ECMO (extracorporeal membrane oxygenation) is a type of artificial life support that can help you if your lungs and heart aren’t functioning correctly. This process continuously pumps blood out of your body and sends it through a series of devices that add oxygen and remove carbon dioxide. The machine then pumps your blood back into your body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
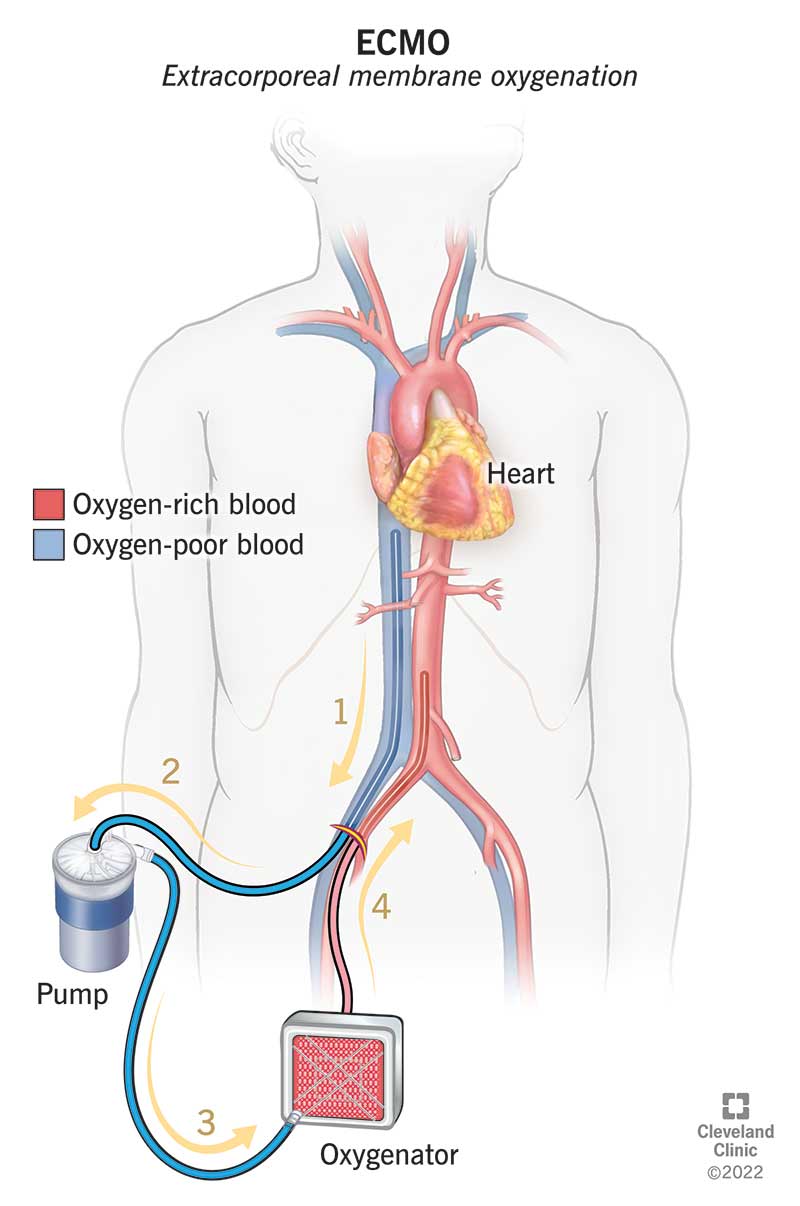
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21722-ecmo-illustration)
ECMO (extracorporeal membrane oxygenation) is a type of artificial life support. It can help you when your lungs and heart aren’t functioning correctly. An ECMO machine constantly pumps blood out of your body and then sends it through devices that add oxygen and remove carbon dioxide. It then pumps the blood back into your body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
ECMO stands for extracorporeal membrane oxygenation. Extracorporeal means “outside the body.” The rest of the name refers to getting oxygen to your body’s cells.
An ECMO procedure helps people who need support for their lungs or heart. But it can also bypass both organs. ECMO can make it possible for your heart and lungs to rest and heal from a respiratory infection, heart attack or trauma.
Healthcare providers consider ECMO a type of life support for people who need intensive or critical care. A ventilator is a type of life support, but it can only move air. It can’t add oxygen to and remove carbon dioxide directly from your blood. ECMO can exchange these gases like your lungs do.
Types of extracorporeal membrane oxygenation include:
Healthcare providers use an ECMO procedure for:
Advertisement
Providers used ECMO more than 21,000 times worldwide in 2024, according to the Extracorporeal Life Support Organization. About 600 hospitals worldwide can provide ECMO.
ECMO has helped many people in critical care units (CCUs) and intensive care units (ICUs) for decades. It’s also getting more use as an add-on to CPR. And critically ill people with COVID-19 have received this treatment.
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_k9uc7wot/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
When your heart and/or lungs stop working, ECMO provides a bridge to life support. Here’s how it works and why it’s needed.
During ECMO, blood flows out of your body through a tube in a large blood vessel in your chest, legs or neck. A pump pushes your blood through tubes that carry it to a machine that adds oxygen and removes carbon dioxide. Then, the ECMO machine pumps your blood back into your body.
A healthcare provider may refer to the process of placing these tubes as ECMO cannulation. You’ll be sedated, so you won’t feel the tubes going in. During extracorporeal membrane oxygenation, you may be awake or sedated.
An ECMO specialist will routinely check your heart and lung functions while you’re on ECMO to make sure you’re in good condition and there are no complications. This also lets providers know how much longer to keep you on ECMO.
Once you show signs of recovery, providers will begin weaning you off ECMO. In most cases, this process takes between two and five days. Then, a provider will remove the tubes and stitch the skin where the tubes were.
The length of time you spend on ECMO depends on why you need it. People can stay on extracorporeal membrane oxygenation anywhere from hours to days to weeks. The ECMO machine gives your lungs (and sometimes your heart, too) a chance to rest and recover. Meanwhile, healthcare providers treat the conditions you have.
An ECMO machine can be a lifesaving tool for people who are critically ill. It can support their lungs and heart, which can:
While an ECMO machine is a vital medical tool, it’s also one that has risks. Some of them are significant. The risks of extracorporeal membrane oxygenation include:
Advertisement
If your kidneys don’t get enough blood flow during ECMO, they can fail (stop working). A dialysis machine can take over your kidneys’ job for the short term. But you may need dialysis for the rest of your life. If you don’t have good blood flow to the leg where the ECMO machine connects, leg tissue can suffer. In rare cases, you may need surgery to fix this or remove part of your leg.
You can help a loved one by providing simple comforts. Just check with a provider to be sure it’s OK. You may:
The survival rate varies widely depending on the reason a healthcare provider uses ECMO. For example, anywhere from 4 to 8 out of 10 neonates may survive ECMO. Survival rates for babies with heart failure may be lower than for those with lung issues.
Researchers studying life expectancy after ECMO found that about 3 out of 10 adults lived five years after ECMO. Nearly 8 out of 10 people who survived the first 30 days lived another five years.
Healthcare providers use ECMO for people who have severe heart or lung problems when other treatments have failed. They use this treatment for conditions that can get better. But you can still die while on ECMO if providers can’t fix the condition you have.
Advertisement
There are several conditions or circumstances where ECMO isn’t an option. These include:
It may be difficult to see a loved one on ECMO or go through it yourself. But this decades-old treatment has helped many people who are critically ill with lung and heart problems. Modern medicine also has a better understanding today than ever before of how ECMO can help save lives. But it isn’t meant for everyone. Your healthcare provider can explain the potential benefits and risks and help you decide what’s best for you or your loved one.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Whether you need stitches, a broken bone set or think your appendix might be causing your abdominal pain, Cleveland Clinic’s emergency medicine team is here to help.
