Inflammatory breast cancer (IBC) is a rare, aggressive cancer. It affects the skin on your breast. It happens when cancerous cells block lymphatic vessels in your breast and cause inflammation. Inflammation may change your breast skin color and appearance. Treatment may be a combination of chemotherapy, targeted therapy and surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
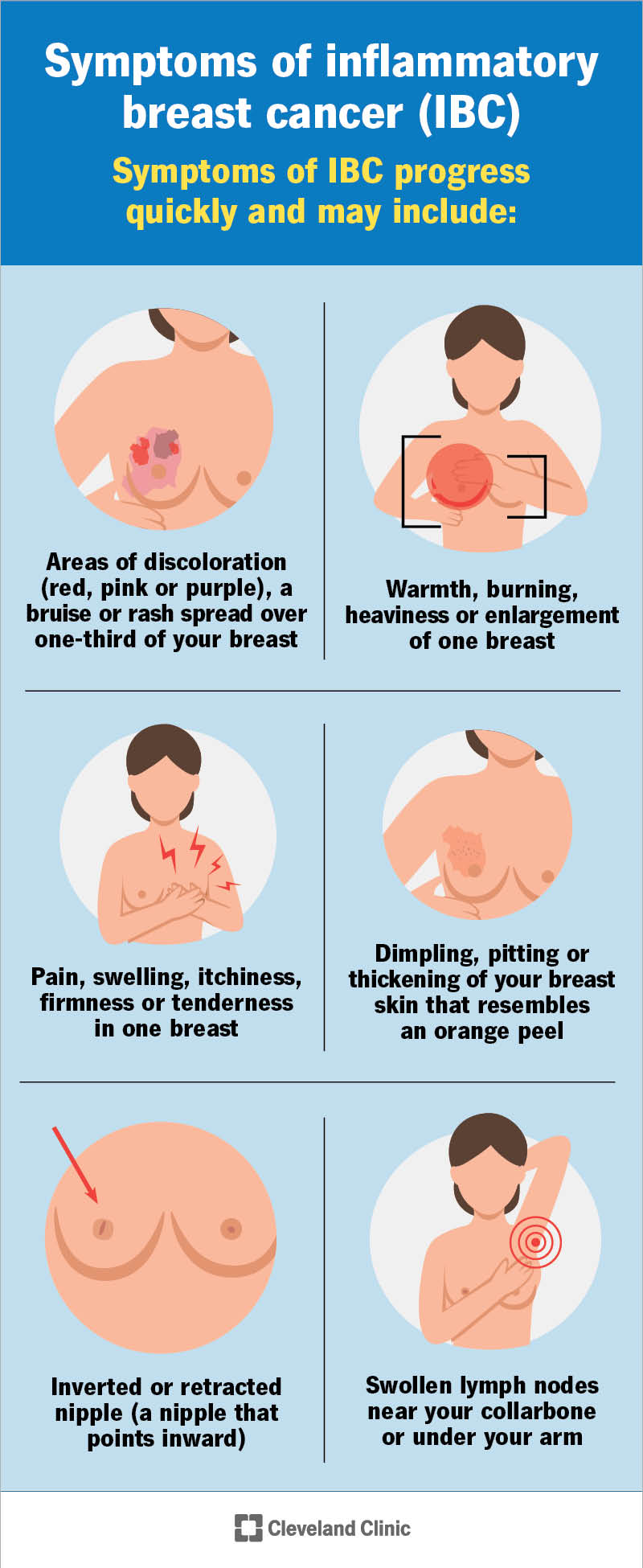
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/17925-Inflammatory-breast-cancer)
Inflammatory breast cancer (IBC) is a rare, fast-growing type of breast cancer. It happens when cancerous cells block lymphatic vessels in one of your breasts. The blocked vessels cause inflammation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Inflammation makes your breast look swollen or discolored. The disease may thicken your breast skin or make it look pitted like an orange peel.
IBC can spread rapidly. It moves from lymphatic vessels in your breast to nearby breast tissue and lymph nodes or other areas of your body. You’ll need treatment right away if tests show you have this type of breast cancer.
IBC doesn’t cause breast lumps like other types of breast cancer or benign breast disease. But it can cause these noticeable symptoms, which develop rapidly and don’t go away:
Experts don’t know the exact cause of inflammatory breast cancer. They do know that having obesity may increase your risk. Having obesity means your body mass index (BMI) is 30 or higher. Researchers are studying other issues that may increase your risk.
Advertisement
Inflammatory breast cancer can spread (metastasize) very quickly. It may spread to other parts of your body, like your brain, lungs or liver.
A healthcare provider will do a physical examination. They’ll ask about your symptoms, including when you first noticed changes in your breast.
They may do the following tests:
Your provider may refer you to a surgical oncologist for a breast biopsy. They’ll remove a small piece of tissue from your breast. A medical pathologist will test the sample for cancerous cells. If they find cancerous cells, your pathologist will check for receptors. These are special proteins that help cancerous cells grow.
Biopsy results can help your cancer care team determine the cancer stage, like whether it has spread to other areas of your body, including your bones, liver or lungs. Often, the cancer is spreading by the time most women receive their diagnosis.
You may have other tests so your providers can check for signs that cancer has spread. Those tests may include:
Healthcare providers may use surgery and anti-cancer medicines to treat regional IBC. This is cancer that hasn’t spread to other areas of your body. Your care team may use a step-by-step approach:
You may have other cancer treatments if IBC spreads to other areas of your body.
Your care team may also recommend that you take part in a clinical trial. A clinical trial is a study that evaluates the safety and effectiveness of new cancer treatments. Treatments that are successful in clinical trials often become the standard treatment approaches.
Advertisement
Inflammatory breast cancer can come back. Changes in the skin on your breast or swelling may mean you need additional treatment. Additionally, if you have any changes in your body that last two weeks or longer, you should let your doctor know.
The American Cancer Society lists two sets of IBC survival rates. One set is for regional IBC. The other set refers to distant IBC.
Regional IBC means the cancer has only metastasized (spread) to the breast and/or lymph nodes nearby. Distant IBC is breast cancer that has metastasized to other areas of your body, such as your bones, liver or lung. When it has spread to a distant part of your body, it is often stage 4.
According to the Cancer Society, 52% of women with IBC were alive five years after their diagnosis. That survival rate drops to 19% when cancer spreads to other areas of your body.
Cancer survival rates are estimates. These estimates come from information about other people’s experiences with IBC. What’s true for them may not be true for you. Ask your care team to explain what survival rate data means in your case.
Inflammatory breast cancer treatment can be exhausting and affect your appetite. Eating well can help combat cancer fatigue by boosting your energy levels. Regular gentle activity like walking, stretching or yoga may also ease exhaustion.
Advertisement
You may benefit from receiving palliative care if you’re having issues with cancer symptoms or treatment side effects. Palliative care focuses on managing cancer symptoms and treatment side effects.
If you have breasts, you’re probably familiar with the way they can change. Some changes are common. Your breasts may feel tender and swollen during pregnancy or when you menstruate.
But the changes that inflammatory breast cancer (IBC) causes are very different. Your breast skin may look bruised or discolored. It may be dimpled.
Talk to a healthcare provider if one of your breasts looks and feels different. Inflammatory breast cancer is very aggressive. It can get worse and spread within a few months. Your symptoms may not mean you have IBC. But if they do, prompt treatment may keep cancer from spreading. Your cancer care team will explain your treatment options. They’ll understand that it’s scary to learn you have a rare, aggressive cancer. Don’t hesitate to ask questions and share your concerns. Your team will take as much time as you need to help you understand your situation.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
A breast cancer diagnosis can turn your world upside down. At Cleveland Clinic, we offer expertise, compassion and personalized treatment plans.
