Pneumonia is inflammation and fluid in your lungs caused by a bacterial, viral or fungal infection. It makes it difficult to breathe and can cause a fever and cough with yellow, green or bloody mucus. The flu, COVID-19 and pneumococcal disease are common causes of pneumonia. Treatment depends on the cause and severity.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
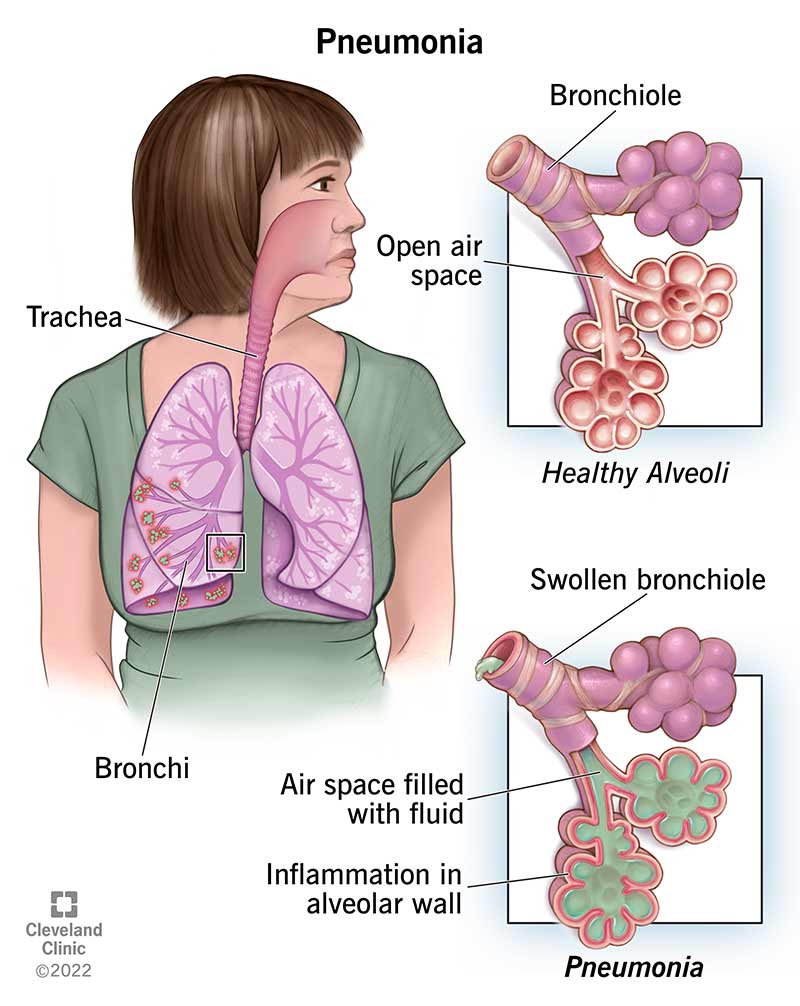
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4471-pneumonia-01)
Pneumonia is an infection that causes inflammation and fluid in the small air sacs of your lungs (alveoli). Bacteria, viruses or fungi can cause it. Bacterial pneumonia is usually more severe than viral pneumonia. Viral pneumonia often gets better on its own.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Pneumonia (pronounced “noo-MOHN-yuh”) can develop when your immune system attacks an infection in your alveoli. This causes your lungs to swell and leak fluids.
You can get pneumonia in one or both lungs. Pneumonia in both lungs is called bilateral or double pneumonia.
You might hear pneumonia defined by where you got the infection. Types include:
Advertisement
You might hear the type of pneumonia described by certain causes, too. These could include:

Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4471-pneumonia-02)
Symptoms of pneumonia can range from mild to severe and sometimes depend on the cause. They include:
Viral pneumonia can also cause dry cough, headache or muscle pain. Symptoms of viral pneumonia usually develop over several days. Symptoms of bacterial pneumonia can develop gradually or suddenly.
Symptoms may appear differently in babies and young children. If you’re over 65 or have a weakened immune system, you may have mild or less noticeable symptoms. Ongoing health conditions may get worse.
Many bacteria, viruses and fungi can cause infections that lead to pneumonia. Adults are most likely to get pneumonia from bacteria. School-aged kids are most likely to get it through a viral infection.
Common causes of pneumonia include:
Less common causes of pneumonia include:
Pneumonia itself isn’t contagious. But the bacteria and viruses that cause it are. For example, many viral infections, like the flu, colds and COVID-19, can lead to inflammation in your lungs. They’re also all contagious. But most people who get viral infections don’t get pneumonia.
Advertisement
On the other hand, some contagious infections, like pneumococcal disease, often cause pneumonia. Fungal infections that cause pneumonia aren’t contagious.
You’re at higher risk for pneumonia if you:
Pneumonia can lead to serious complications, including:
To diagnose pneumonia, a healthcare provider will ask about your health history and examine you. They’ll listen to your lungs with a stethoscope.
Your provider may get additional tests or imaging to help diagnose pneumonia and its cause. These could include:
Advertisement
Sometimes, a provider might not be able to find the exact cause.
Treatment for pneumonia depends on the cause and how serious the inflammation is. If a provider can’t determine the cause, treatment will focus on managing symptoms and making sure your condition doesn’t get worse.
Some treatments could include:
If you have severe pneumonia, you may need to stay in the hospital for treatment. You’re more likely to be hospitalized for pneumonia if you’re:
Advertisement
If your provider says it’s OK to recover at home, over-the-counter medications and other at-home treatments can help you manage the symptoms. These include:
Pneumonia can be life-threatening if left untreated, especially if you have an underlying health condition. Contact a healthcare provider if you have these symptoms, especially if they’re new or getting worse:
Go to the emergency room or call 911 if you:
How soon you’ll feel better depends on:
Most symptoms of bacterial pneumonia usually start to get better within a day or two after starting treatment. Some symptoms, like cough and fatigue, may linger for several weeks. It may take six to eight weeks to feel back to normal if you’ve been hospitalized.
You may have lingering health issues after recovery. You might notice:
Children who’ve recovered from pneumonia have an increased risk of chronic lung diseases.
Follow up with your healthcare provider if you have ongoing health concerns after recovering.
Viral pneumonia often goes away on its own. But you should always have a healthcare provider check you out. Some cases of pneumonia can be serious, especially if bacteria cause it. Bacterial pneumonia is best treated with antibiotics. The only way to know the difference is to see a provider.
If you have bacterial pneumonia, you’re no longer considered contagious when your fever is gone and you’ve been on antibiotics for at least two days. If you have viral pneumonia, you’re likely to be contagious until you feel better and have been fever-free for several days.
The best way to prevent pneumonia is to get vaccinated against bacteria and viruses that commonly cause it. These vaccines won’t protect against all types of pneumonia, but if you do get sick, it’s less likely to be severe. Your healthcare provider can recommend which vaccines make sense for you or your loved ones.
Vaccines that can reduce your risk of pneumonia include:
There are also everyday precautions you can take to help reduce your risk of getting and spreading pneumonia:
Bacterial pneumonia tends to be more common and more severe than viral pneumonia. It’s more likely to require a hospital stay. Providers treat bacterial pneumonia with antibiotics. Viral pneumonia causes flu-like symptoms and is more likely to resolve on its own. You usually don’t need specific treatment for viral pneumonia.
When you’re sick with respiratory symptoms, you may wonder: Is it just a cold or could it be pneumonia? It can be worrying if you’re not sure if something more serious might be going on. A high fever, bloody or unusually colored mucus, chest pain and shortness of breath are symptoms you shouldn’t ignore. Don’t hesitate to get medical attention when your body is telling you that something isn’t right.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
