Castleman disease refers to a group of rare conditions that cause swelling and tissue changes in your lymph nodes. The two primary types are unicentric Castleman disease and multicentric Castleman disease. Symptoms, treatment options and prognosis vary depending on the type.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
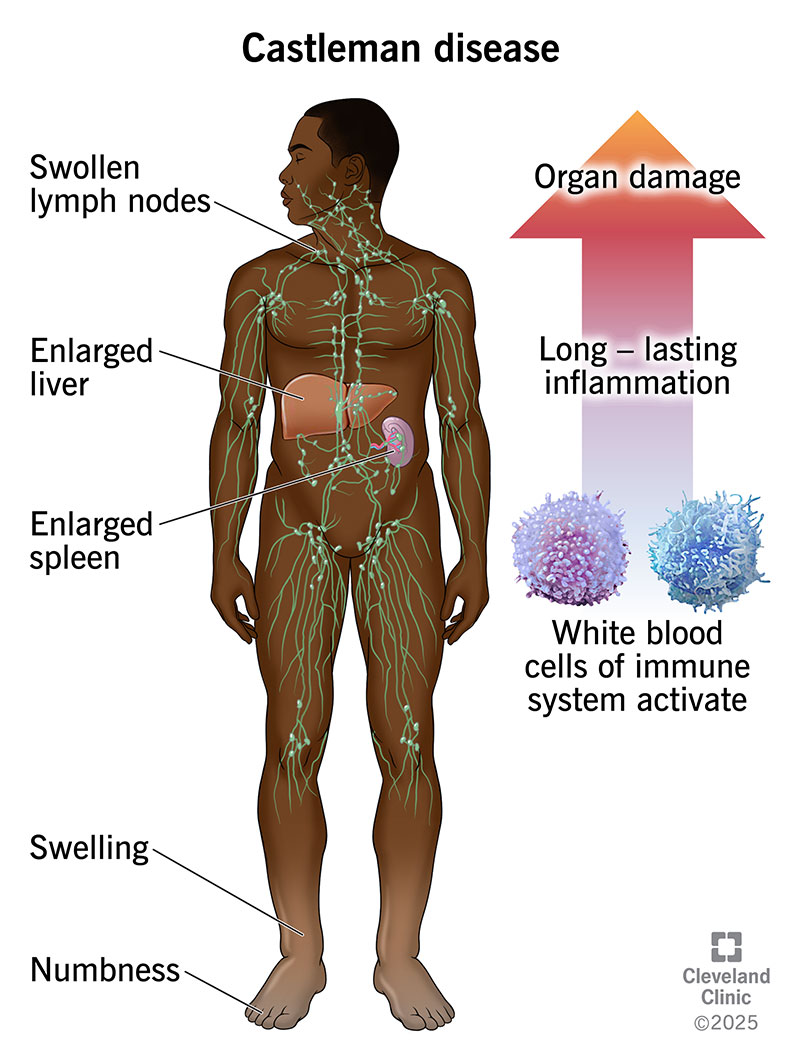
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/castleman-disease)
Castleman disease is a group of disorders that involve a hyperactive immune system. Typically, healthy immune systems activate to fight germs invading your body. Then, they settle down once the threat is gone. But if you have Castleman disease, your immune system remains activated. This leads to long-lasting inflammation that can damage organs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Meanwhile, your lymph nodes work overtime to filter germs and the immune cells that fight them. This causes an overgrowth of cells that leads to swollen lymph nodes. The lymph nodes don’t just get bigger. Castleman disease causes changes in the tissue of affected lymph nodes.
Castleman disease is rare. There are only about 4,300 to 5,200 new Castleman disease cases diagnosed in the U.S. each year. There’s still a lot that doctors are learning about this condition. In the meantime, treatment involves customizing the right therapies based on your unique diagnosis.
There are two main types of Castleman disease.
Unicentric Castleman disease (UCD) causes enlargement of one or more lymph nodes in one region of your body. About 3 in 4 cases of Castleman disease are UCD.
Multicentric Castleman disease (MCD) causes lymph node enlargement in many regions of your body. Healthcare providers classify MCD as:
Advertisement
There are three subtypes of iMCD:
Castleman disease symptoms vary depending on the type. You likely won’t have symptoms with unicentric Castleman disease. Enlarged lymph nodes may be the only sign. Sometimes, symptoms occur when an enlarged lymph node creates pressure on a nearby organ.
MCD is more likely to cause noticeable symptoms. In addition to enlarged lymph nodes, signs and symptoms include:
While the causes of unicentric Castleman disease (UCD) are unknown, an HHV-8 infection is associated with multicentric Castleman disease (MCD).
Scientists are researching potential causes of UCD and iMCD. These include infections other than HHV-8, gene mutations and autoimmune responses.
There aren’t any known risk factors for UCD or iMCD. You’re at increased risk of developing HHV-8-associated MCD if you have HIV or another condition that weakens your immune system.
People of any age can develop Castleman disease, but most people diagnosed are ages of 30 to 60.
Castleman disease increases your chances of developing cancer, including lymphoma.
Although it’s rare, people with UCD are at risk of developing a serious condition called paraneoplastic pemphigus (PNP). MCD can increase your risk of developing infections that can damage organs. The damage can be life-threatening without treatment.
Your healthcare provider will monitor your condition to prevent complications whenever possible.
Castleman disease symptoms are similar to those in other conditions, including common illnesses like the flu. Your healthcare provider may rule out these conditions first. Then, they’ll perform tests to diagnose Castleman disease and determine the type.
Advertisement
Tests and procedures may include:
Treatment for Castleman disease varies according to the type.
Surgery to remove the affected lymph nodes is the primary treatment for UCD. You may need radiation therapy or immunotherapy before surgery. These therapies shrink the growths on your lymph nodes, making them easier to remove.
If surgeons can’t remove the affected lymph node and you don’t have symptoms, your provider may monitor it instead of treating it. If surgery isn’t an option and you have symptoms, your provider may recommend treatments for MCD.
MCD is more difficult to treat than UCD. As it’s widespread, providers don’t typically use surgery or radiation to treat it. Instead, treatment depends on whether you have HHV-8 and how severe the disease is.
Advertisement
Your provider may use:
Call a healthcare provider if you find a lump in your neck, armpit or groin.
Reach out to your provider if you experience other symptoms of Castleman disease that don’t go away after a few weeks.
The prognosis (outlook) is good for most people with UCD. Removing the affected lymph node is often enough to cure it. With treatment, UCD doesn’t usually affect life expectancy.
The outlook for people with MCD depends on the type of MCD and how serious it is. Some people have intense symptom flare-ups that can be life-threatening. Others have more chronic symptoms. Sixty-five percent to 75% of people diagnosed with MCD are still alive five years later. With breakthrough therapies, there’s hope that the outlook will continue to improve.
Advertisement
There aren’t easy answers when it comes to Castleman disease. Your experience will depend on the type of Castleman disease you have. Additional conditions like HIV or associated disorders — like TAFRO and POEMS — will also shape your experience. In some cases, surgery and careful monitoring may be the only treatment needed. Or you may need many treatments throughout your lifetime to prevent complications. Ask your healthcare provider how your unique diagnosis will impact your treatment and outlook.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic provides expert, personalized treatment for Castleman disease using the most advanced therapies, from medications to surgery.
