A lung transplant replaces one or both of your damaged or diseased lungs with healthy donor lungs. You may need it if you have a condition or injury that doesn’t respond to other treatments. Risks include rejection and infection. Many people return to a good quality of life within three to six months.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
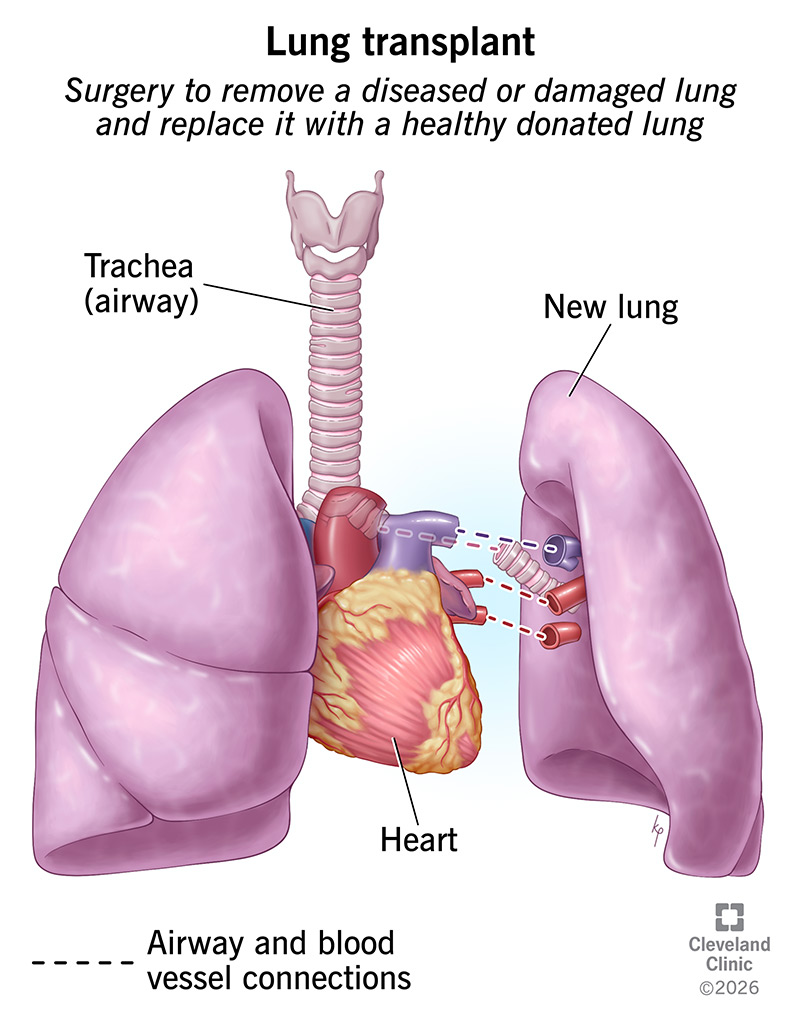
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/lung-transplant)
A lung transplant is a type of surgery that removes your diseased or damaged lung and replaces it with a healthy donated lung. Donated lungs come from a deceased person.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
To get a lung transplant, you must have a serious lung condition that doesn’t respond to other treatments or medications. You’re a good candidate for the procedure if you:
There are three main types of lung transplant:
Diseased or damaged lungs can prevent your body from getting oxygen. Many different conditions can affect how well your lungs work. Some common conditions include:
For many, medications and therapies can help successfully treat these conditions. But when treatments no longer help, healthcare providers may suggest a lung transplant.
Advertisement
In 2023, providers performed over 3,000 lung transplants in the U.S. But there aren’t enough donor lungs available for people who need a lung transplant.
Increasing organ donation awareness is one of the best ways to increase the number of donor lungs. Providers do this through public events, presentations and media campaigns. Many people register as organ donors when they get a driver’s license or state ID card. They can also register online.
If a provider recommends a lung transplant, you must go through an in-depth screening or evaluation. During the screening, members of your care team will:
After completing testing and meeting with transplant surgeons, they’ll present you to a selection committee. After their approval, they’ll place you on a national waiting list. You match with a donor by having compatible:
You must have the same blood type as your donor, and your lungs must be about the same size. You may be on the waiting list for months until a good match is available. Providers will give you a better idea of what to expect as far as your time on the waiting list.
A lung transplant is a major surgery. You’ll receive general anesthesia so you won’t be awake and won’t feel pain during the procedure. Once you’re asleep, your lung transplant team will:
Advertisement
A lung transplant takes a lot of time. A single lung transplant takes about four to six hours. A double lung transplant takes about six to eight hours.
After the lung transplant is complete, your anesthesiologist will stop giving you anesthesia. Providers will move you to an intensive care unit (ICU). They’ll wait for you to fully wake up and monitor your overall health. While in the ICU, the mechanical ventilator will continue to help you breathe.
Once your care team thinks it’s safe, they’ll take you off the ventilator. They’ll also remove the catheter and move you to a post-transplant unit. They’ll monitor how you and your body respond to immunosuppressants. They’ll adjust your dosages as necessary. Immunosuppressants help prevent lung transplant rejection. Lung transplant rejection is when your immune system doesn’t accept your new lung and attacks it. It can happen in rare cases.
As you heal, you’ll start working with physical therapists and respiratory therapists. They’ll help you build up strength in your lungs and the rest of your body.
After you’ve made enough progress and providers think it’s safe, you can go home. Most people stay in the hospital for 12 to 14 days after a lung transplant. But your body is unique. Your hospital stay may be shorter or longer.
Advertisement
A lung transplant can increase your overall quality of life. Examples include:
A 2023 report lists the lung transplant survival rates as:
Some people live over 20 years after a lung transplant.
Potential lung transplant complications include:
It takes a long time to make a full recovery after a lung transplant. Your progress will come in stages:
Advertisement
Remember, your body is unique. Your recovery times and benchmarks after surgery may be different. It’s important to closely follow your healthcare provider’s instructions. This helps ensure the fastest recovery.
After a lung transplant, you’ll need regular follow-up appointments with your providers. Initially after your release from the hospital, you may need one or more appointments every week for lab tests, check-ups and therapy. Once you’re stable, you’ll see your providers about every three months in an outpatient clinic.
Call your provider immediately if you aren’t feeling well. Let them know if you notice any discomfort or changes to your breathing.
Talk to your provider before you start taking any new medicines after a lung transplant. These include prescribed and over-the-counter medications. They also include vitamins and herbal supplements. They may affect how well your immunosuppressants work.
A lung transplant is a major surgery. It has the potential to improve your quality of life after a condition affects how well your lungs work. The pre-screening process before you’re on a lung donor list can be exhausting. And once you’re on the list, you may have to be patient. It can take some time to find the perfect match. The recovery process can also be challenging, too. So, it’s important to have a strong support system that can help you through the entire process. Healthcare providers are also available to answer any questions you have and make sure you’re comfortable with your choices.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When end-stage lung disease affects your life and your breathing, a lung transplant might be an option for you. Cleveland Clinic experts are here to help.
