Renal artery stenosis means the arteries that supply blood to your kidneys are too narrow. This limits how much blood can reach your kidneys. As the condition progresses, you may develop high blood pressure throughout your body and other complications. Treatments include medications, changes to your habits and procedures to improve blood flow.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
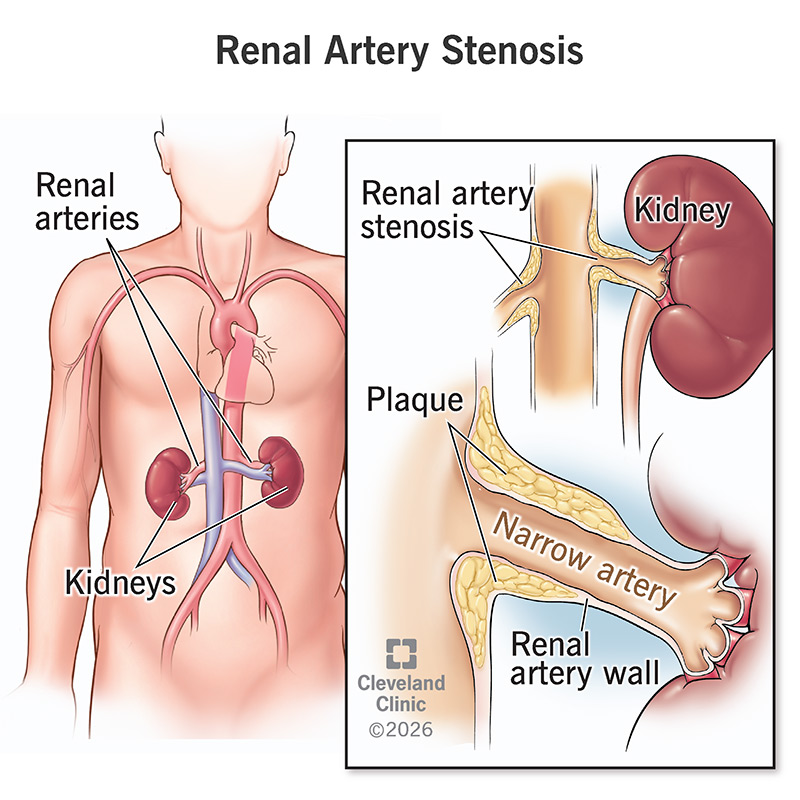
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/renal-artery-stenosis)
Renal artery stenosis, also called renal artery disease, is narrowing of the arteries that send blood to your kidneys. One or both of these arteries can grow too narrow, typically due to plaque buildup along the artery walls. As the artery narrows, there’s less room for blood to flow through and reach your kidneys.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
At first, your kidneys can adapt. But the narrowing may get worse over time and greatly reduce blood flow to your kidneys. This can lead to a range of issues, like high blood pressure and kidneys that are less able to filter waste out of your blood. Medications and changes to your daily habits are mainstays of treatment. Some people need a procedure to improve blood flow to their kidneys.
About 7 in 100 people over age 65 have renal artery stenosis. It’s more common among those who have peripheral artery disease (PAD) or congestive heart failure.
Most people don’t have symptoms of narrow kidney arteries. Rather, healthcare providers notice signs during physical exams and tests. The two main signs of renal artery stenosis are:
Symptoms you may develop from very high blood pressure or poor kidney function include:
Advertisement
The most common cause of renal artery stenosis is plaque buildup in your arteries (atherosclerosis), but some people develop it for other reasons. Here’s a breakdown:
Renal artery stenosis has the same risk factors as plaque buildup in arteries throughout your body. These include:
Many people who have renal artery disease also have plaque buildup in their heart arteries (coronary artery disease) and/or leg arteries (PAD).
Renal artery stenosis can lead to serious problems like:
You might hear your healthcare provider use the term “Pickering syndrome.” This refers to flash pulmonary edema and reduced kidney function that occur together as complications of renal artery stenosis.
Healthcare providers commonly diagnose renal artery stenosis when running tests for other reasons. For example, an imaging test of other blood vessels in your belly and upper legs may show narrowing of your kidney arteries.
Sometimes, providers notice clues that make them suspect renal artery stenosis. For example, a physical exam and review of your medical history may show:
These findings might mean that your renal arteries are narrowed and reducing blood flow to your kidneys. To learn more, your provider may run one or more tests, including:
These can show if your renal arteries are narrowed and, if so, how narrow they’ve become. They also help your provider learn how well your kidneys are working. The results guide treatment.
Advertisement
The most common treatments for renal artery stenosis are medications and changes to your daily habits. Some people need a minimally invasive procedure to widen their renal arteries and help blood reach their kidneys. Nowadays, open surgery is the least common treatment for this condition.
There’s no single medicine for renal artery stenosis. But healthcare providers commonly prescribe several different medicines that improve blood flow in all your arteries and lower your risk of complications. These include:
Your healthcare provider will likely recommend a variety of changes to lower your blood pressure and help your heart and blood vessels work at their best. They may advise you to:
You may need a procedure if your blood pressure is still too high despite taking medicines or if you develop other complications. Options include:
Advertisement
Your provider will tell you how often to come in for follow-up visits if you have renal artery stenosis. These are very important. Your provider will keep a close eye on your condition and look for signs of complications — like problems with your heart or kidney function.
Contact your provider if you have:
Advertisement
Call 911 or your local emergency services number if you have:
Renal artery stenosis is a condition that gets worse over time. Your healthcare provider will keep a close eye on how you’re feeling and run routine tests. Treatment can help slow the progression and lower your risk of complications.
Renal artery stenosis is the medical term for narrowed kidney arteries. If you have this condition, you’ll probably hear lots of other medical terms, too. These might feel confusing or, at times, scary. But think of this as a time to learn more about your body and your health. It may help to take notes at your appointments or bring a trusted friend or family member along.
There’s a lot you can do to manage renal artery stenosis — including small changes in your daily life. Each one adds up to make a big difference. Ask your provider which changes to start with. They’ll help you make a plan that feels doable.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Vascular disease may affect your life in big and small ways. Cleveland Clinic’s specialists treat the many types of vascular disease so you can focus on living.
