Post-traumatic stress disorder (PTSD) is a common mental health condition that can develop after a traumatic event. It involves symptoms like flashbacks, anxiety, negative thoughts and beliefs, hypervigilance and more. The main treatment for PTSD is psychotherapy (talk therapy).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
PTSD (post-traumatic stress disorder) is a mental health condition that some people develop after they experience or witness a traumatic event. The traumatic event may be life-threatening or pose a significant threat to your physical, emotional or spiritual well-being. PTSD affects people of all ages.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
People with PTSD have intense and intrusive thoughts and feelings related to the experience that last long after the event. PTSD involves stress responses like:
These symptoms cause distress and interfere with your daily functioning.
Trauma or a traumatic event is anything that severely threatens your existence or sense of safety. It doesn’t have to be a single event (like a car accident) — it can be long-term trauma like living through war or frequent abuse. Trauma also doesn’t have to happen directly to you — you could witness a traumatic event. In addition, you could develop PTSD after learning that a traumatic event happened to a loved one.
Examples of traumatic events include (but aren’t limited to):
Two conditions are closely related to PTSD:
Advertisement
PTSD is common. It develops in 5% to 10% of people who have experienced trauma.
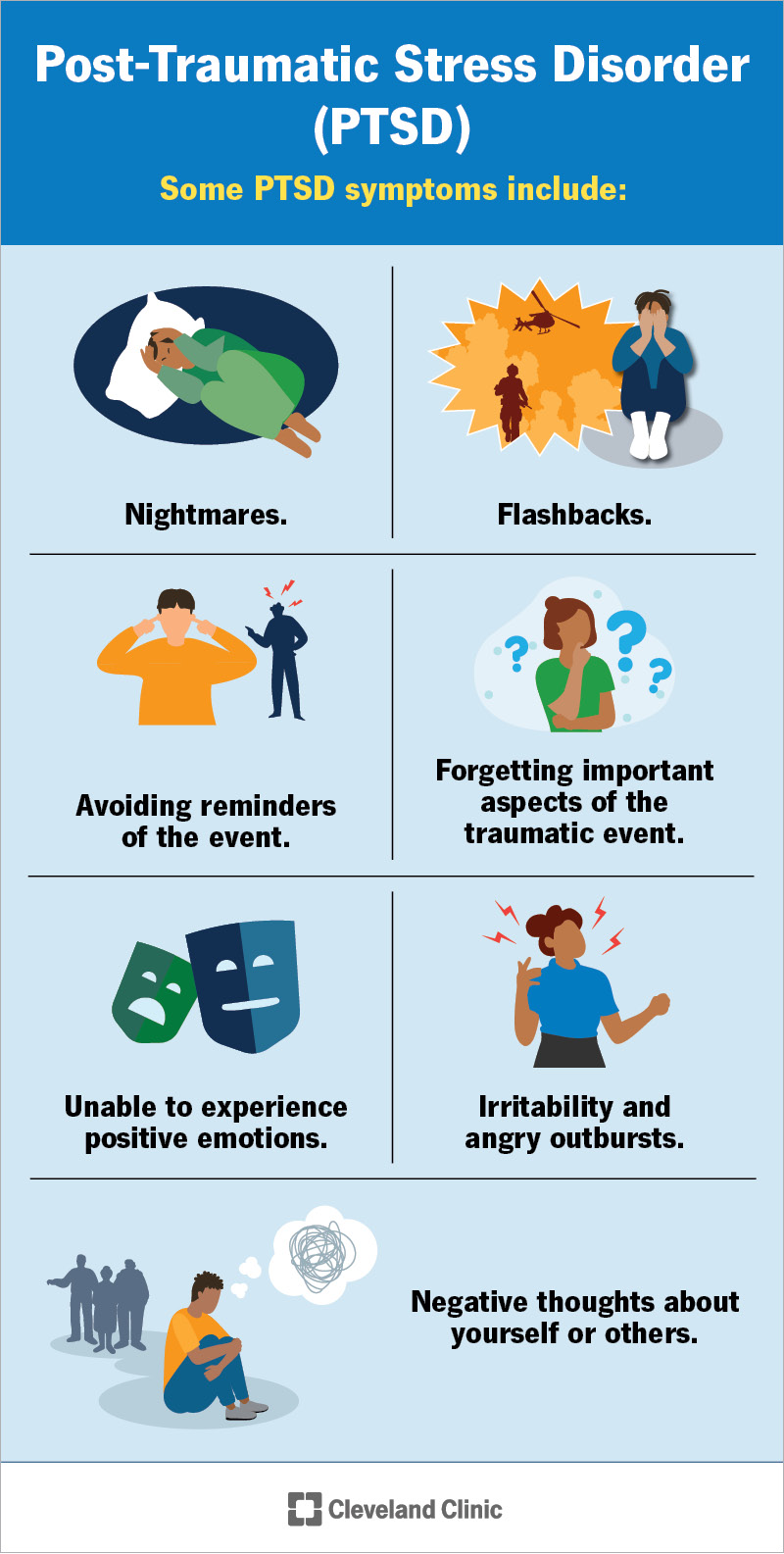
To receive a PTSD diagnosis, symptoms must last for more than a month and must cause significant distress or issues in your daily functioning. The symptoms of PTSD fall into four categories:
Intrusion:
Avoidance:
Changes in thinking and mood:
Changes in arousal and reactivity:
Children with PTSD may have difficulty expressing how they’re feeling or they may have experienced trauma that you don’t know about. They may seem restless, fidgety, or have trouble paying attention and staying organized.
These symptoms can be confused with symptoms of attention-deficit/hyperactivity disorder (ADHD). Because of this, it’s important to take your child to a specialist (like a child psychologist) who has experience in diagnosing PTSD.
The following conditions are common in people with PTSD, which can make PTSD symptoms worse:
People with PTSD also have an increased risk of suicidal thoughts and attempts.
If you or a loved one is thinking about suicide, call or text 988 to reach the Suicide and Crisis Lifeline. Someone is available to help you 24/7.
Approximately 61% to 80% of people experience a traumatic event at some point in their lives. PTSD develops in about 5% to 10% of this population.
It’s unclear why people respond differently to trauma. But studies show that people with PTSD have abnormal levels of certain neurotransmitters and hormones. They also experience brain changes.
Advertisement
Studies show that people with PTSD have normal to low levels of cortisol (the “stress hormone”) and elevated levels of corticotropin-releasing factor (CRF) despite ongoing stress. CRF triggers the release of norepinephrine, which leads to an increased sympathetic nervous system response. This “fight or flight” response leads to increased:
In addition, some studies show altered functioning of other neurotransmitter systems, including:
PTSD is associated with changes in the functioning and anatomy of your brain:
There’s no way to predict who will develop PTSD after a traumatic event. But PTSD is more common in people who have experienced:
Advertisement
There’s no test to diagnose PTSD. Instead, a healthcare provider makes the diagnosis after asking about your:
It may be difficult to talk about the trauma. You may want to bring a loved one with you to the appointment for support and to help provide details about your symptoms and behavior changes.
Providers use the diagnostic criteria for PTSD in the American Psychological Association’s Diagnostic and Statistical Manual of Mental Disorders (DSM-5). The latest version is the DSM-5-TR (“TR” stands for “text revision”). To get a diagnosis of PTSD, you must have had the following symptoms for at least one month:
Your provider may also perform a physical exam and order certain tests (like blood tests) to see if any physical conditions could be causing some of your symptoms.
Psychotherapy (talk therapy) is the main treatment for PTSD, especially forms of cognitive behavioral therapy (CBT).
This therapy takes place with a trained, licensed mental health professional, such as a psychologist or psychiatrist. They can provide support, education and guidance to you and/or your loved ones to help you function better and increase your well-being.
Advertisement
Specific forms of CBT for PTSD include:
Currently, there are no medications approved by the U.S. Food and Drug Administration (FDA) to treat PTSD. However, healthcare providers may prescribe certain medications to help certain PTSD symptoms, such as:
The prognosis (outlook) for PTSD can vary, but treatment often helps. With treatment, about 30% of people eventually recover from the condition. About 40% of people get better with treatment, but mild to moderate symptoms may remain. For some people, symptoms of PTSD go away over time with the support of loved ones and without professional treatment.
You can’t necessarily prevent a traumatic event. But some studies show that certain steps may help you prevent PTSD afterward. These are called “protective factors” and include:
It’s important to see your medical healthcare provider and/or mental health provider regularly following a traumatic event. If your symptoms get worse, call your provider.
If you’re experiencing thoughts of suicide or self-harm, it’s crucial to contact 911, go to the nearest emergency department or call 988 to reach the Suicide and Crisis Lifeline.
It may be very difficult to seek professional help following a traumatic event. Know that PTSD is treatable, and with time, treatment can help you feel better. Talk to your healthcare provider about therapy options and remember that they’re available to help and support you.
Your mental well-being is just as important as your physical well-being. Cleveland Clinic’s mental health experts can help you live life to the fullest.

Last reviewed on 10/06/2023.
Learn more about the Health Library and our editorial process.