Acute respiratory distress syndrome (ARDS) is a life-threatening lung injury caused by sepsis, pneumonia, COVID-19 and other conditions. ARDS tends to develop within a few hours to few days of the event that caused it, and can worsen quickly. People with ARDS may have to be put in an intensive care unit (ICU) and on a ventilator to help them breathe.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
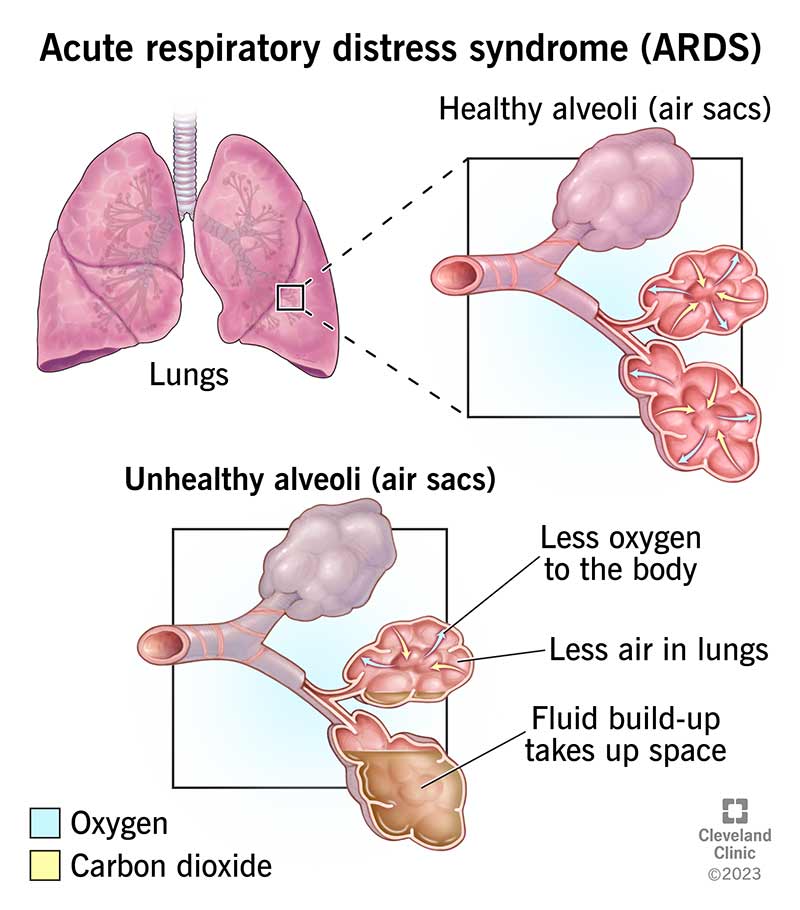
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/acute-respiratory-stress-syndrome)
Acute respiratory distress syndrome (ARDS) is a lung injury that happens when fluids build up in small air sacs (alveoli) in your lungs. ARDS prevents your lungs from filling up with air and causes dangerously low oxygen levels in your blood (hypoxia). Healthcare providers typically diagnose a person as having mild, moderate or severe respiratory distress syndrome. They determine that level by comparing the level of oxygen in your blood with the amount of oxygen that needs to be given to achieve a healthy blood oxygen level.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
ARDS prevents other organs such as your brain, heart, kidneys and stomach from getting the oxygen they need to function. ARDS is dangerous and can lead to several serious and life-threatening problems.
ARDS typically happens when a person is in the hospital receiving treatment for an infection, illness or trauma. If you’re not hospitalized and experience symptoms of ARDS, get medical attention immediately.
Healthcare providers sometimes classify ARDS into three stages: exudative, proliferative and fibrotic. This classification mainly describes the level of inflammation and fluid buildup, and the subsequent repair process that your lungs go through to heal. Not all people progress to the third stage, which mainly describes the formation of scar tissue in your lungs and a prolonged need for ventilation.
ARDS affects about 200,000 people in the United States and 3 million people worldwide every year. ARDS causes around 10% of all intensive care unit (ICU) admissions . It’s the reason at least 25% of people require mechanical ventilation in a hospital setting.
Symptoms of ARDS depend on the cause and severity of the case, as well as preexisting lung or heart conditions. Symptoms include:
Advertisement
ARDS tends to develop within a few hours to a few days of the event that caused it. ARDS can worsen rapidly.
Causes of ARDS include:
People who are already in the hospital due to an injury or illness are most at risk for ARDS. But, just because you’re hospitalized, doesn’t mean you’ll end up in respiratory distress. Some factors that can increase your risk include:
Complications and problems from ARDS may develop while you’re in the hospital or after you go home, like:
Healthcare providers diagnose ARDS based on a physical exam and the results of several tests. Since the symptoms of ARDS are similar to chronic lung or heart conditions, your provider may need to rule out other causes.
A healthcare provider may order a combination of tests, including:
Advertisement
Treatment for ARDS involves increasing oxygen levels in your blood to prevent organ failure. People with ARDS need a mechanical ventilator and/or oxygen therapy to improve blood oxygen levels. They also need help to open up the airways that have closed due to damage.
Your healthcare provider may take steps to minimize complications from ARDS. These include:
It depends on how severe it is and how long it takes a person’s lungs to heal. Most studies estimate it takes between six months to a year, on average, for a person to regain their usual lung function after ARDS. But some people don’t regain full lung function.
Survival rates for ARDS are around 55% to 70% when treatment is prompt. If treatment is delayed or other organs begin to fail, survival rates are lower.
Advertisement
Factors like the underlying medical conditions, health history and how severe the respiratory distress is all go into determining the outlook. Your healthcare provider will tell you what to expect.
ARDS can be life-threatening and scary. But improved care and ventilator treatments — including having people lay face down (prone) to improve oxygen flow — are helping more people survive and reduce ARDS complications. The outlook is typically better in people younger than 65 and when trauma or a blood transfusion causes ARDS.
Recovery from ARDS may take a long time. Most people who are taken off a ventilator can breathe freely. Some recover completely, but others may develop chronic lung problems that require care by lung specialists (pulmonologists).
Yes, your lungs can recover from ARDS. The exact amount of time varies depending on how much lung damage you have. Most people regain their lung function within two years, although several factors go into that estimate.
There’s no way to prevent acute respiratory distress syndrome (ARDS). But you may be able to prevent it from being severe by seeking immediate medical attention if you have symptoms of respiratory distress, or if you have a lung injury or other disease. You can lower your risk of getting severe ARDS by quitting smoking and avoiding alcohol.
Advertisement
Life after ARDS can be challenging. Have patience with yourself as you navigate recovery and lean on friends and family members for support. You may need help performing everyday tasks while your lungs regain function. Talk to your healthcare provider about support groups or other resources available to help you get your strength back.
Most people who have ARDS are already in the hospital due to an injury or illness. A healthcare provider is usually already checking on you and monitoring your vital signs. It’s important to share all your symptoms with your providers. If you ever experience symptoms of ARDS and aren’t in a hospital, contact 911, or your local emergency services, immediately.
No, they aren’t the same. People with COVID-19 can develop ARDS when the virus gets into their lungs.
Researchers are always learning more about the COVID-19 virus. Most studies conclude that the survival rate for a person with both COVID-19 and ARDS is about 50% to 60%. But many factors go determining if a person survives ARDS and COVID-19, including health history and other medical conditions.
Time in the ICU can be traumatic and hard. People recovering from ARDS may not be able to go back to everyday life quickly, and you’ll need support. Getting professional help and advice is important along the road to recovery from ARDS. Ask your healthcare team about any post-intensive care recovery programs in your area and online support groups that are available.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Breathing issues can affect your life in many ways. Cleveland Clinic’s respiratory therapy program treats your symptoms so you can feel better day to day.
