Becker muscular dystrophy (BMD) is a rare, inherited condition that causes muscle weakness that gets worse over time. It mainly affects males. There's currently no cure for the condition, so treatment involves managing symptoms and optimizing quality of life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Becker muscular dystrophy (BMD) is a rare, inherited condition that results in progressive muscle degeneration and muscle weakness. It almost exclusively affects males due to its X-linked inheritance (passed on through the mother, who is a carrier).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The muscle weakness usually begins in your legs and pelvis and travels up your body over time.
After myotonic dystrophy and facioscapulohumeral dystrophy, BMD is probably the third most common type of muscular dystrophy found in adults.
Both Becker muscular dystrophy (BMD) and Duchenne muscular dystrophy (DMD) are caused by changes (mutations) in the gene that gives instructions for a protein called dystrophin, which is important for muscle function.
In DMD, dystrophin is completely absent in muscle tissue, while in BMD, there’s some — but not enough — dystrophin present.
Becker muscular dystrophy is less common and less severe than Duchenne muscular dystrophy. The symptoms of the two conditions are similar, but Becker muscular dystrophy gets worse much more slowly.
Becker muscular dystrophy (BMD) mainly affects males, but females who are carriers for BMD can sometimes have symptoms, which are usually mild.
Symptoms most often appear between the ages of 5 and 15 years but may begin later.
Becker muscular dystrophy is rare. It occurs in about 3 to 6 out of every 100,000 births and mainly affects boys.
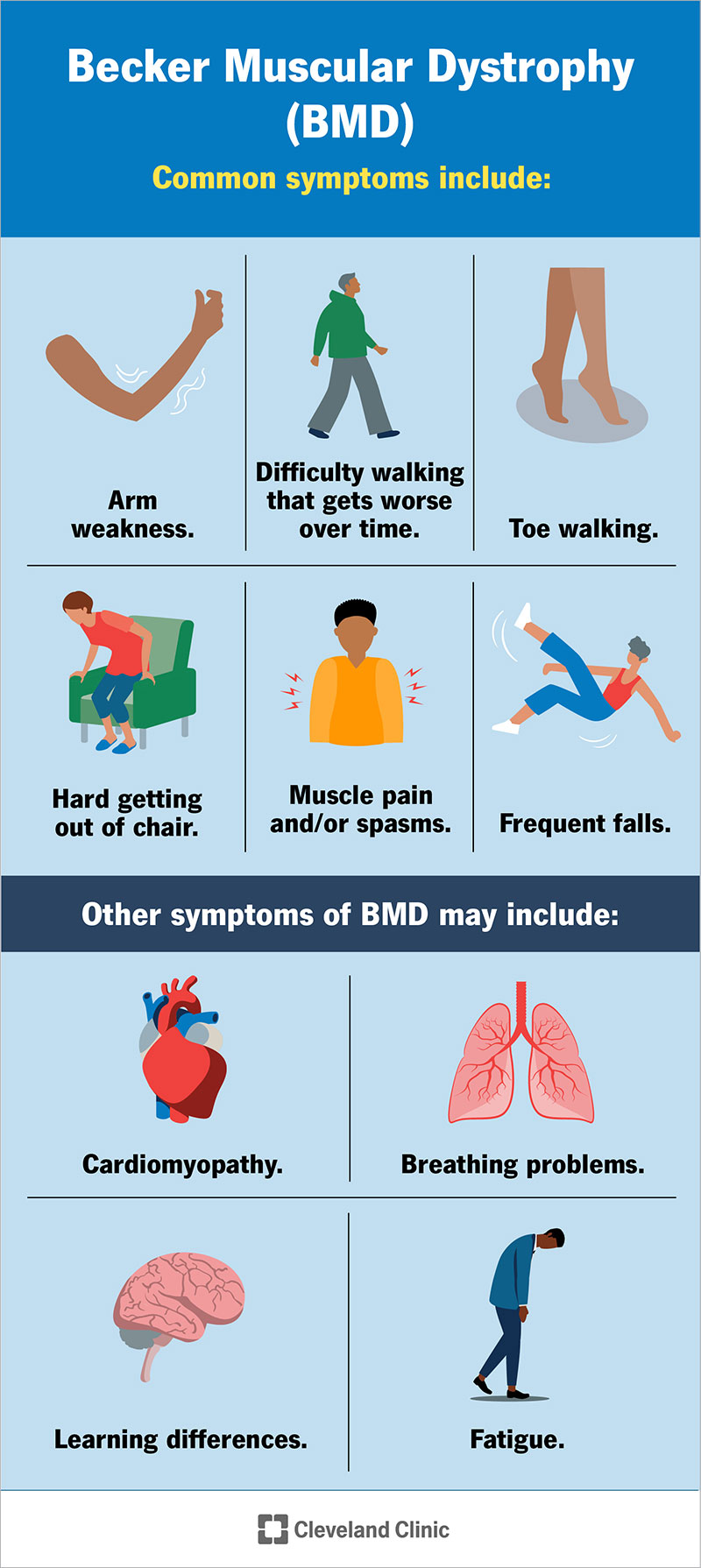
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23541-becker-muscular-dystrophy-bmd)
Symptoms of Becker muscular dystrophy (BMD) most often start between the ages of 5 and 15 years but may begin later.
Advertisement
BMD causes muscle weakness that gets worse over time, so common symptoms include:
Other symptoms of BMD may include:
Females who are carriers of BMD may only have cardiomyopathy or mild muscle weakness. Approximately 22% of carriers have symptoms, but they vary greatly.
Becker muscular dystrophy (BMD) is in inherited condition. It’s caused by a change (mutation) in the gene that gives instructions for a protein called dystrophin. Your body needs dystrophin to stabilize muscle cells.
A change in the dystrophin gene results in nonfunctional or less production of dystrophin, which causes muscle weakness and damage over time.
Becker muscular dystrophy (BMD) has X-linked recessive inheritance.
X-linked means the gene responsible for BMD is located on the X chromosome, one of two sex chromosomes. Genes, like chromosomes, usually come in pairs. Recessive means that when there are two copies of the responsible gene, both copies must have a disease-causing change (pathogenic variant or mutation) for a person to have the condition.
Because males have one X chromosome and thus only one copy of the gene, a pathogenic variant in their one copy is enough to cause BMD.
Because females have two X chromosomes, a pathogenic variant for an X-linked recessive disease generally needs to occur in both copies of the gene to cause the condition. Females who have a variant in one copy of the gene are called carriers. In rare cases, females who are carriers may experience mild to moderate symptoms, but most have no symptoms.
A women who carries one X-linked gene variant has a 50% chance of having a son with BMD and a 50% chance of having a daughter who is a carrier. A man with BMD can’t pass it on to their sons, but all of their daughters will be carriers.
If you or your child are experiencing symptoms of Becker muscular dystrophy, your healthcare provider will likely perform a physical exam, neurological exam and muscle exam. They’ll ask detailed questions about your symptoms and medical history.
During the exams, they may find:
Advertisement
If your provider suspects that you or your child may have Becker muscular dystrophy, they’ll likely order the following tests:
If you or your child has BMD, your provider may also recommend an electrocardiogram (EKG) and echocardiogram to check for any heart muscle issues that BMD can cause.
There’s currently no cure for Becker muscular dystrophy (BMD), so the main goal of treatment is to manage symptoms and optimize quality of life.
The two main forms of treatment for BMD include:
Advertisement
Other supportive therapies for BMD include:
There are many new drugs currently undergoing clinical testing that show promise in treating BMD.
The prognosis (outlook) of Becker muscular dystrophy (BMD) varies. BMD leads to slowly worsening disability, but the severity of disability varies. Some people may need a wheelchair, while others may only need to use walking aids such as canes or braces.
If a person with BMD has heart or breathing issues, their lifespan may be shortened.
Possible complications of BMD include:
The average life expectancy of a person with Becker muscular dystrophy is somewhat shortened and is about 40 to 50 years. Dilated cardiomyopathy (weakening of your heart muscles) is the most common cause of death.
Advertisement
Since Becker muscular dystrophy (BMD) is an inherited condition, there’s nothing you can do to prevent it.
If you have BMD, or if you’re concerned about the risk of passing on BMD or other genetic conditions before trying to have a biological child, talk to your healthcare provider about genetic counseling.
If you have Becker muscular dystrophy (BMD), it’s essential to ensure you’re getting quality medical care to prevent or treat complications of BMD, such as heart and breathing issues. You may also want to consider joining a support group to meet others who can relate to your experiences.
If you’re taking care of someone with BMD, it’s important to advocate for them to ensure they get the best medical care and access to mobility devices and therapy that can help them be more independent.
If you (or your child) have been diagnosed with Becker’s muscular dystrophy, you’ll need to see your team of healthcare providers regularly to receive treatment and monitor symptoms.
Understanding your (or your child’s) diagnosis of Becker muscular dystrophy diagnosis can be overwhelming. Your healthcare team will offer a robust management plan that’s unique to your symptoms. It’s important to make sure you receive the support needed and are attentive to your health.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.