Idiopathic intracranial hypertension (IIH) is increased pressure in your skull. It occurs because of cerebrospinal fluid buildup around your brain. The cause is unknown. It can affect your vision and cause headaches, nausea or ringing in your ears. Treatments are available.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Idiopathic intracranial hypertension (IIH), formerly known as pseudotumor cerebri, is increased pressure around your brain. It occurs when cerebrospinal fluid (CSF), the liquid that cushions your spinal cord and brain, builds up in your skull. Pressure builds up in your brain and on your optic nerve, the nerve at the back of your eye that helps you see.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The words within the condition name mean:
A former name for IIH is pseudotumor cerebri. Pseudotumor cerebri means “false brain tumor.” Providers used to call it this because the symptoms can be similar to a brain tumor.
Let a healthcare provider know if you notice symptoms like changes to your vision in addition to a headache or ringing in your ears. Treatment options are available for IIH.
IIH is rare. It affects an estimated .2 to 2 people (between ages 25 and 36) out of 100,000 in a general population study.
IIH isn’t life-threatening. However, symptoms can cause permanent vision changes that can affect your quality of life. A healthcare provider can quickly treat this condition to prevent complications.
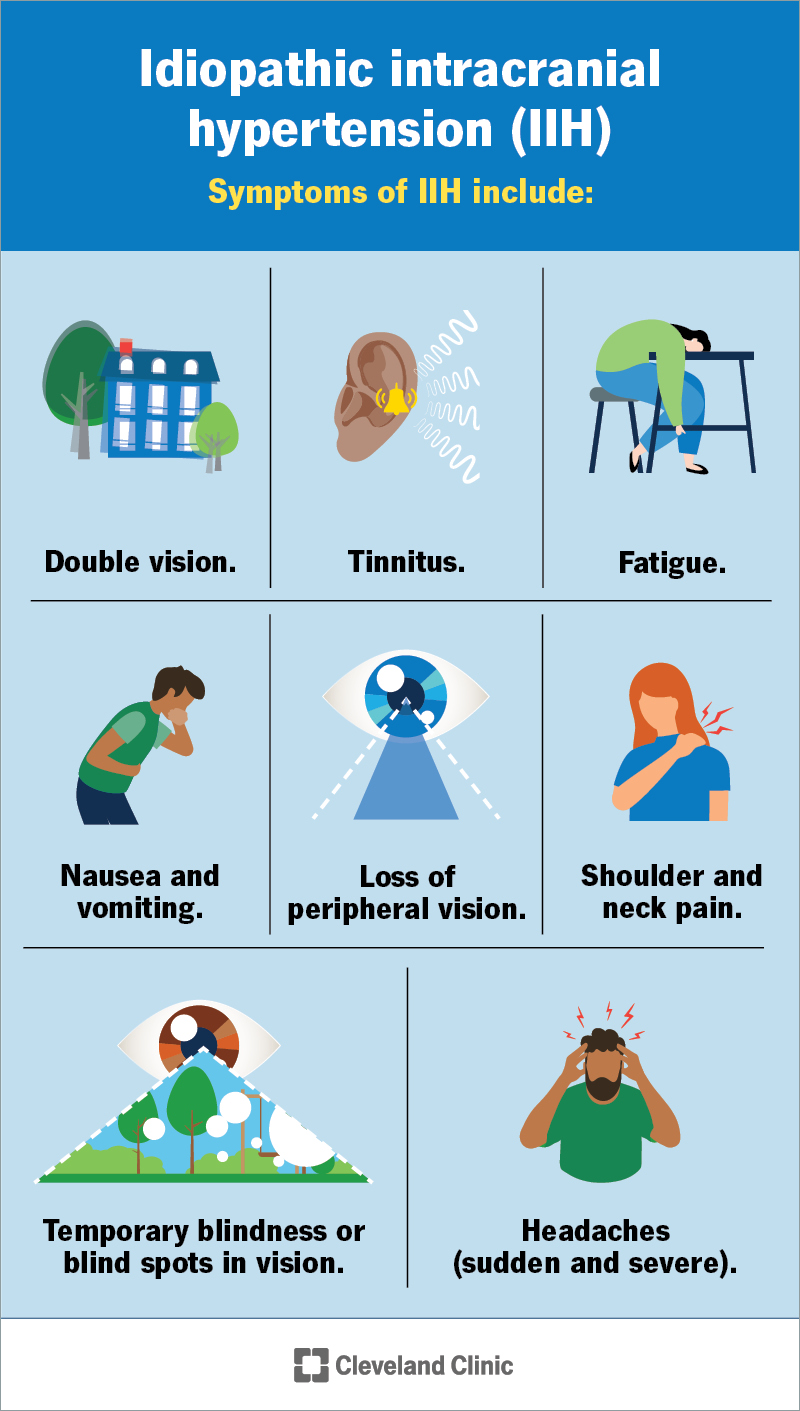
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/idiopathic-intracranial-hypertension)
Symptoms of IIH include:
Several conditions can cause these symptoms, so check with a provider to find out if these symptoms are related to IIH or something else.
Healthcare providers don’t know the exact cause of IIH. “Idiopathic” means that the cause is unknown.
Advertisement
Researchers theorize that there may be a blockage in the path cerebrospinal fluid uses to travel through your brain (CSF pathway) or a narrowing of large veins (venous sinuses) in your brain. This may cause fluid or blood to back up as it tries to exit your brain, which increases pressure.
Studies are ongoing to learn more about whether IIH is hereditary (runs in your biological family). Some people who have the condition report family members having it, too.
IIH can affect anyone. You may be more at risk of developing it if you:
IIH may lead to vision loss if untreated. This is irreversible. A healthcare provider can offer treatment options to prevent this complication, so let them know as soon as possible if you notice changes to your vision.
To diagnose IIH, a healthcare provider will take your medical history and perform a physical exam. They’ll learn more about what symptoms you experience and order several diagnostic tests to rule out conditions with similar symptoms. Tests may include:
The goals of IIH treatment are to decrease pressure on your brain and prevent vision loss. Depending on the severity, your healthcare provider may recommend:
Your provider will determine what type of treatment is best by reviewing diagnostic test results. They’re looking for areas of your brain where there may be problems with cerebrospinal fluid movement or blood flow. They’ll also assess the severity of your condition. Severe cases may require surgery to prevent permanent vision loss.
Some medicines can help you manage IIH symptoms. Your provider may prescribe:
Let your healthcare provider know if you’re pregnant, plan on becoming pregnant or take birth control pills. They may offer alternatives for acetazolamide and topiramate due to potential side effects.
In severe cases, you may need surgery for IIH. Surgical options could include:
Advertisement
To prevent IIH from happening again, your provider may suggest making lifestyle changes to improve your overall health. This could include participating in a weight management program if you have a BMI over 30.
Researchers suggest that excess body fat in your chest and abdomen creates pressure that makes it harder for blood from your brain to reach that area. As a result, fluid can collect in your brain and increase your risk of IIH.
Timely treatment at the first sign of vision changes or symptoms can help reduce your risk of complications like permanent vision loss. Treatment is often successful at relieving symptoms. Your healthcare provider can give you the best information on what you can expect in your situation.
Your provider and ophthalmologist (eye doctor) will want to schedule regular check-ups to monitor your health after you receive an IIH diagnosis.
IIH doesn’t directly affect your life expectancy. Most people have a normal life expectancy.
There isn’t a cure for IIH, so you may have to manage this condition for the rest of your life.
This condition may return in the future. It’s important to follow your treatment plan, especially if your provider recommends making changes to the foods you eat or your activity level to help reduce your risk.
Advertisement
You can’t prevent IIH because the cause isn’t well understood. You can help reduce your risk of developing the condition by maintaining a healthy weight that’s appropriate for you. A healthcare provider can help you manage any risk factors for IIH, too.
Let a provider know if you notice symptoms of IIH (like a headache or ringing in your ears) with changes to your vision. This could include:
Even if these happen for a moment and your vision returns to normal soon after, discuss your symptoms with a provider.
You may also want to ask your provider:
It can be frustrating to receive a diagnosis for a condition with an unknown cause. After running some tests, your healthcare provider may suspect where fluid might be backing up, but this isn’t the case for everyone. Even though it may seem like there aren’t any answers for idiopathic intracranial hypertension (IIH), you can still ask questions to learn more about what’s going on inside of your body. Your care team is available to help you understand what you need to do to maintain your health. In the meantime, get regular eye exams and let your provider know if you notice any changes to your vision.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
