Aicardi syndrome is a rare condition that affects your child’s brain and eyes. Seizures are a common symptom. It also causes developmental delays and intellectual disability. Research suggests it’s an X-linked genetic condition, as it mostly affects females. Aicardi syndrome may lead to a shortened life expectancy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Aicardi syndrome is a rare, present at birth condition that affects your child’s brain and eyes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The three most common features of Aicardi syndrome are:
This is a life-threatening condition. Severe cases may affect your child’s life expectancy, but not all cases are severe. Your child will still be able to play, laugh and enjoy their childhood, even if it’s shorter than others. Your child’s provider will let you know what to expect for their situation, as it’s as unique as they are.
Your child will also build a close relationship with their providers, as they’ll need lifelong care and support. Resources are also available for parents and caregivers to help navigate your child’s needs as they grow.
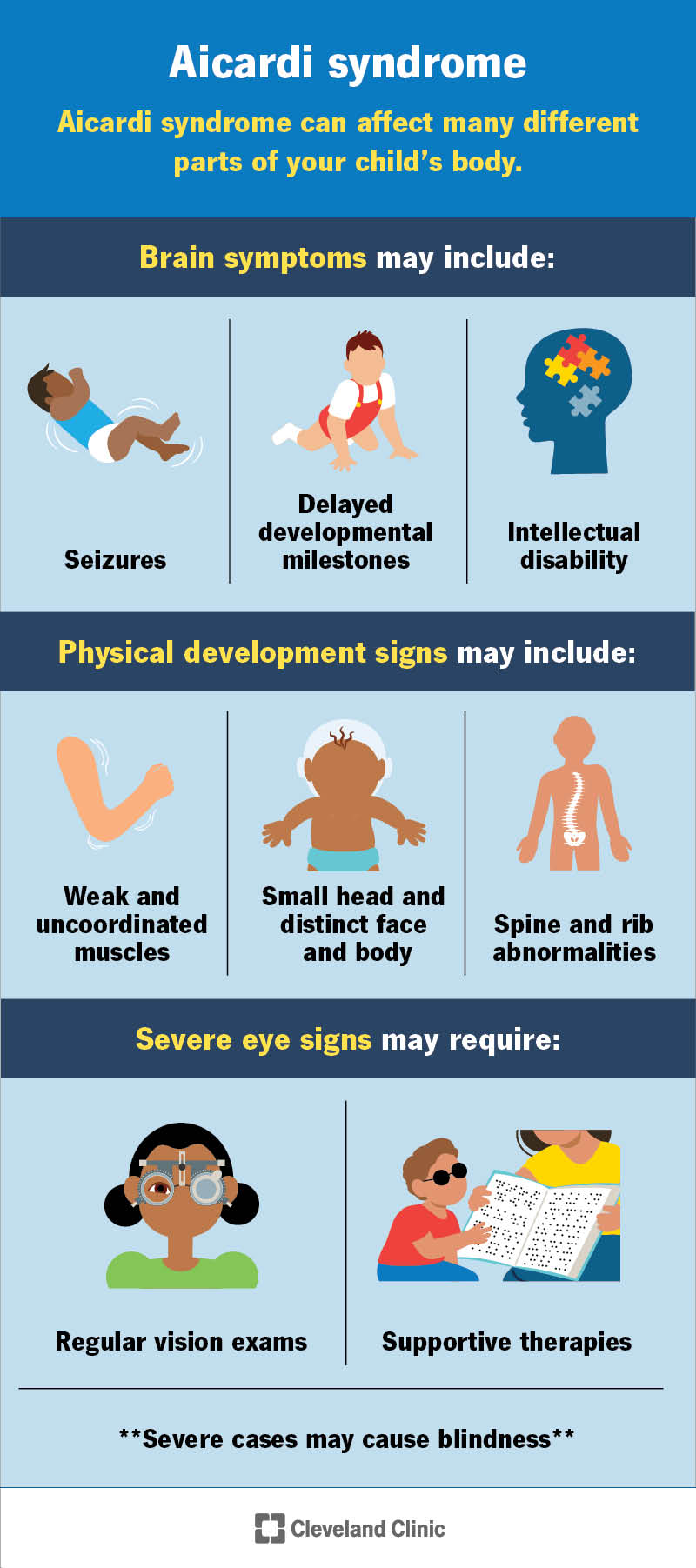
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/arcadi-syndrome)
Aicardi syndrome can affect many different parts of your child’s body, including their:
Signs and symptoms of this condition that affect your child’s brain may include:
Advertisement
One early sign of Aicardi syndrome can be seizures that start when your child is a few months old. These may appear as infantile spasms. You may notice your child’s entire body makes sudden movements or jerks all at once. Seizures may occur several times a day and could get worse over time.
In addition, you may notice that your child misses developmental milestones for their age. This could include delays in walking and saying their first words. Intellectual disability is common and can range from mild to severe.
Aicardi syndrome signs that affect your child’s eyes could include:
Mild cases may cause vision problems that require glasses and regular eye exams. Severe eye abnormalities usually cause blindness.
Aicardi syndrome can affect how certain parts of your child’s body develop. This can lead to the following physical characteristics:
Infants may have trouble sitting up on their own, grasping objects or walking. Your child may have one or multiple characteristics from this list, but likely not all of them.
Gastrointestinal symptoms may also happen with this condition, like:
Even with differences in the way certain parts of their body developed, your child may be able to do some things on their own, like:
It may take your child longer than others to accomplish these skills. Some severe cases may prevent your child from mastering these skills. But each child’s case is different.
A gene variant on the X chromosome causes Aicardi syndrome. Research is ongoing to identify which gene it is.
The condition doesn’t run in families and happens randomly or sporadically. This means a new gene change causes it. You don’t inherit it from your biological parents.
Advertisement
Almost all cases of Aicardi syndrome affect females. This is because a gene variant targets one X chromosome.
Females have two X chromosomes. Males have an X and a Y chromosome. These chromosomes identify whether you’ll have male or female physical sex characteristics.
The condition is fatal in males, as they only have one X chromosome. Females have two X chromosomes and still have one unaffected X chromosome.
Aicardi syndrome can lead to early death. The main causes are:
Your child may be more at risk of life-threatening outcomes from respiratory infections like pneumonia. This is usually due to muscle weakness in their lungs and diaphragm. It can make managing these infections difficult.
A healthcare provider may detect signs of Aicardi syndrome before birth during a prenatal ultrasound. They’ll confirm a diagnosis after your child is born by looking for signs or symptoms that affect your child’s brain and eyes.
Tests can confirm a diagnosis and may include:
Advertisement
Treatment for Aicardi syndrome varies based on how symptoms affect your child.
Antiseizure medications can help regulate seizures. Sometimes, seizures are difficult to treat. There isn’t one medication that works well for everyone. Your child’s provider may offer several different types of antiseizure medications to find one that works best.
Implantable devices, such as a vagus nerve stimulator, help regulate brain activity. This may be an option if medications aren’t successful.
Other types of treatment may include:
Your child will need support throughout their life, especially if they have intellectual disabilities. Support is also available to families and caregivers to help you care for your child and have access to resources if necessary.
If your child didn’t receive a diagnosis during infancy, and they’re missing developmental milestones for their age, like speaking their first words or sitting upright on their own, contact their healthcare provider.
Contact emergency services if your child has a seizure for the first time.
Advertisement
You may have a lot of questions after learning about your child’s diagnosis. You may want to ask:
It’s difficult to know how Aicardi syndrome will affect your child, as the condition is rare and symptoms can vary widely from one person to the next. Your child’s healthcare provider will let you know about your child’s outlook specifically.
Your child will need support throughout their life, as they may not be able to do many things on their own safely or live independently. They’ll need ongoing medical care, therapies and supportive services. Your child’s care team will help you along the way so you know what to expect and how to better support your child.
Your child’s future well-being depends on their symptoms and how severe they are. Severe symptoms may cause your child to have a short life expectancy. Many people with mild symptoms survive into adulthood.
This is different for each person, so talk to your child’s healthcare provider for the most accurate information.
It may be one of the most difficult things for a parent or caregiver to hear — that your child has a rare condition like Aicardi syndrome. You likely have a lot of questions about what this means and what to expect. While healthcare providers can’t predict the future, they can offer care and support to make sure your child has everything they need to stay as healthy as possible.
Care for Aicardi syndrome is lifelong. While this may be a very stressful and emotional journey, know that your child’s providers will be there with you every step of the way. Don’t hesitate to reach out if you need help or have any questions.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your child has a neurological condition, you want them to have the best care. At Cleveland Clinic Children’s, we offer compassionate, personalized treatment.
