Bronchiectasis is a condition where damage causes the tubes in your lungs (airways) to widen or develop pouches. It makes it hard to clear mucus out of your lungs and can cause frequent infections. Coughing a lot with pus and mucus is the main symptom. There isn’t a cure, but you can manage it with treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
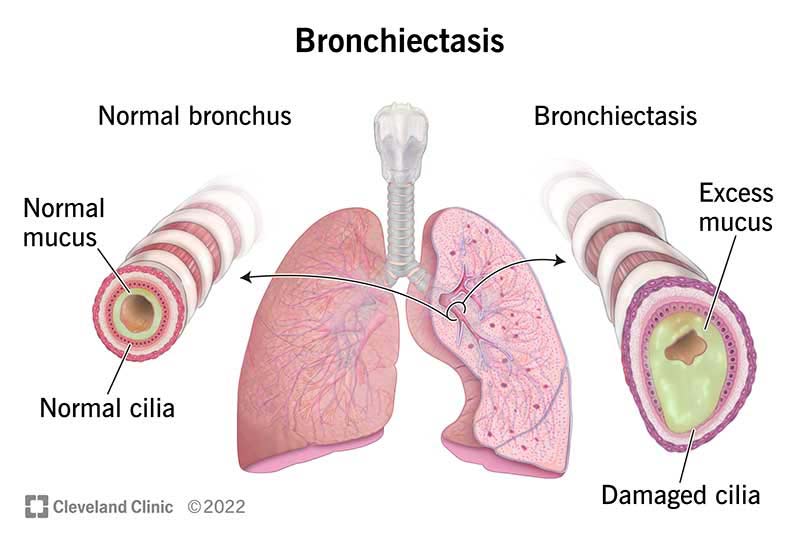
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21144-bronchiectasis)
Bronchiectasis is a lung condition where your airways get damaged and enlarged. Your airways are the tubes that carry air into your lungs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Damaged airways can’t clear mucus like they’re supposed to. Bacteria then grow in the mucus, causing more inflammation and damage to your lungs. This makes you cough a lot as your body tries to remove the infected mucus.
Bronchiectasis (“bronk-ee-EK-tuh-sis”) can be mild or severe depending on how damaged your lungs are. Some people have it and don’t even know it. Others have long-lasting symptoms, repeated infections and severe airway damage.
Healthcare providers describe bronchiectasis based on what the damage looks like and how widespread it is. Types include:
Advertisement
Bronchiectasis symptoms include:
You might have stretches of time where your symptoms aren’t as bad, then have a flare-up (exacerbation) where your symptoms get worse. Exacerbation symptoms include:
Airway damage causes bronchiectasis. Mucus in your airways is one way your body protects you from germs. Certain conditions make it so you can’t cough out mucus — and the bacteria trapped in it. This can cause lasting damage to your airways.
This damage happens in two phases:
Some of the specific causes of initial damage that start the cycle of bronchiectasis include:
It’s also associated with other pulmonary disorders, like asthma and COPD (chronic obstructive pulmonary disease).
In general, the risk of bronchiectasis increases as you get older. You’re also at a higher risk if you have an underlying condition that affects your lungs or immune system.
Damage caused by severe bronchiectasis can lead to life-threatening complications. These include:
Healthcare providers diagnose bronchiectasis by listening to your lungs and testing how well they’re working. If they think you have bronchiectasis or another lung condition, they’ll recommend imaging tests to take a closer look at your lungs.
A healthcare provider may do tests to diagnose bronchiectasis or rule out other conditions. These could include:
Advertisement
Healthcare providers treat bronchiectasis by clearing mucus and managing infections. Treatment options could include:
If an underlying medical condition is causing bronchiectasis, treating that condition may help your symptoms.
If you have bronchiectasis, contact your healthcare provider if you:
Advertisement
Go to the ER if you are:
Bronchiectasis can’t be cured — the damage it causes is irreversible. But most people can manage the symptoms by working together with their healthcare providers.
Your outlook will depend on how severe your condition is, how well you respond to treatment and what other health conditions you have. You may need to practice physical therapies or take medications daily. More severe cases may impact your quality of life.
You can reduce your risk of developing bronchiectasis by taking steps to protect your lung health:
Bronchiectasis and bronchitis have similar symptoms, including mucus in your lungs and coughing. But bronchiectasis causes permanent widening of your airways. Bronchitis is a temporary infection that doesn’t cause lasting damage.
Advertisement
Managing damage to your airways might seem overwhelming at first. But in most cases, bronchiectasis shouldn’t keep you from living a full life.
Talk to your provider about bothersome symptoms and how to deal with exacerbations. They may not be able to take care of every symptom, but sometimes small changes can greatly improve your quality of life.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Recurrent pneumonia, shortness of breath and coughing up mucus are three big signs of bronchiectasis. Cleveland Clinic is here to help you breathe easier.
