Overview
A living donor transplant is a procedure during which a kidney is removed from a healthy donor and surgically placed in an individual with kidney failure. The living donor often is an immediate family member (parent, sibling, or child). The living donor can also be an uncle, aunt, cousin, or even a spouse or friend. Living donor kidneys can also come from strangers, Good Samaritans, that want to help someone in need of a kidney.
A living donor transplant has many advantages over a deceased donor kidney transplant, the most important being a significantly higher success rate. Additional reasons include:
- A kidney from a living donor generally functions immediately after transplant. A deceased donor kidney might take several days or weeks to function normally.
- The living donor transplant can be scheduled, allowing the recipient and donor preparation time. Recipients will not know when a deceased donor kidney will be available, and surgery must be performed very soon after it is available.
- There may be a reduced risk of rejection, especially if the kidney is donated by a blood relative.
- A living donor transplant can shorten the amount of time a recipient has to wait to receive a kidney transplant. The average wait time for a deceased donor kidney could be three to five years.
Interested in becoming a Living Donor?
Get started today by filling out our confidential online health questionnaire.
Frequently Asked Questions
Who would be a good living donor candidate?
Biological siblings generally make the best living donors due to matching. However, with the advancements in drugs and treatment for rejection prevention, anyone can be considered a donor if they have a compatible blood type. Most healthy individuals ages 18 and over are potential donors. All living donors are evaluated individually. You should discuss donation with immediate and extended family members, friends, co-workers, and friends of friends. The success of kidney transplants using unrelated living donors is nearly as high as living related donors.
What are the risks of having only one kidney?
A common question from a donor candidate is: “What if I get kidney disease later on in life?” A person with one kidney is no more likely to get kidney disease than someone with two kidneys. Even if the most common forms of kidney disease were to occur, a person with one kidney has no major disadvantage because medical kidney disease attacks both kidneys simultaneously. After surgery, the donor’s remaining kidney will increase in size and function. The donor’s chance for a long, normal, and healthy life remains the same with one kidney.
Will the quality of life change for the donor?
Once the donor has healed from the surgery, the person should not experience a difference in energy level, ability to work, life expectancy, susceptibility to illness, sexual function, or feeling of health. Also, donation should not affect fertility. Many female kidney donors have had normal pregnancies after donation. Donors also might receive a certain amount of satisfaction knowing they were able to help save another person’s life. In addition, by giving one of his or her kidneys, the living donor has also made a deceased donor kidney available to another who might not have any other options.
Is the donor operation dangerous?
Kidney donor surgery is a very safe operation. As with any surgery, there is a risk of bleeding and infection. The most advanced surgical technique, laparoscopic nephrectomy, has reduced the hospital stay to one or two days, resulted in less pain and scarring, and has reduced full recovery time from eight to 12 weeks down to two to four weeks.
Who will pay the donor’s medical bills?
A donor candidate will undergo a complete evaluation to determine if he or she can safely donate a kidney. The recipient’s insurance company will pay for these costs. All costs associated with the donor’s operation and recovery will also be billed to the recipient’s insurance company.
Once a donor has recovered, he or she will be required to have a follow-up appointment at six months, one year, and two years. A donor also might incur costs of travel, lodging, meals, and other non-medical expenses. Donating an organ is covered by the Federal Medical Leave Act. However, the donor candidate should determine the impact donation will have on his or her work situation before committing to the operation.
Evaluation Process
If you are interested in being evaluated as a potential living donor, please contact the Living Kidney Donor office for additional information at 216.445.3150 or 800.223.2273 ext. 53150.
Living Kidney Donor Evaluation Process
Can I be a kidney donor?
Generally, any normal, healthy adult with two normal kidneys can be a kidney donor. Your blood type will be the main factor in determining who can receive your kidney.
What blood tests are performed to determine if I am a compatible kidney donor?
ABO blood type
First, a simple blood test is performed to determine your blood type and that of the recipient. Here’s how your blood type should be compatible with the recipient’s blood type:
- If you have blood type A, your recipient should have blood type A or AB.
- If you have blood type B, your recipient should have blood type B or AB.
- If you have blood type AB, your recipient must have blood type AB.
- If you have blood type O, you are a universal donor and can donate to someone of any blood type: A, B, AB, or O.
Tissue typing
Tissue typing is a blood test that evaluates the compatibility, or closeness, between your tissues and the recipient’s. A human lymphocyte antigen (HLA) blood test is used to determine tissue type and help ensure that you’re a good genetic match for the recipient. In an HLA blood test, the tissue typing lab can identify and compare information about you and your recipient’s antigens (the “markers” in cells that stimulate antibody production) so they can match your kidney to the recipient.
While biological siblings (brothers and sisters) have the best chance of being a perfect match (six of six antigens), advancements in anti-rejection medicines have greatly reduced the occurrence of rejection in kidneys from unrelated donors. Researchers are also making strides in the development of treatments that will significantly increase the donor success rate when tissue doesn’t closely match.
Crossmatching
In crossmatching, your blood and the recipient’s blood are placed together in a test tube and examined to see if there is cell damage. If all your cells survive, there is a negative crossmatch, which is considered a good result. If your cells begin to die, a positive crossmatch results and gives a preview of what might happen with a transplant. In this case, it may be determined that the risk of proceeding with the transplant would be too high.
After the blood tests, how will I be evaluated as a potential donor?
If the initial blood tests indicate you are a suitable match, and you decide you would like to proceed , we will arrange an extensive donor evaluation to ensure you are in normal physical and emotional condition, and to inform you about the risks and procedures of being a kidney donor.
The evaluation generally consists of two days of outpatient appointments and testing. The evaluation will consist of:
- Medical Evaluation
- Surgical Evaluation
- Psychosocial Evaluation
- Living Donor Education
- Financial Education
- Lab work
- EKG (electrocardiogram)
- Chest X-Ray
- 24 hour ambulatory blood pressure monitor
- CT Scan of the abdomen and pelvis
Based upon the physicians’ findings during the evaluation appointments, additional testing and consults may be needed. You will also be asked to update your health maintenance testing if needed:
- Pap test for women 18 years of age and older
- Mammogram for women 40 years of age and older
- Colonoscopy for both women and men 50 years of age and older
Information for Donors
Interested in becoming a Living Donor?
Get started today by filling out our confidential online health questionnaire.
Overview of the Surgery
Laparoscopic Donor Nephrectomy - A Minimally Invasive Kidney Removal
There is an ever-increasing demand for living kidney donors. Until recently, kidney donation from a living donor could only be accomplished through a surgical procedure called open nephrectomy (kidney removal). This procedure requires a large, muscle-cutting abdominal incision; removal of a rib; and a relatively longer hospital stay and recovery period. However, advances in laparoscopic surgery have made an advanced surgical procedure called laparoscopic donor nephrectomy possible. This procedure has significant benefits over the traditional open surgery for kidney donation.
Laparoscopy—also known as “keyhole surgery”—is a minimally invasive surgical procedure during which a special camera, called a laparoscope, is used to produce an inside view of the abdominal cavity. Surgeons use the laparoscope, which transmits a real-life picture of the internal organs to a video monitor, to guide them through surgical procedures. The laparoscope magnifies these images many times their actual size, providing surgeons with a superior view of the abdomen.
Laparoscopic nephrectomy is a minimally invasive procedure that uses a laparoscope to remove a kidney for donation. Laparoscopic kidney removal is considered minimally invasive because it only requires three or four small non-muscle-cutting incisions rather than one large muscle-cutting incision in the abdomen. (See figures 1 and 2.) During the procedure, carbon dioxide is passed through one of the incisions into the abdominal cavity to lift the abdominal wall away from the organs below, creating more operating space to perform the surgery. The pencil-thin laparoscope and surgical instruments are then inserted through the other incisions.
At the end of the procedure, the kidney is removed through a 7cm, non-muscle-cutting incision in the bikini area.
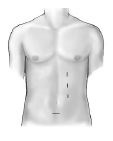
Figure 1: Positions of small incisions for laparoscopic donor nephrectomy surgery. No muscle is cut for any of these incisions.
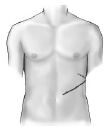
Figure 2: Muscle-cutting incision (6- to 10-inches long) used in traditional open nephrectomy surgery.
Frequently Asked Questions About This Surgery
What are the advantages of laparoscopic donor nephrectomy?
Because laparoscopic donor nephrectomy is a minimally invasive procedure, donor patients experience significantly less discomfort; have a shorter recovery period, and return to work more quickly than donors who had traditional open surgery. Because the incisions are small, laparoscopic donor nephrectomy causes reduced post-operative pain and shorter hospital stays, and patients experience a quicker return to normal eating habits and daily activities.
Who is a candidate for laparoscopic donor nephrectomy?
Most people who are eligible for open nephrectomy are also eligible for laparoscopic nephrectomy. However, you might not qualify for the procedure if:
- You have had multiple previous abdominal surgeries
- You are significantly overweight
- There is abnormal anatomy of the kidney
The surgeon will complete a pre-operative evaluation to ensure that laparoscopic nephrectomy is appropriate for you. However, in a small percentage of cases, even approved laparoscopic procedures might be converted to open procedures.
Paired Donation Program
Donors that are not matches to their intended potential transplant candidate have the option of participating in a paired donation program (where your donated kidney goes to a different recipient, and in return your recipient will receive a living donor kidney from another individual). Cleveland Clinic Kidney donors also have the option to donate to a stranger via our altruistic program.
Cleveland Clinic currently works with National Kidney Registry (NKR) to facilitate paired donor transplants. Altruistic living kidney donors can also be entered into the NKR program. National Kidney Registry is a nonprofit organization based out of Long Island that was established to expand the opportunities for living donor kidney transplants through paired donation. More information can be found on the National Kidney Registry website.
If you are interested in learning more about the paired donation or altruistic donation programs, please contact the Living Kidney Donor office locally at 216.445.3150 or toll-free 800.223.2273 ext. 53150.