A tilt table test shows how your body responds to standing up after lying down. It does it in a safe way, with fabric straps keeping you from falling if your blood pressure drops. Healthcare providers monitor your vitals while the table you’re on tilts at various angles. This allows them to find out why you faint.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
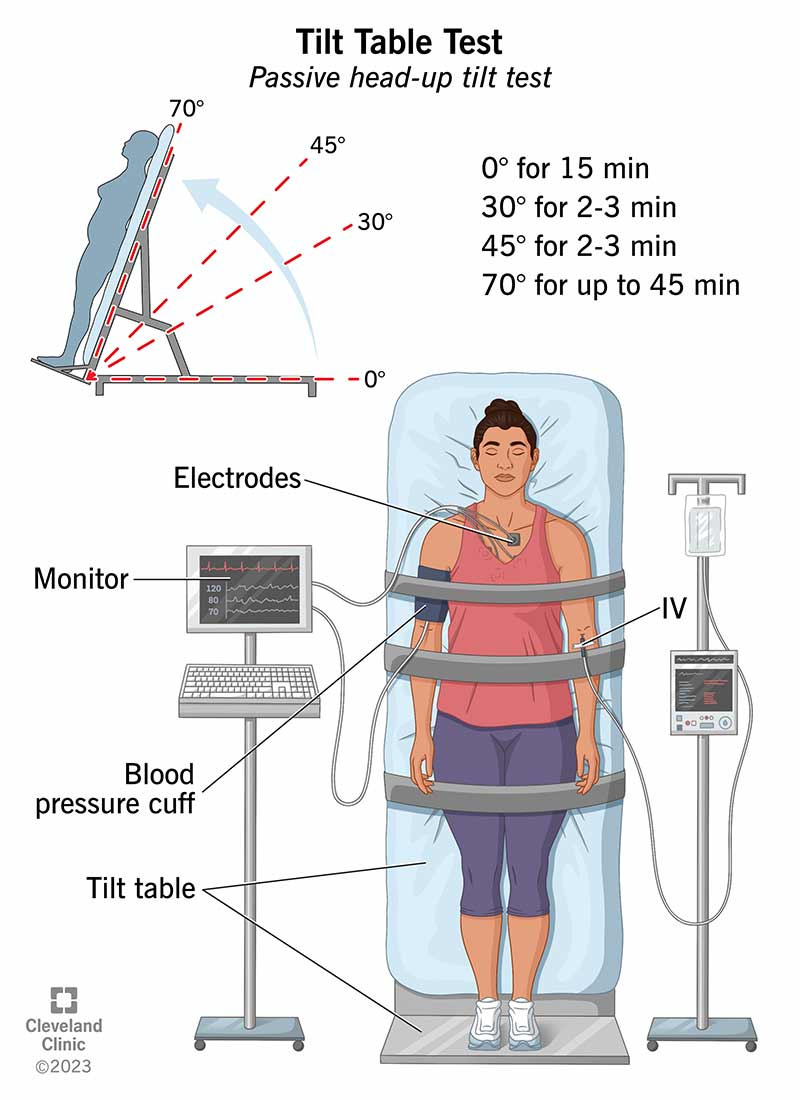
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17043-tilt-table-test-illustration.ashx)
The tilt table test (also called a “passive head-up tilt test” or “head-upright tilt test”) is a test healthcare providers use for people who faint. It records your blood pressure, heart rhythm and heart rate on a beat-by-beat basis when the table you’re on tilts at different angles. The table always stays head-up.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A tilt table test shows how different positions affect your heart rate, heart rhythm and blood pressure. A healthcare provider uses this information to find the cause of symptoms like lightheadedness and fainting spells (syncope) and develop the best treatment plan for you.
Fainting or syncope is a brief loss of consciousness and posture (which is why it makes you fall) that happens because of a temporary decrease in blood flow to your brain. This decrease can happen because of a sudden drop in your blood pressure or heart rate or changes in the amount or movement of blood in your body. You may be confused for a bit after you become conscious again.
Whether you’re standing, sitting or lying down, your body should automatically manage your heart rate and blood pressure. However, certain conditions can get in the way of that process. When that happens, your blood pressure may drop suddenly when you stand or sit up too fast.
Syncope often happens because of other medical conditions that may involve your heart, nervous system or blood flow to your brain.
Your provider may also order other tests to get a better understanding of your condition.
A tilt table test imitates what happens in your body when you stand up after lying down. It changes your body’s position in a safe way because straps keep you from falling if you faint when you move to a standing position.
Advertisement
A provider performs a tilt table test to find the reason why you get lightheaded or pass out for an unknown reason.
Healthcare providers perform tilt table testing in a hospital or clinic that has a tilt lab or electrophysiology lab.
The test takes about 90 minutes if you complete both parts of it. It may take only 30 to 40 minutes, depending on your symptoms and the way the test affects your blood pressure, heart rhythm and heart rate. Some people only need the first part of the test because they get symptoms during that part. When that happens, providers have the information they need without going further.
Review your provider’s instructions ahead of time so you’ll know what to do on the day of your test. Ask a friend or relative to go with you so they can drive you home after your test.
Eat a normal meal the evening before your procedure.
Don’t eat or drink anything except small sips of water for four hours before the test.
Don’t eat or drink anything that contains caffeine on the day of the test.
Take your prescription medications as you normally would, with small sips of water.
If you take a diuretic (“water pill”), ask your healthcare provider if you can wait until after the test to take it.
Don’t take a laxative.
If you have diabetes or take insulin, ask your provider how to take your medications on the day of your test. Bring your glucose meter to check your sugar if it feels low on your way to the hospital.
Don’t stop taking any medication without first talking to your healthcare provider.
Wear comfortable clothes and shoes. You may wear a short-sleeved or sleeveless T-shirt in place of a hospital gown. If you’re wearing a long-sleeved or tight-fitting shirt, you may need to change into a hospital gown for the test. You may want to bring a change of clothes in case you vomit or pee during the test.
Don’t bring valuables.
Bring:
A provider will explain the details of the test, answer your questions and ask you to sign a consent form. You may sign the consent form during a visit before the day of your test. A provider will help you get ready for the test and answer any questions you have.
Before your tilt table test, let your provider know if they need to avoid using one of your arms for an IV or blood pressure readings.
Advertisement
Before your tilt table test, a provider will:
Healthcare providers will be with you throughout your tilt table test. They’ll try to keep you as comfortable as possible. Machines will constantly monitor your blood pressure, heart rhythm and heart rate throughout the test. A computer will store the collected information.
Advertisement
During a tilt table test, you’ll rest for 15 minutes.
Then, as you lie still, a provider will record your blood pressure and EKG.
A provider who controls the motorized table will tilt it:
You’ll always be upright during the test.
For the most accurate test results, follow these directions:
Stay as still and quiet as possible during the test.
Don’t move your legs while you’re in the standing position.
Try not to talk unless you need to.
Tell a provider about symptoms you have during your tilt table test.
If your blood pressure doesn’t fall during the first part of the test, a provider may give you medicine to see if your body reacts to it. The medicine makes your heart beat faster. You may get the medicine through your IV or as a pill or spray in your mouth.
After you receive the medicine, a provider will tilt the table to 60 degrees for up to 15 minutes. If your blood pressure goes down during this time, it’s the end of the test. Either way, you’re done in 15 minutes with the second part of the test.
A provider will ask you how you feel throughout the test. You may not have any symptoms, or you may have pre-syncope symptoms. These can include, but aren’t limited to, feeling:
Advertisement
You also may have blurred vision or a headache.
The purpose of the test isn’t to make you faint. However, you may faint, depending on how you respond to the test.
It’s important to tell a provider how you feel throughout your test. They may ask you to rate your symptoms on a scale of 1 to 10, with 10 being the most severe. Your symptoms, along with the information providers collect during the test, help them figure out what’s making you faint.
Tell a provider if you feel like you can’t continue the test because of symptoms you have. They can stop the test if they have to. But, if they feel you can safely continue the test, they’ll encourage you to so they can get the most complete results possible.
After your tilt table test, a provider will lower the table to a flat position. You’ll stay on the table for 5 to 10 minutes as you lie flat. This allows providers to make sure you're OK and measure your blood pressure, heart rate and heart rhythm.
It’s rare for severe symptoms to continue after the test. But if this happens, you may need an evaluation in the emergency department.
If the tilt test is the last test of the day, a provider will remove your IV. If you have other tests that day that require an IV, they may leave your IV in place. Another provider will remove your IV after your final test.
Most people can go home after their test. A responsible adult must drive you home after your tilt table test. You won’t be able to drive for the rest of the day.
You can eat normally after the test unless you have other tests scheduled that require you to fast.
Report any symptoms or side effects that are new or continue after the test.
Rarely, people faint during tilt table testing. Because providers are with you, they can put the table back down so you recover quickly. You also may feel tired and/or have an upset stomach. Some people can’t control their bladder and release urine (pee) when they faint.
Yes, tilt table tests are safe. However, all tests and procedures carry some risk. Very rarely, people with narrowed coronary arteries or carotid arteries may have heart attacks or strokes.
Your healthcare provider will talk to you about the risks and benefits of the tilt table test before you agree to have the test. A provider can modify the test if they need to in order to reduce your risks.
A positive tilt table test means you may have a condition that causes an abnormal change in blood pressure, heart rate or heart rhythm.
A negative tilt table test means that there were no signs of a condition that causes an abnormal change in your blood pressure, heart rate or heart rhythm.
Conditions that can cause a positive tilt table test include:
A provider will review the results and may talk to you about them if:
If a provider from the tilt table testing lab doesn’t discuss your results with you after your test, call your referring provider to discuss test results. You’ll most likely get results in a few days if you don’t get them right away.
Depending on the results of the tilt table test, you may need more tests to determine the cause of your syncope. These tests can include:
Your referring provider will explain the test results to you and talk to you about your plan of care.
It’s important to ask your provider about medications. You may need to make changes to the types or amounts of medications you take. Follow the new treatment plan your provider prescribes.
Fainting can make you feel afraid to be alone or go anywhere. Providers have been using the tilt table test for decades to get the information they need to find out what’s making people faint. Once they know the cause, they can make a treatment plan to help you.
Learn more about the Health Library and our editorial process.
Cleveland Clinic's health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability, and up-to-date clinical standards.
Cleveland Clinic's health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability, and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
