A brachial plexus injury involves sudden damage to the network of nerves that branch off from your spinal cord in your neck and extend down into your shoulder, arm and hand. Symptoms include muscle weakness, pain and diminished sensation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
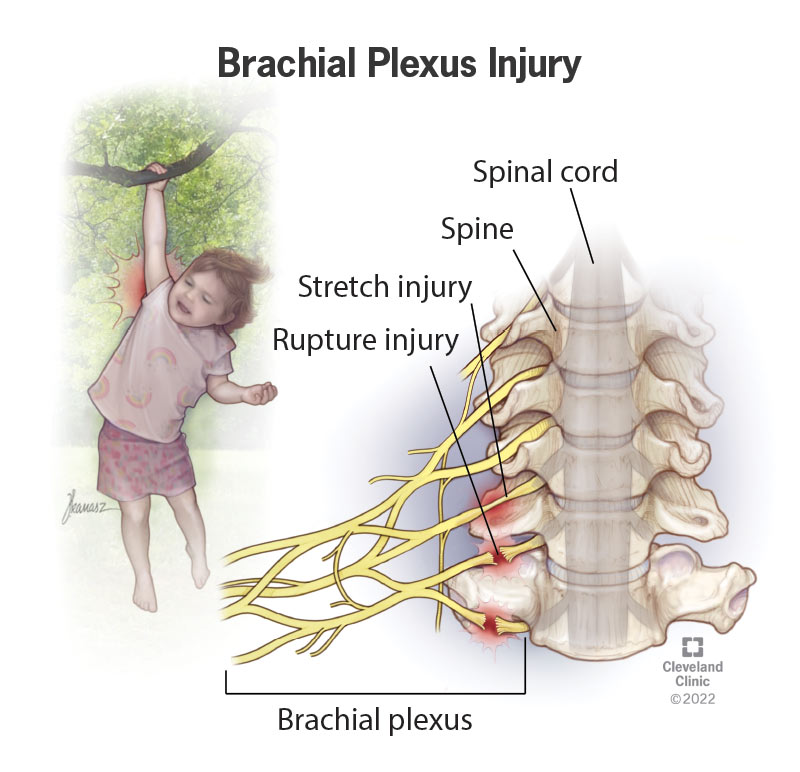
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22822-brachial-plexus-injury)
The brachial plexus is a network of intertwined nerves that control movement and sensation in your arm and hand. A brachial plexus injury involves sudden damage to these nerves, which may cause pain, weakness, loss of feeling, or loss of movement in your shoulder, arm and/or hand.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The brachial plexus begins at your neck and crosses your upper chest to your armpit. Injury to this network of nerves often happens when your arm is forcibly pulled or stretched or your head and neck are forcibly pulled away from your shoulder.
Mild brachial plexus injuries may heal without treatment, but more severe injuries may require surgery to regain function in your arm or hand.
Babies can experience brachial plexus injuries while in the uterus or during delivery. This injury is called neonatal brachial plexus palsy (NBPP).
The brachial plexus consists of five nerves that branch off from your spinal cord at your neck and conduct signals from your spinal cord to your shoulder, arm and hand. You have a brachial plexus on each side of your body.
In the medical world, a plexus is a bundle of intersecting nerves, blood vessels or lymphatic vessels in the human body. “Brachial” means “relating to the arm or to a structure resembling the arm.” (The brachial artery, for example, is the main vessel supplying blood to the muscles in your upper arm and elbow joint.) Thus, the brachial plexus is a bundle of nerves that run from your spinal cord down into your arm.
The plexus connects these five nerves with the nerves that provide sensation to your skin and allow movement in the muscles of your arm and hand.
Advertisement
Each of the five nerves in the brachial plexus has a specific function, such as stimulating muscles or carrying sensory information, like temperature and touch, from your hand to your brain.
Because each nerve has a different function, the location of the nerve injury and the type of nerve injury within the plexus determines the symptoms you experience and the type of treatment you may need.
There are five nerves in your brachial plexus, each with a different function. These nerves work together to complete movements and sensations in your arms and hands:
Brachial plexus injuries vary greatly in severity, depending on the type of injury and the amount of force involved. You can injure several different nerves of your brachial plexus in varying severity from the same event.
The main types of brachial plexus injuries include:
While cervical radiculopathy and a brachial plexus injury have similar symptoms, they are different conditions.
Cervical radiculopathy (also known as “pinched nerve”) is a condition that results in neurological dysfunction caused by compression and inflammation of any of the nerve roots of your cervical spine (neck). Neurological dysfunction can include radiating pain, muscle weakness and/or numbness.
Advertisement
While cervical radiculopathy results from compression and inflammation, a brachial plexus injury more commonly happens due to tearing or overstretching the nerves in the plexus.
Brachial plexus injuries often involve multiple nerve roots and there’s usually an absence of neck symptoms, such as neck spasms and pain, unlike with cervical radiculopathy.
Anyone at any age can experience a brachial plexus injury, including babies during delivery.
These injuries are most common in males between the ages of 15 and 25.
Researchers don’t know exactly how many brachial plexus injuries happen to children and adults each year, but the number seems to be increasing. More participation in high-energy sports and higher rates of survival from high-speed motor vehicle accidents may be reasons why the number of these injuries is growing.
Approximately 70% of traumatic brachial plexus injuries result from traffic accidents, of which 70% involve motorcycles or bicycles.
Neonatal (infant) brachial plexus injuries are a common type of birth injury. There are 2 to 3 cases for every 1,000 births.
Symptoms of a brachial plexus injury vary depending on the type of injury and which nerve(s) are affected. You may also experience other symptoms at the same time if you have other injuries.
Advertisement
The most common symptoms of a brachial plexus injury in children and adults include:
Symptoms of a brachial plexus injury in newborns include:
Brachial plexus injuries can occur as a result of:
Damage to the upper part of your brachial plexus often occurs when your shoulder is forced down while your neck is forced up and away from your shoulder.
Damage to the lower part of your brachial nerves is more likely to happen when your arm is suddenly forced above your head.
Examples of trauma that can result in damage to your brachial plexus include:
Advertisement
Tumors can grow in or along your brachial plexus or put pressure on your brachial plexus.
Breast cancer and lung cancer are the most common cancers that involve your brachial plexus.
Lymphoma, melanoma and squamous cell carcinomas arising in your head and neck, and malignant mesotheliomas are some of the tumors that can metastasize (spread) to your axillary (armpit) lymph nodes and affect your brachial plexus.
When your body encounters an offending agent (like viruses, bacteria or toxic chemicals) or suffers an injury, it activates your immune system.
Your immune system sends out its first responders: inflammatory cells and cytokines (substances that stimulate more inflammatory cells).
These cells begin an inflammatory response to trap bacteria and other offending agents or start healing injured tissue. While this inflammatory response is necessary in a lot of cases, sometimes, your immune system can send out its first responders for no known reason and attack healthy tissue. Or the inflammatory response to an offending agent can be excessive and damage tissues in your body in the process.
A rare syndrome called Parsonage-Turner Syndrome (brachial neuritis) causes inflammation of the brachial plexus without any obvious shoulder injury. It can begin with severe shoulder or arm pain followed by weakness and numbness.
This syndrome is often misdiagnosed as cervical radiculopathy.
Infants can experience brachial plexus injuries due to compression inside their birth mother’s uterus or during a difficult delivery. This injury is called neonatal brachial plexus palsy (NBPP). Injury may be caused by the following situations:
If your healthcare provider suspects you have a brachial plexus injury, they’ll perform a comprehensive examination to diagnose the injury and determine whether you have any other injuries, which is common in forceful events that result in brachial plexus injuries.
Your provider will examine all the nerve groups involved with the brachial plexus to identify the specific location of the nerve injury and its severity. The pattern by which nerves from the brachial plexus control different muscles of your arm and hand will help your provider identify potential sites of nerve injury.
If your newborn shows signs of a brachial plexus injury, their provider will perform a physical exam to see if your baby can move their upper or lower arm or hand. Their affected arm may flop when their provider rolls them from side to side. The Moro reflex (startle response) is also absent on the side of the injury.
Your healthcare provider may perform several tests to help diagnose a brachial plexus injury and to check for other possible injuries. These tests include:
If your newborn infant shows signs of a brachial plexus injury, their provider may request an X-ray of their collarbone to see if it’s fractured.
Neonatal brachial plexus injuries can mimic a condition called pseudoparalysis. This happens when an infant has a fracture and isn’t moving their arm because of pain, not because they have nerve damage.
As brachial plexus injuries are typically caused by traumatic, forceful events, many people have additional injuries. These may include:
Because of this, your healthcare team may need to treat these more life-threatening injuries before they start treating the brachial plexus injury.
A brachial plexus injury is best managed by a team of medical professionals that may include a:
There are two main types of treatment for brachial plexus injuries: nonsurgical and surgical.
Many brachial plexus injuries will heal without surgery over a period of weeks to months, especially if they’re mild. Nerve injuries that heal on their own tend to have better outcomes in terms of muscle and nerve function.
If your healthcare provider thinks the injury has a good potential for recovery without surgery, they may wait to see how your injury heals before considering surgery.
Your provider may recommend physical therapy as your injury heals to prevent joint and muscle stiffness. You’ll also likely need to rest your arm and shoulder and avoid strenuous activities.
Healthcare providers typically recommend surgical treatment for brachial plexus injuries when the nerves don’t heal on their own or don’t recover enough to restore necessary function to your arm and hand.
It’s important to know that depending on the severity of the injury, surgery may not be able to return your arm or hand to its abilities before the injury.
Neurosurgeons use several different techniques to treat nerve injuries, depending on the type and severity of the injury and the amount of time that has passed since the injury.
Types of surgical procedures include:
If your newborn has a mild brachial plexus injury, their provider will likely recommend gently massaging their arm and range-of-motion exercises for treatment.
If the damage is severe or it doesn’t improve within the first few weeks, your baby may need to see a pediatric neurosurgeon. They may consider surgery if your baby’s strength doesn’t improve by 3 to 9 months of age.
All surgeries have certain risks of possible complications, including:
In addition, if you have pre-existing medical conditions, you may have additional risk factors that could make it more likely to experience the following complications:
Nerves heal very slowly. Because of this, recovery from a brachial plexus injury takes time. You may not experience results or improvement for several months.
It’s important to keep a positive mindset and to stay committed to your treatment plan.
You’ll likely work with an occupational therapist to learn how to use your unaffected arm to perform daily activities like eating and personal hygiene.
You’ll also likely need physical therapy for your shoulder, elbow, wrist and fingers to prevent stiffness and muscle atrophy.
It’s important to develop healthy coping skills to make adjustments in your life — both in terms of employment and daily activities — in case your arm and/or hand function doesn’t return to how it was before your injury.
The prognosis (outlook) for brachial plexus injuries depends on several factors, including:
For avulsion and rupture injuries, there’s generally no potential for muscle and function recovery unless you undergo surgical reconnection of your nerves in a timely manner.
Most people who have stretch injuries (neuropraxia) recover without surgery with a 90% to 100% return of nerve function.
Most babies who experience a brachial plexus injury at birth will fully recover within three to four months. Babies who don’t recover during this time have a poor outlook. In these cases, they may have a nerve avulsion.
Risk factors for experiencing a brachial plexus injury include:
Always practice safety when playing sports and driving to try to prevent these injuries.
The following factors increase the risk of neonatal brachial plexus palsy (NBPP):
If you’ve experienced a brachial plexus injury, you’ll need to see your healthcare team regularly throughout your recovery to monitor the healing and function of your nerves.
You’ll also need to see your physical therapist regularly if you have a rehabilitation plan. It’s very important to commit to these therapies so you can have the best possible outcome.
Nerves heal slowly. The recovery period after a brachial plexus injury, especially after surgery, is often long and requires a strong commitment to a rehabilitation program to restore physical abilities. While it can be daunting to have such a long recovery, it’s important to maintain a positive outlook. Reach out to your friends and family for support. Your healthcare providers are also available to offer support and comprehensive treatment plans.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
