Flat and inverted nipples lay flat or point inward instead of sticking out. They’re usually harmless, but they can make breastfeeding more difficult. Most people with flat or inverted nipples are born with them. But if you have nipples that invert suddenly, it could indicate an underlying health condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
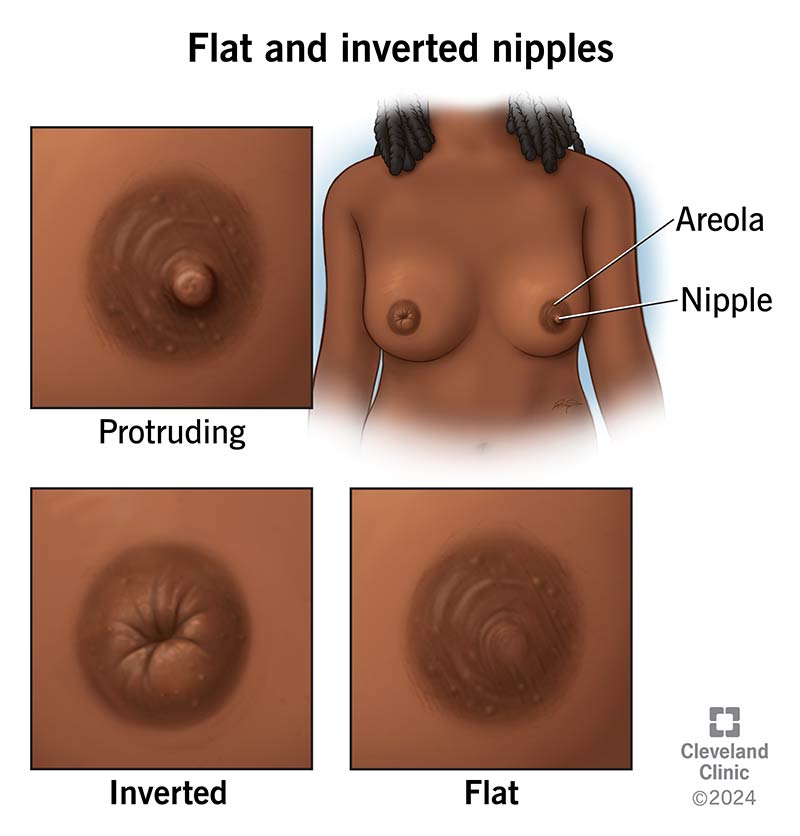
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/flat-inverted-nipples.jpg)
Flat nipples lay even with your surrounding breast tissue. Inverted nipples point inward toward your breast instead of sticking out. Inverted and flat nipples are usually just harmless variations of healthy breast anatomy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Though flat and inverted nipples are typically harmless, sudden changes in the color or shape of your nipples could indicate an underlying health condition. If your nipples invert or change suddenly, let a healthcare provider know.
Your nipples might be:
About 10% to 20% of the general population has flat or inverted nipples.
There can be many reasons why someone has flat or inverted nipples. Possible causes include:
Advertisement
Flat or inverted nipples usually don’t indicate cancer. But if your nipple’s appearance changes suddenly, talk to a healthcare provider. It could be a sign of underlying disease.
People with breast cancer may notice that their nipple suddenly becomes flat or inverted. Additional breast cancer symptoms may include:
A healthcare provider can tell you if your flat or inverted nipples are a cause for concern. They’ll do a physical examination to see if they feel any lumps or bumps. They may also recommend tests to rule out other conditions. These tests may include:
Flat or inverted nipples don’t always need treatment. But if a condition causes flat or inverted nipples — or you just want to enhance the appearance of your nipples — your provider will help you choose a treatment based on your specific needs.
If an infection causes flat or inverted nipples, a provider can prescribe antibiotics. They can also drain or surgically remove any abscesses.
Flat or inverted nipples might make it difficult for your baby to latch during breastfeeding. While it can be challenging at first, you can still breastfeed with flat or inverted nipples. There are things you can try to coax your nipples outward, making it easier for your baby to attach. These include:
If these methods fail, consider talking with a lactation consultant. They may recommend nipple shields. Nipple shields are thin silicone covers that can help your baby latch. Be sure to discuss the pros and cons of nipple shields with your healthcare provider.
Advertisement
When breast cancer causes flat or inverted nipples, you’ll meet with an oncologist to discuss your treatment options, which might include:
Nipples come in all varieties, including flat and inverted. But if you feel self-conscious about your nipples, your provider can recommend plastic surgery procedures to make them more protruded.
Inverted nipples don’t usually go away on their own. If you’re concerned about their appearance, speak with your provider about surgical options. Or, ask your provider about options for training your nipple outwards, like the Hoffmann technique. Your provider can discuss short-term and long-term solutions based on what’s causing your nipples to invert and what grade of inversion they are.
Most of the time, people are born with flat or inverted nipples. In these cases, there’s nothing you can do to prevent them.
But you can reduce your risk of infection by not smoking. Most people who have periductal mastitis (a chronic infection of breast tissue) use tobacco products. The condition causes many symptoms, including nipple inversion.
Yes, it’s totally possible to breastfeed with flat or inverted nipples. Your healthcare provider can recommend ways to turn your nipples outward so your baby can latch.
Advertisement
It’s normal to feel frustrated when faced with these challenges. But your provider is here to help.
Your provider needs to know if you’ve noticed sudden changes in your breast, like inverted nipples. This change may signal an underlying issue that requires treatment.
Some people get nipple piercings to help their inverted nipples protrude more. The idea is that the jewelry will keep your nipple erect.
It’s important to know that inverted nipple piercing doesn’t work for everyone. It can also make you more prone to infections. (Not to mention, it can be painful.) You also shouldn’t get your nipples pierced if you plan on breastfeeding. Before you get your nipples pierced, talk to your healthcare provider about risks and benefits.
Having flat or inverted nipples doesn’t mean there’s something wrong with you. In fact, healthy nipples come in many shapes and sizes. But if you want to fix inverted or flat nipples — whether it’s to breastfeed or simply to boost your confidence — your healthcare provider can find a treatment that works for you and your specific needs.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
