Pap smears are a lifesaving screening tool for cervical cancer. The test can detect abnormal cells in your cervix before they become cancerous. Healthcare providers often perform HPV tests during Pap tests to check for HPV, one of the leading causes of cervical cancer. An unclear or abnormal Pap smear result may be a sign of infection, another problem or cancer.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
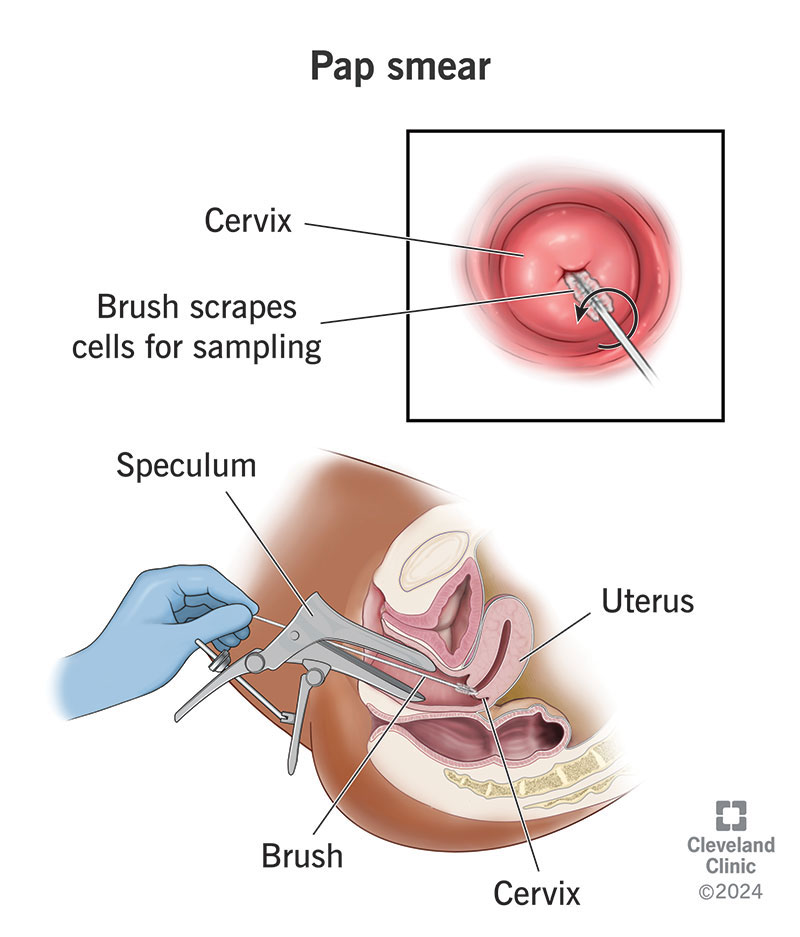
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4267-pap-smear)
A Pap smear (also called a Pap test) screens for cervical cancer. The test checks for abnormal cells on your cervix that are cancerous or have the potential to become cancerous and may also detect certain infections and inflammation. During a Pap smear, your healthcare provider takes cells from your cervix to examine under a microscope. The test is named for an American physician, Dr. George Papanicolaou, who developed the Pap smear.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Anyone with a cervix between the ages of 21 and 30 should get a Pap smear at least once every three years. Between the ages of 30 and 65, you should have one every five years. Healthcare providers consider a Pap smear to be the gold standard for preventing cervical cancer because it detects cervical cell changes before they can turn into cancer. Detecting precancerous or cancerous cells as early as possible typically increases your chances of beating the disease.
Going for your Pap test may feel like a nuisance, and you may dread going when the time comes. It’s easy to push the test off or think you don’t need to get one because your last one was fine, but it’s imperative for your reproductive health and putting it off could mean dangerous cell changes go unnoticed. Talk to your healthcare provider if you’re unsure when you’re due for your next Pap smear.
The test checks for:
A Pap smear can’t detect STIs like gonorrhea and chlamydia, but it may pick up things like trichomonas, bacterial overgrowth or yeast infections. Your provider performs gonorrhea and chlamydia tests separately from a Pap test.
Advertisement
During a pelvic exam, your healthcare provider examines and feels your uterus, ovaries and other parts of your reproductive system. A pelvic exam doesn’t always include a Pap smear, but a Pap smear almost always involves a pelvic exam.
HPV tests check for certain types of HPV that increase your cervical cancer risk. There are many different types of HPV. Not all cause cancer.
Providers can do HPV tests and Pap tests at the same time, using the same steps (a gentle scrape of your cervix for cell samples). When sending these samples to a lab, your provider specifies whether the lab specialist (pathologist) should check for precancerous or cancerous cells (Pap smear), HPV or both (a co-test). The time between tests is slightly different depending on whether you get just a Pap test or a co-test.
How often you’ll have the test depends on many factors, including your age, health history and results from your last Pap or HPV test. Most people don’t need Pap smears after age 65.
Generally, Pap smears occur:
| Age | Pap frequency |
|---|---|
| Younger than 21. | Not necessary. (Your risk for cervical cancer is very low before 21.) |
| 21 to 29 years old. | Every three years. |
| 30 to 65 years old. | Every three years with a Pap test alone or every five years with a Pap/HPV co-test. |
| Older than 65. | Not necessary if you’ve never had abnormal cervical cells or cervical cancer, and you’ve had three normal Pap test results in a row within the previous ten years. |
| Age | |
| Younger than 21. | |
| Pap frequency | |
| Not necessary. (Your risk for cervical cancer is very low before 21.) | |
| 21 to 29 years old. | |
| Pap frequency | |
| Every three years. | |
| 30 to 65 years old. | |
| Pap frequency | |
| Every three years with a Pap test alone or every five years with a Pap/HPV co-test. | |
| Older than 65. | |
| Pap frequency | |
| Not necessary if you’ve never had abnormal cervical cells or cervical cancer, and you’ve had three normal Pap test results in a row within the previous ten years. |
Certain factors may cause you to have more frequent screenings or screening past age 65. Some of these are:
It depends on what kind of hysterectomy you had and if you had it due to cancer or another condition:
People who had a hysterectomy due to ovarian, uterine or cervical cancer may still need Pap tests to check their vaginal tissue for signs of cancer. If you had a hysterectomy for a condition like uterine fibroids, your provider may decide your risk for cancer is low and you no longer need Pap smears.
Some things that you do in the days before a Pap smear can affect test results. For the most accurate results, you should:
It’s best to avoid having a Pap test while on your period as it could alter the results. Some healthcare providers will perform a Pap test at the end of your period (when bleeding is light). It’s best to check with your provider’s office to see what they recommend or reschedule your Pap for when you aren’t on your period.
Advertisement
A Pap takes place in your healthcare provider’s office. The appointment is quick, and the Pap test takes just a few minutes to perform. First, you’ll undress from the waist down or undress completely and put on a hospital gown. Then, you’ll sit on an exam table with your legs spread and your heels in stirrups. Your provider will give you a drape or paper sheet to place over your legs.
During the procedure, your healthcare provider:
A Pap smear shouldn’t hurt but may feel uncomfortable. You could experience light bleeding afterward, but you shouldn’t feel pain or cramping. Let your healthcare provider know if you feel discomfort lasting more than a few minutes or if the bleeding lasts longer than 24 hours.
Your healthcare provider will send the sample to a lab. A specialist called a pathologist examines the samples under a microscope to look for abnormal cells that may indicate cancer or HPV.
Advertisement
Pap smears are very safe and highly reliable. You may experience light bleeding after the test, but you shouldn’t have cramps or pain. There’s a small risk of false-negative or incorrect results, but this is rare.
It can take up to three weeks for your healthcare provider to receive the lab results. Your healthcare provider will let you know when to get your next Pap smear or if you need further testing.
When you receive your results, they may be:
Pap smears are a lifesaving screening tool. The test finds abnormal cervical cells before they have a chance to become cancerous. More than 95% of the time, people treated for precancerous cells don’t develop cervical cancer. An unclear or abnormal Pap test result doesn’t mean you have cervical cancer. Your provider can discuss test findings and the next steps with you.
Advertisement
If you have an abnormal Pap smear result, your healthcare provider will perform a procedure called a colposcopy. Some may choose to do another Pap smear to make sure the findings are the same.
Pap smears only screen for cancer — they can’t diagnose it. To get more information to help diagnose or rule out cervical cancer, your provider does a colposcopy. During this procedure, your provider:
Yes. Not all cervical cancers happen due to being sexually active. Even if you aren’t having sex, you still need a Pap smear if you’re 21 years old.
Yes, you can decline a Pap test. But studies continually show that getting a Pap test is the best way to prevent cervical cancer.
Since a Pap is the gold standard for detecting cell changes that could lead to cancer, not ever getting a Pap test means you could have cervical cancer and not know it. This could lead to cancer progressing and causing serious or life-threatening complications. Cancer is also much harder to treat once it begins to progress. Early detection is always best, and a Pap smear is how providers can detect cervical cancer as early as possible.
It’s common to dread getting a Pap smear. Most people don’t enjoy getting them, but they’re so important to your vaginal health. Luckily, Pap tests take less than 10 minutes and any discomfort you feel passes quickly.
Pap smears are a critical tool for detecting irregular cells in your cervix that may lead to cervical cancer. Check with your healthcare provider if you’re between 21 and 65 to make sure you’re up to date on your Pap smears. Early detection of precancerous or cancerous cells on your cervix can increase your chances of fighting cervical cancer.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Routine screening tests like Pap smears are an important part of your health. Cleveland Clinic’s providers can help you stay healthy with routine Pap smears.
