Calcinosis cutis happens when calcium salts build up in your body and form growths on and under your skin. There are five types with varying causes. Some are mild. Others can be severe and cause serious complications. A healthcare provider will help you understand which type you have, what’s causing it and how you can manage it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
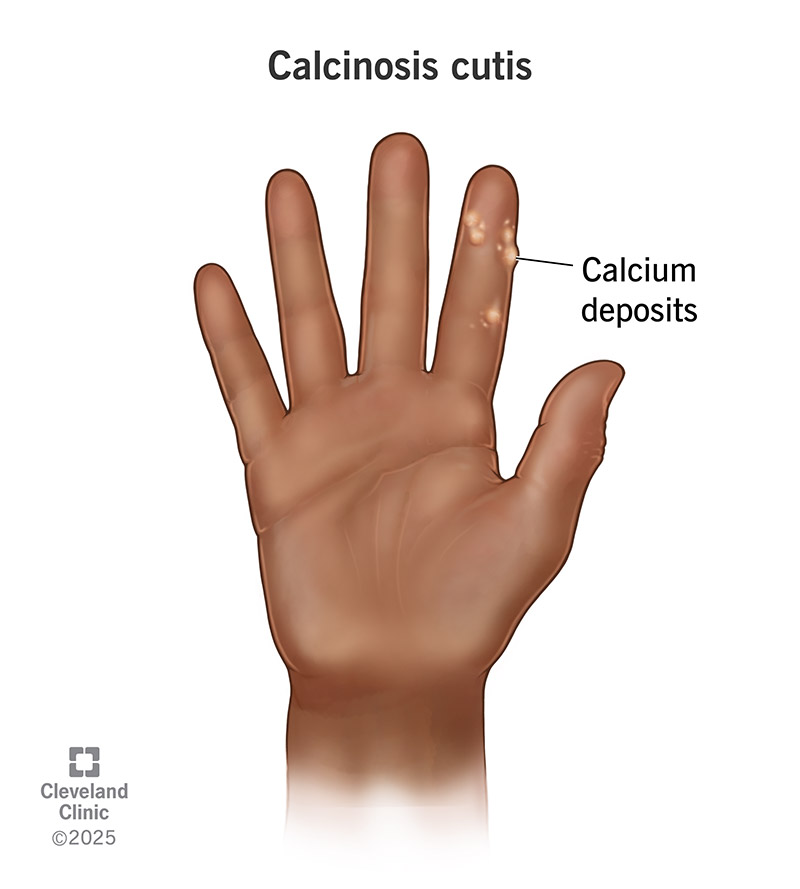
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/calcinosis-cutis)
Calcinosis cutis is a condition that happens when yellowish or white calcium deposits form on and under your skin. They can develop anywhere, but they’re most common near your:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The calcium deposits may not cause any problems. Sometimes, they go away on their own. But in some cases, they can affect how well your body functions. This can lead to serious complications, especially if they develop in your blood vessels. Visit a healthcare provider if you notice any new skin growths.
The growths on your skin are the most noticeable symptom. You may only have one. But it’s more common to have several. These growths can:
Calciphylaxis, one type of calcinosis cutis, causes purple or red lesions and patches. These are usually very painful, especially when you touch them.
Several issues can cause calcinosis cutis, including:
There are five types of calcinosis cutis. Some have more specific causes than what’s listed above. The five types include:
Advertisement
In severe cases, the growths can lead to gangrene. This can be fatal if it’s not treated right away. Calciphylaxis can also be fatal if the lesions break open and you develop an infection that spreads to your organs.
A healthcare provider will diagnose calcinosis cutis with a physical exam and tests. Your provider will look at any growths on your skin. Tell them when you first noticed any changes and if you’ve had any other symptoms.
Talk to your provider about your health history. Let them know if you have any conditions, which medications you’re taking and if you’ve had surgery recently.
Your provider will order blood tests to check your calcium and phosphate levels. These tests can also show signs of other issues that can cause calcinosis cutis. You might need some other tests, too, including:
Your healthcare provider will recommend treatments for the underlying cause of calcinosis cutis, if there is one. That can help reduce how fast the growths in your skin form.
Your provider may recommend medications to manage calcinosis cutis, including:
Not all types respond well to these treatments, so they may not be what’s best for you.
You may also need to make some tweaks to your daily routine to improve your circulation. This can help fresh blood get to all parts of your body and improve how well calcinosis cutis treatments work. You may want to:
Advertisement
A surgeon can remove larger lesions, especially if you have a higher risk of complications. There are a few surgical techniques. Your surgeon will tell you which one they suggest based on your unique needs.
Visit a healthcare provider if you notice new growths or changes in your skin, especially if the growths hurt or leak fluid. Talk to a provider if it’s harder to move or use part of your body, too.
Also, let your provider know if it seems like your treatments aren’t working as well as they used to. Or if you notice new lesions forming faster than in the past.
What you can expect depends on a few factors, including:
Some types don’t cause symptoms and may even go away on their own. Others may get better with medication. But you may need to keep taking your medicine for months or years to keep the condition from coming back.
Calciphylaxis usually happens during end-stage kidney failure. That’s part of why it can be life-threatening. Talk to your healthcare provider about what to expect.
Advertisement
Anything that causes visible changes to your skin can be stressful. And calcinosis cutis is no different. No matter which type you have or what causes it, see a healthcare provider as soon as you notice any new growths on or under your skin. They’ll help you understand what they are and how you can manage them.
There are lots of medications that may help. But it can take time to find the ones that are right for you. Talk to your provider about what’s working and what isn’t. Never be afraid to share feedback or ask questions. You know your body better than anyone, and you know when something doesn’t feel right. They’ll help you find the best options.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From sudden injuries to chronic conditions, Cleveland Clinic’s orthopaedic providers can guide you through testing, treatment and beyond.
