Cervical cancer is cancer of the cells in your cervix. HPV infections cause most cervical cancers. Getting Pap tests and practicing safe sex are the most important steps you can take to help prevent cervical cancer. Surgery, radiation and chemotherapy are the main treatments.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
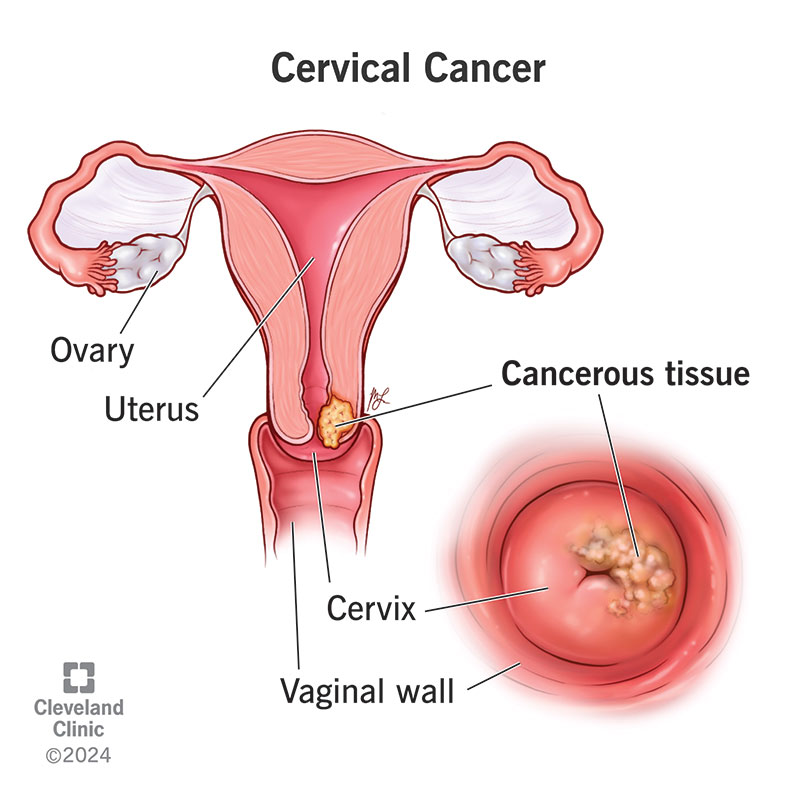
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12216-cervical-cancer)
Cervical cancer is cancer that begins on the surface of your cervix. It happens when the cells on your cervix start to change to precancerous cells. HPV (human papillomavirus) infection causes almost all cases of cervical cancer. HPV is a virus that spreads through sexual contact. You can lower your risk of cervical cancer by getting regular cervical cancer screenings (like a Pap smear) and receiving the HPV vaccine.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cervical cancer often doesn’t cause symptoms until it begins to spread. That’s why regular screenings and the HPV vaccine are so important. Cervical cancer is highly treatable when found in the early stages. A healthcare provider can treat it with surgery, radiation therapy, chemotherapy and other cancer medications.
About 14,000 people in the United States receive a cervical cancer diagnosis each year. Women between the ages of 35 and 44 are most likely to receive a diagnosis.
There are two main types of cancer of the cervix: squamous cell carcinomas and adenocarcinomas. About 80% to 90% of cervical cancers are squamous cell carcinomas, while 10% to 20% are adenocarcinomas. You can also have a mix of both types.
Early stages of cervical cancer don’t usually involve symptoms and are hard to detect. The first signs of cervical cancer may take time to develop.
Signs and symptoms of Stage I cervical cancer can include:
If cancer has spread to nearby tissues or organs, symptoms may include:
Advertisement
If you experience abnormal bleeding, unusual vaginal discharge or any other unexplainable symptoms, you should contact a healthcare provider.
Most cervical cancers are caused by HPV, a sexually transmitted infection. HPV spreads through sexual contact (anal, oral or vaginal) and can lead to cancer. Most people will get HPV at some point in their lives and not realize it because their bodies fight off the infection. But if your body doesn’t fight off the infection, it can cause the cells of your cervix to change to cancerous cells.
There are more than 100 kinds of HPV, and about a dozen of them have been shown to lead to cancer. Early detection of these HPV strains is key in preventing cervical cancer. The HPV vaccine can help prevent HPV infection by protecting you against the HPV that causes up to 90% of all cervical cancers.
In many cases, you can have no known risk factors for cervical cancer. Other times, you may have one or more risk factors. Some risk factors within your control are:
There are some risk factors you can’t change or control. These are:
Precancerous cell changes can progress slowly, but once they turn into cancer, it can progress quickly. It takes between three and seven years for abnormal cell changes to become cancer. Pap tests can detect precancerous cell changes before they have a chance to turn into cancer. If you’re keeping up with regular Pap tests, cervical cancer isn’t likely to go unnoticed.
Early detection and treatment of cervical cancer are key to avoiding life-threatening complications of the disease.
Some possible complications of cervical cancer include:
Advertisement
Cervical cancer usually develops slowly and over many years. Before turning into cancer, the cells in your cervix go through a lot of changes. The once normal cells in your cervix start to appear irregular or abnormal. These abnormal cells may go away, stay the same or turn into cancer cells.
Regular cervical cancer screenings with a Pap test can detect most cases of cervical cancer. The goal of cervical cancer screening is to detect cell changes on your cervix before they become cancer. A Pap test, or Pap smear, involves looking at cells from your cervix under a microscope. These cells are examined for signs of precancers or other irregularities.
If your Pap comes back as abnormal, further testing is necessary. This could include an HPV test, which is a specific test that checks the cells of your cervix for the HPV strains that are most likely to cause cancer.
If your screenings come back as abnormal, your healthcare provider will want to run more tests to confirm you have cervical cancer. The first step in that is typically a colposcopy. A colposcope magnifies the cells of your cervix so your healthcare provider can see irregular cells. If the cells look suspicious or unusual, they’ll remove a sample of cervical cells and send them to a lab for further testing.
Advertisement
They can use any of the following methods to get a sample of tissue from your cervix:
If the results from these tests confirm cervical cancer, further tests will determine whether the disease has spread (metastasized). These tests might include:
The results of these tests also help your healthcare provider stage the cancer. Cervical cancer ranges from Stage I (least severe) to Stage IV (most severe). Staging helps your healthcare provider determine the best treatment plan.
There are four main stages of cervical cancer, and within each stage, there can be several different substages. The main stages of cervical cancer are:
Advertisement
Your healthcare provider is the best person to discuss what stage of cervical cancer you have and what it means.
Cervical cancer cells look different under a microscope compared to normal or healthy cells. Only a pathologist can identify these changes. You wouldn’t be able to see or touch cervical cancer on your own. A pathologist will notice the following features of cervical cancer cells:
Treatment for cervical cancer is based on many factors, including the stage of the disease, your age and general health, and if you want children in the future.
The treatments for cervical cancer are radiation, chemotherapy, surgery, targeted therapy and immunotherapy.
Clinical trials are another option. They’re controlled research studies to test new treatments for cancer. Talk to your oncologist if you’d like to participate in a clinical trial.
Some people use alternative treatments like diet, herbs, acupuncture and other methods to supplement their cancer treatment. Talk to your healthcare provider about alternative methods that claim to relieve cancer symptoms. Some may help, but others could be harmful.
Radiation therapy uses energy beams to kill cancer cells on your cervix. There are two types of radiation therapy:
Chemotherapy (chemo) uses drugs injected into your veins or taken by mouth to kill cancer cells. It enters your blood and is effective for killing cells anywhere in your body. There are several drugs used for chemo and they can be combined. Chemo is often given in cycles. The length of the cycle and the schedule or frequency of chemotherapy varies depending on the drug used and where the cancer is in your body.
Different kinds of surgery are used to treat cervical cancer. Your provider can remove just the cancerous tissues when the cancer is in its early stages. Some of the most common kinds of surgery for cervical cancer include:
Some people may have a combination of treatments. Your provider may use radiation or chemotherapy to treat cancer that has spread or come back (recurred). Sometimes, your provider will use radiation and chemotherapy before or after surgery.
Targeted drug treatment destroys specific cancer cells without damaging healthy cells. It works by targeting proteins that control how cancer cells grow and spread. As scientists learn more about cancer cells, they’re able to design better-targeted treatments that destroy these proteins.
Immunotherapy uses medicine to stimulate your immune system to recognize and destroy cancer cells. Cancer cells pretend to be healthy to hide from your immune system. Immunotherapy helps target these signals so the cancer cells can’t trick your body into thinking it’s a healthy cell.
Yes. It’s a highly treatable cancer, especially if it’s caught in the early stages. Healthcare providers typically use the term “remission” to describe a cancer that has gone away. It can still come back.
You may not need chemotherapy for Stage I cervical cancer. Surgery is usually the first treatment your provider will recommend for Stage 1. But there are times when chemotherapy is also an option.
A cure at this stage is unlikely, but remission is possible. Stage IV is the most advanced stage of cervical cancer. It means the cancer cells have spread to other organs and tissues throughout your body. Your healthcare provider will still recommend the best ways to try to eliminate the cancer. Radiation therapy, chemotherapy and targeted treatment are still options for you.
Cervical cancer is serious, but it’s highly treatable, especially in the early stages. If you do receive a diagnosis, it’s normal to worry about your health or feel angry that cancer has happened to you. You want the cancer to go away so you can continue living a long and fulfilling life. Ask your healthcare provider about what treatment they recommend.
Cancer treatment can be difficult and cause unpleasant side effects. Lean on your loved ones for help. Support groups for people with cancer can also be helpful when you need someone to understand what you’re going through.
Once treatment is over, your healthcare provider will want to monitor you closely to ensure the cancer doesn’t come back. Even if you reach remission, you’ll likely always have cancer in the back of your brain, feeling worried that it can come back. This is a normal response to having cancer. Talking through your feelings with a counselor, close friend or healthcare provider can be beneficial.
Survival rates for cervical cancer are very good, especially when your provider catches cells at the precancer level (before they change to cancer cells). According to the National Cancer Institute, the five-year relative survival rates are:
These statistics don’t necessarily predict what will happen to you. Your healthcare provider is the best person to discuss your outlook which is unique to you.
There are some things you can do to help prevent cervical cancer. Receiving regular gynecological exams and getting Pap tests are the most important steps to take toward preventing cervical cancer. Other things you can do are:
You should contact a healthcare provider if you develop abnormal or suspicious symptoms. Some things to watch for include:
Contact your healthcare provider if you’re unsure when your last Pap test was. They can get you on a regular schedule to ensure any changes to your cervix are caught early.
Receiving a cervical cancer diagnosis can cause a flood of emotions. You’ll likely have many questions over the next several weeks and months. What treatment gives me the best chance at remission? Is the cancer going to come back? Discuss your questions and concerns with your healthcare team to make sure you understand your diagnosis and treatment plan. Treatment could involve surgery, chemotherapy, radiation or a combination of treatments.
It’s easy to put off Pap tests and other gynecological exams. But these tests are critical in detecting cervical cancer early, when it’s most treatable. If you’re unsure when your last Pap test was, talk to a healthcare provider so they can get you on a regular schedule.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Get expert diagnosis and the latest treatments for cervical cancer at Cleveland Clinic. We’re here to support you on your journey.
