A dislocated kneecap (patella dislocation) occurs when your kneecap pops sideways out of its vertical groove at your knee joint. It’s usually caused by force, from a collision, a fall or a bad step. A dislocated patella is painful and will prevent you from walking, but it’s easy to correct and sometimes corrects itself.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
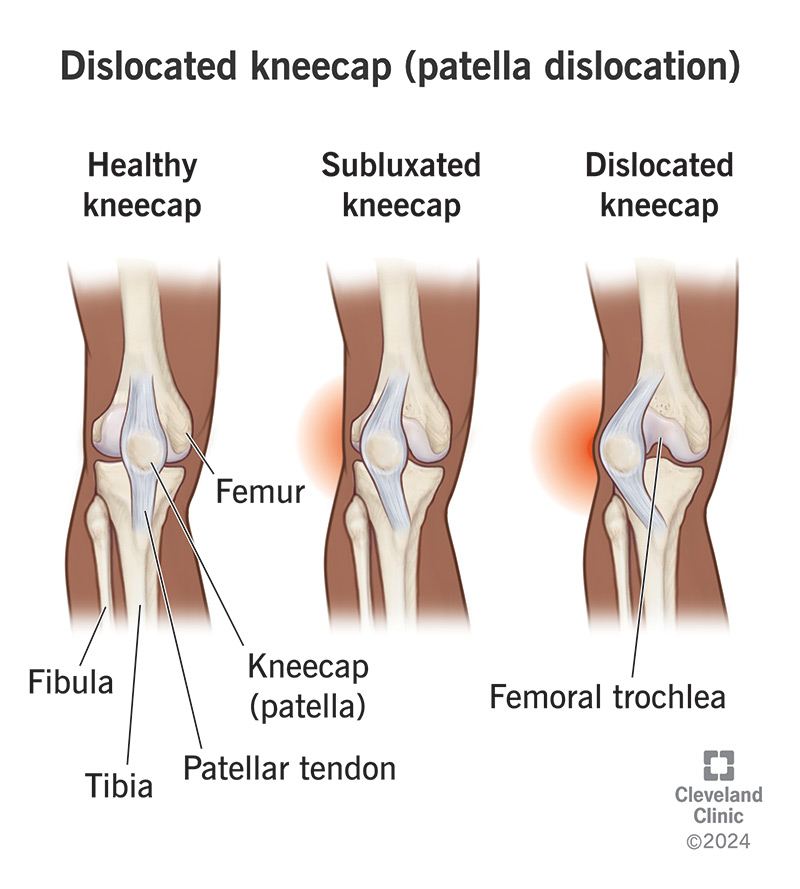
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/dislocated-kneecap)
A patella dislocation occurs when your kneecap (patella) slides out of the groove at your knee joint. Your knee joint is a meeting of three bones: your thighbone (femur), shinbone (tibia) and patella in the middle. Normally, when you bend and straighten your leg, your kneecap slides up and down inside a vertical groove (the trochlear groove) between the bottom end of your femur and the upper end of your tibia. A network of tendons and ligaments secure your kneecap within the groove, flexing as it moves.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When your patella dislocates, it’s forced outside of the trochlear groove and can no longer move up and down. This locks your knee and pulls the ligaments out of place, often tearing them. Most frequently, your kneecap pops out laterally (to the side of the groove). Like any dislocation, a dislocated kneecap is painful and debilitating until you correct it. But a dislocated patella will sometimes correct itself.
A patella dislocation is different than a knee dislocation, a much more serious injury that involves your femur and tibia. It’s also different than a patella subluxation, in which your kneecap only partially dislocates.
There are two main types of patella dislocations:
Patellar dislocation symptoms may include:
Advertisement
Long-term complications may include a less stable knee joint and deteriorated cartilage, which can contribute to knee osteoarthritis later in life.
In addition, up to 45% of people who’ve experienced a patella dislocation will dislocate their knee again. This recurrence can happen from weeks to years later.
Force — either from a direct impact or a bad step that uses your own body weight against you — causes acute patellar dislocation. A heavy fall or collision can knock your kneecap out of place. But it doesn’t always take that much. Something as simple as a sudden turn that twists your knee while your lower leg is still firmly planted can cause it. This commonly happens to athletes and dancers, who are prone to quick pivots.
Some people have patellar instability, which means that the tendons and ligaments that hold your kneecap in place are already loose and unstable. An unstable kneecap will dislocate more easily.
People with congenital patellar dislocation (trochlear dysplasia) are born with the condition. It’s often, but not always, related to other developmental abnormalities.
Anyone can dislocate their patellas through injury. But certain people are more at risk, including:
Researchers don’t know what causes congenital patella dislocation, but a higher incidence among biological family members suggests a genetic link. Certain other congenital conditions are also associated with it, including:
A healthcare provider can usually diagnose a dislocated kneecap by physically examining your knee and asking you questions about the injury. In addition, they’ll order imaging tests to check for any related injuries, like torn ligaments, cartilage injuries or fractures. Imaging tests may include:
If your dislocated patella corrected itself, you might not realize that it was dislocated. A dislocation that corrects itself is called “transient.” Afterward, your knee will still be sore and swollen, but it may look like many other more common knee injuries. In this case, imaging tests can show evidence after the fact that there was a dislocation, along with secondary injuries.
Advertisement
Patellar dislocation treatment starts by resting your knee. Don’t try to walk on it or perform any of your usual physical activities. You may also want to use an ice pack and take pain relievers (NSAIDs) to help with the pain and swelling. Your healthcare provider may treat the kneecap dislocation using several different methods:
Possibly. The kneecap has been known to pop back into place on its own when the leg is carefully extended. If it’s too painful to extend the leg, your healthcare provider can give you medication to make it easier. If you do fix it yourself, see your healthcare provider after. They’ll want to check for fractures and for damage done to the cartilage and ligaments.
Advertisement
If you think you may have dislocated your kneecap, you should see your provider. Look for signs including:
Questions you may want to ask your provider include:
Recovery time for a dislocated kneecap depends on the severity of your injury and method of treatment.
If this is your first patella dislocation and there’s no major damage, your prognosis (outlook) is good. Most people will be able to get back to their normal, daily activities within six to eight weeks. You can usually participate in sports after three to four months.
If you have recurring dislocations or major damage that requires surgery, your recovery time will take longer. It may be more than a year before you’re back to playing sports.
All dislocations stretch your ligaments and deteriorate the cartilage of your joints to some extent. Once you dislocate your patella, it’s more likely to happen again if you reinjure it in a similar way. Accidents are hard to prevent, but sometimes there are contributing factors that you can try to reduce. Depending on what made your patella dislocate in the first place, you may want to take one or several of these preventive measures:
Advertisement
Dislocations are often very painful, but there’s a range. It depends on the extent of the injury. It’ll always be painful to move the dislocated joint or bear weight on it. You won’t be able to use the limb normally until you correct the joint.
If your dislocated patella corrects itself, your pain and mobility may improve. But you should still see your healthcare provider. They’ll check for secondary injuries to your ligaments and guide you through the longer rehabilitation process.
No. Your knee will either be locked and unable to straighten or bend, or it’ll catch and pop when you try to bend it. The joint will be unstable and buckle when you try to bear weight on it. It will also be painful to move it. If you can walk, you may only have a patella subluxation.
If your dislocated patella pops back into place, you may be able to walk afterward. But the knee will still be swollen and painful from the trauma. You shouldn’t try to walk if it’s too painful. Always see your healthcare provider anyway to check for any secondary injuries. They’ll likely recommend crutches and a brace when you begin to walk again.
A dislocated patella can be a scary and painful injury. You may be able to pop your kneecap back into place yourself, but you should still see your healthcare provider for treatment. At a minimum, your provider will recommend that you rest your knee and get physical therapy to strengthen your muscles, tendons and ligaments. More serious injuries may require surgery and extended rehabilitation. With time, you’ll be back on your feet.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Knee pain can keep you from doing the things you love. Cleveland Clinic experts can craft a treatment plan to get you back to the regular pace of your life.
