Stickler syndrome is a genetic condition that affects connective tissues in your face and joints, leading to problems with vision, hearing and movement. This hereditary condition is usually diagnosed in babies and children, and early treatment leads to a positive outcome.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Stickler syndrome is a genetic condition that affects connective tissues that support and give structure to other organs in your body, primarily in the face, ears, eyes and joints. This hereditary condition can cause facial abnormalities like a cleft palate. The condition can lead to problems with vision, hearing and movement.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Stickler syndrome is also known as Stickler dysplasia.
Stickler syndrome can affect anyone. People who have a family member with Stickler syndrome are at a higher risk of having the condition. But in some people, a spontaneous genetic change (mutation) causes the condition and there’s no tie to family history.
Stickler syndrome occurs in roughly 1 to 3 out of 7,500 to 10,000 newborns. The exact rate of occurrence among the general population is unknown because many cases of Stickler syndrome go undiagnosed. In the U.S., Stickler syndrome is one of the most common connective tissue conditions that exists.
Stickler syndrome affects connective tissues in your body, which are responsible for protecting and supporting other tissues and organs. Because a mutation of a gene responsible for making connective tissue didn’t receive instructions on how to form and function, symptoms of the condition affect how you see, hear and move, targeting your eyes, ears and joints. It’s common for people diagnosed with Stickler syndrome to have arthritis at a young age. Treatment addresses symptoms of Stickler syndrome to allow those diagnosed with the condition to live full and active lives.
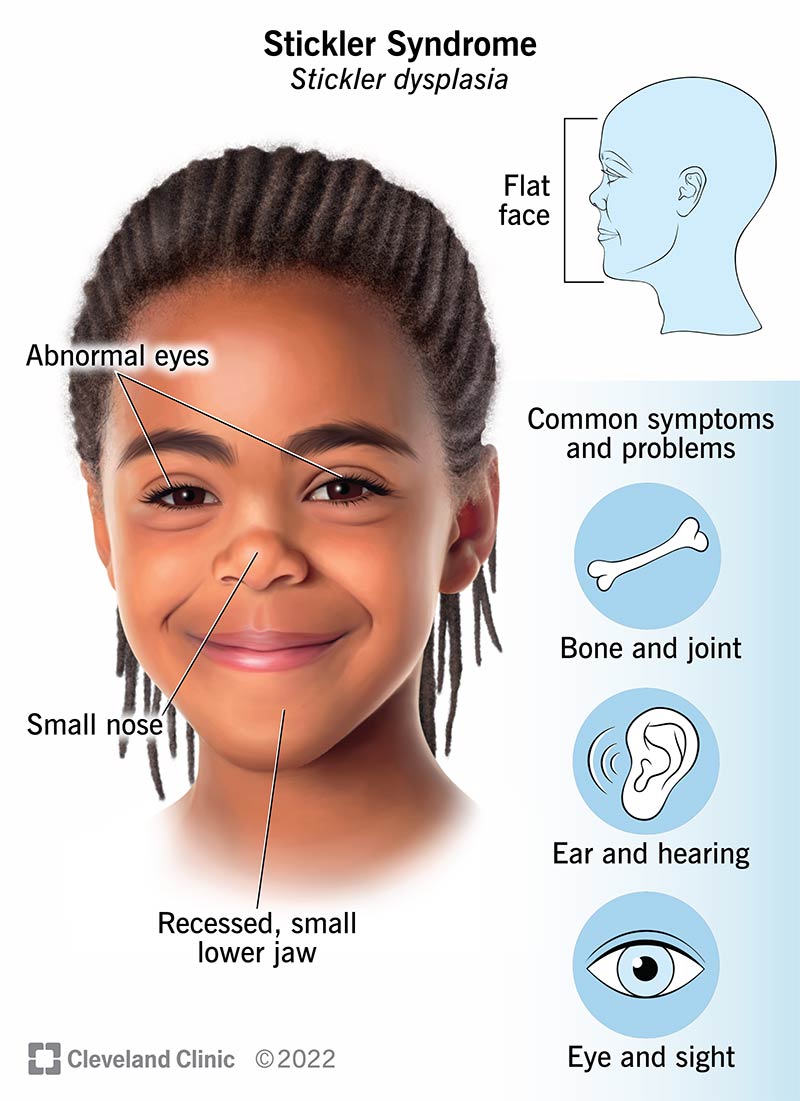
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17987-stickler-syndrome)
Symptoms of Stickler syndrome vary from person to person. It’s rare for people to experience all of the symptoms associated with the condition. Symptoms of Stickler syndrome could include:
Advertisement
Additional symptoms could include:
Many children with the condition have symptoms that affect how the structure of their faces develops. These symptoms include:
There are six types of Stickler syndrome. Symptoms of each type range in severity as the types increase in number. Types I through III are most common – with type I being the most common. Types IV, V and VI are extremely rare. Symptoms for each type include:
A genetic mutation of one of six genes causes Stickler syndrome. The six genes are:
These genes are responsible for forming collagen (proteins that add flexibility and strength to connective tissue). When a genetic mutation occurs, collagen doesn’t develop properly. The mutated genes mainly affect the collagen that makes cartilage in the body and the jelly-like substance inside the eyes.
If a child receives a mutated copy of any one of these genes, they will show symptoms of Stickler syndrome.
Inheritance of Stickler syndrome is almost always autosomal dominant (types I-III) but is occasionally autosomal recessive (types IV-VI). If a child inherits the gene in an autosomal dominant pattern, only one parent needs to have the genetic mutation to have a 50% chance of passing it on to their child during fertilization. With recessive inheritance, both parents are healthy carriers who only have one mutation (no symptoms) but would have a 25% chance of having a child who inherits a mutation from each of them.
Some genetic mutations occur randomly, without being present in a person’s family history (de novo). You can’t predict the occurrence of de novo mutations.
Advertisement
Healthcare providers classify Stickler syndrome into different types during diagnosis. Each type has varying symptoms. Your healthcare provider will identify the type of Stickler syndrome using your family medical history and diagnostic tests. Diagnosis may involve:
Healthcare providers will diagnose Stickler syndrome early in babies, typically after they’re born, to confirm the diagnosis. Prenatally, genetic testing can identify any gene abnormalities or genetic mutations associated with the condition. A confirmation of the diagnosis occurs after the baby is born, once your healthcare provider is able to perform a complete physical exam along with any other imaging tests to check for symptoms.
Advertisement
Treatment for Stickler syndrome varies depending on a person’s symptoms. There’s no cure for the condition, so treatment aims to alleviate symptoms. Early diagnosis and treatment of symptoms lead to the best outcome, especially if there’s a need to repair a detached retina or joint abnormalities.
Your healthcare provider will offer different types of treatment to manage symptoms associated with the condition. Common treatments include:
Stickler syndrome has no cure. The condition does not affect life expectancy. With ongoing treatment and support, many people with Stickler syndrome live active and fulfilling lives. Prompt diagnosis is important during infancy or early childhood so your healthcare provider can alleviate symptoms and help prevent complications.
Advertisement
Symptoms can arise after treatment. For example, if someone receives retinal reattachment surgery, their retinas can detach again, even if the first surgery was successful. It’s important to schedule regular checkups with your healthcare provider to address any concerns about the condition and your symptoms as they arise.
Stickler syndrome affects people’s regular activities differently depending on the symptoms. Your healthcare provider can help you understand healthy activity levels depending on the symptoms the condition causes.
People diagnosed with Stickler syndrome should avoid playing contact sports like football because there’s a high risk of retinal detachment that would require surgery to preserve their vision.
You can’t prevent Stickler syndrome since it’s the result of an inherited genetic mutation. People with a family history of the condition who want to have children should seek genetic counseling and genetic testing to learn about the risk of having a child with the condition.
Contact your healthcare provider if you or your child shows signs or symptoms of Stickler syndrome that are preventing you from going about your normal daily tasks. Symptoms include:
If you or your child are having trouble breathing, visit the emergency room or call 911 immediately.
If you or your child has Stickler syndrome, you may want to ask your doctor:
Stickler syndrome can affect each person differently and the symptoms can range in severity, but the diagnosis does not affect overall life expectancy and the majority of cases have a positive prognosis. Since the condition is hereditary, if you plan on becoming pregnant, talk with your healthcare provider about genetic testing to understand your risk of having a child with a genetic condition.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Do certain health conditions seem to run in your family? Are you ready to find out if you’re at risk? Cleveland Clinic’s genetics team can help.
