or fungi spread to your brain, eyes or nearby bone.
Healthcare providers diagnose sinusitis based on your symptoms and health history. A provider will check your ears, nose and throat for swelling, draining or blockage. They might use an endoscope (a small, lighted instrument) to look inside your nose.
Advertisement
A primary care provider may also refer you to a specialist, like an otolaryngologist (also called an ENT — an ear, nose and throat specialist).
Specific tests your provider might order to diagnose sinus infection include:
There are many treatment options for sinusitis, depending on your symptoms and how long you’ve had them. You can treat a sinus infection at home with:
If symptoms of sinusitis don’t improve after 10 days, a provider may prescribe:
Advertisement
Providers treat chronic sinusitis by focusing on the underlying condition. Treatments can include:
If you need an antibiotic, which one your provider prescribes depends on your specific situation. Some options include:
You might find acupressure, acupuncture or facial massage helpful in reducing symptoms of sinusitis, including draining, pressure and pain. Ask a provider if these therapies might help in your specific case.
No. Providers often wait to see how long your symptoms last before prescribing antibiotics. Many sinus infections are caused by viruses. You can’t cure viral infections with antibiotics. Overusing antibiotics or using them to treat viral infections can lead to unnecessary side effects or antibiotic resistance. This may make future infections harder to treat.
Sinusitis usually only lasts a week to 10 days. You can usually treat it with over-the-counter medicines and at-home treatments. If you have chronic sinusitis or if it keeps coming back, there may be underlying causes that you’ll need to treat.
Advertisement
Depending on the cause, there are a few ways to reduce your risk of getting sinus infections, including:
You can usually care for sinus conditions on your own. But if you continue to have symptoms that concern you or if you get infections repeatedly, talk to a healthcare provider. They can help you understand your next steps.
Go to the nearest emergency room or seek medical attention right away if you experience symptoms of a serious infection, including:
You should ask your provider to show you how to properly use any devices they recommend. This includes nasal inhalers and nasal irrigation devices. It may also be helpful to ask:
Sinus infections are common and usually not serious. They can have many causes, including viruses and bacteria, nasal polyps or allergies. You can usually care for yourself at home by resting, taking over-the-counter products and drinking plenty of fluids. Contact your healthcare provider if your symptoms don’t improve, if sinusitis happens often or if you have any symptom that worries you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Getting rid of chronic sinusitis isn’t easy. Cleveland Clinic’s experts are here to treat your lingering pain, congestion and drainage.
