Pyoderma gangrenosum is a skin condition linked to certain autoimmune diseases or an earlier skin injury. Medical experts aren’t sure of its causes, and it’s difficult to diagnose because it looks like other diseases. Medications and other treatment options can relieve your symptoms. Pyoderma gangrenosum may result in scarring.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
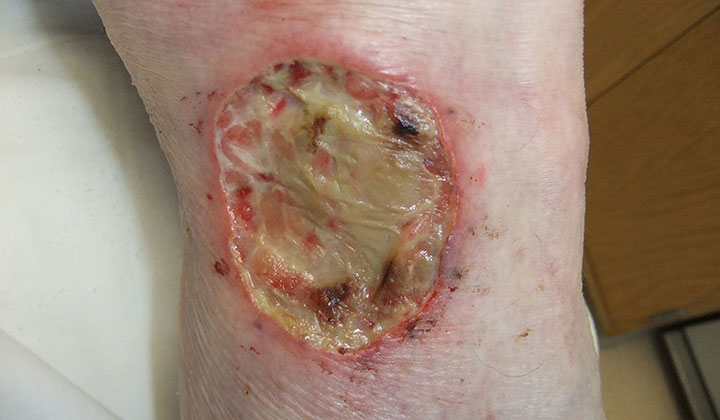
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17825-pyoderma-gangrenosum)
Pyoderma gangrenosum (pie-oh-der-muh gang-rah-no-sum) is a chronic, recurrent skin disorder in which small, discolored bumps or blisters (bullae) appear on your skin that can rapidly grow and join together to become large open sores (ulcers).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The number of ulcers can vary. Mild cases of pyoderma gangrenosum may only have one ulcer, while severe cases may have multiple or many. These ulcers can be painful.
There’s often a link between pyoderma gangrenosum and other systemic diseases.
Pyoderma gangrenosum affects people of all ages, though it’s rare in children. It most commonly affects women between the ages of 20 and 50. You may be more likely to develop pyoderma gangrenosum if you have:
Pyoderma gangrenosum isn’t common. Approximately 1 in every 100,000 people in the United States has pyoderma gangrenosum.
Pyoderma gangrenosum causes small, discolored bumps and inflammation on your skin. The bumps may be anywhere on your body, but they commonly appear on your lower extremities (legs, ankles and feet).
The bumps often rapidly open up (erode) your skin and expand to large, painful ulcers.
Studies show that up to 70% of people with pyoderma gangrenosum often have more than one illness or disease occurring at the same time (comorbidities). A combination of pyoderma gangrenosum and other systemic diseases — including rheumatoid arthritis, inflammatory bowel disease and blood disorders — may increase the likelihood of death by 30%.
Advertisement
Pyoderma gangrenosum may be an autoimmune disease. That means that pyoderma gangrenosum results from your immune system damaging tissue in your own body. For some people, pyoderma gangrenosum will improve after treatment for their other systemic diseases.
Pyoderma gangrenosum commonly affects your lower extremities. It may also appear on your arms, genitals and neck.
Symptoms of pyoderma gangrenosum include:
Your ulcers may be large and deep, and they can be very painful.
Medical experts don’t know exactly what causes pyoderma gangrenosum. More than half of people with pyoderma gangrenosum have other conditions, including rheumatoid arthritis, leukemia, lymphoma, ulcerative colitis and Crohn’s disease.
In addition, pyoderma gangrenosum often develops after an injury to your skin (pathergy), like trauma or surgery. Sometimes, pyoderma gangrenosum appears near a surgical opening (stoma site). This is peristomal pyoderma gangrenosum.
Pyoderma gangrenosum isn’t contagious. You can’t spread pyoderma gangrenosum to another person through skin-to-skin contact.
Pyoderma gangrenosum can be challenging to diagnose. No single test can confirm a diagnosis, so healthcare providers often order tests to rule out other possible causes of skin problems. These diseases include:
These tests may include:
There are many possible treatment options for pyoderma gangrenosum.
In mild cases, your healthcare provider may prescribe topical creams or ointments that you apply to your ulcers.
In more severe cases, your healthcare provider may prescribe oral medications that you take by mouth with water. Some studies indicate that newer, more targeted medications (biologic agents) may also help.
Surgically removing (debriding) dead tissue from your ulcers may be helpful in some cases. But it has risks, as injury to your skin can potentially make your pyoderma gangrenosum symptoms worse (pathergy).
Early diagnosis and treatment are important in preventing scars.
For early or mild cases of pyoderma gangrenosum, your healthcare provider may recommend:
Advertisement
For more severe cases of pyoderma gangrenosum, your healthcare may prescribe the following medications or treatments:
Trauma, including cuts, punctures and scrapes, can worsen your symptoms. Be careful to avoid any trauma that can cause more ulcers.
It’s also important to keep your wounds clean to prevent infection. Carefully wash your wounds with clean running water and soap. Then, carefully cover it with a nonadhesive bandage to prevent dirt or bacteria from entering the site. Ideally, your dermatologist will give you more in-depth instructions concerning how to keep your pyoderma gangrenosum clean and dressed.
Advertisement
If you have a prescribed topical medication, wash your wound with clean running water and soap. Apply the medication to your wound, and then cover it with a nonadhesive bandage.
For more severe ulcers, your healthcare provider may recommend covering them in a hydrocolloid bandage (dressing). These bandages protect your ulcers from further irritation or infection. After two to three days, they’ll “melt” into your skin.
Pyoderma gangrenosum is difficult to treat. Even with proper treatment, it may take weeks or even months to heal.
Pyoderma gangrenosum is difficult to diagnose, so it’s important to have realistic expectations. You may need to see several specialists and undergo many tests to rule out other conditions. This may delay proper treatment.
You may feel overwhelmed, stressed or depressed as you and your healthcare provider work to diagnose pyoderma gangrenosum and develop a treatment plan. Ask your healthcare provider for any tips or suggestions on keeping yourself as comfortable as possible during this time.
After a pyoderma gangrenosum diagnosis, it may take up to several months to heal. You may wish to seek out pyoderma gangrenosum support groups. They allow you to share your experiences and learn new ways to manage your symptoms.
Advertisement
The outlook for people with pyoderma gangrenosum depends on the severity. Severe forms of pyoderma gangrenosum, along with the presence of comorbidities, can result in severe pain, scarring and death.
If you have pyoderma gangrenosum, it’s important to discuss your diagnosis with any healthcare provider who’s considering a procedure that may damage your skin, such as surgery. They must consider if the procedure’s benefits outweigh the risks of triggering pyoderma gangrenosum. If you must have the procedure, they’ll need to closely supervise you to prevent any new ulcers from developing.
Medical experts aren’t sure exactly what causes pyoderma gangrenosum, so there may be no way to prevent it.
Pyoderma gangrenosum can advance quickly and leave permanent scars. If you have any risk factors associated with pyoderma gangrenosum, such as leukemia or inflammatory bowel disease, be sure to let your healthcare provider know right away if you develop any skin problems. Ask your healthcare provider to refer a dermatologist or another specialist with experience in treating pyoderma gangrenosum.
Contact your healthcare provider if:
Ecthyma gangrenosum is a rare skin infection typically caused by Pseudomonas bacteraemia found in water and soil. Ecthyma gangrenosum causes lesions that can kill surrounding tissue (necrosis). It most commonly affects people with a weak or damaged immune system (immunocompromised).
Like ecthyma gangrenosum, pyoderma gangrenosum also causes skin lesions. Medical experts aren’t sure what causes pyoderma gangrenosum. Autoimmune diseases may cause pyoderma gangrenosum, but pyoderma gangrenosum doesn’t primarily affect those who are immunocompromised.
There are four types of pyoderma gangrenosum ulcers:
Pyoderma gangrenosum causes small bumps on your skin that can quickly develop into large ulcers. This condition can be difficult to diagnose, and even after a diagnosis, it may take some time for your symptoms to heal. You’ll also have to be careful to avoid any trauma that may cause new ulcers to develop. Severe pyoderma gangrenosum or the presence of comorbidities along with pyoderma gangrenosum may affect your life expectancy. If you have an autoimmune disease and start developing sores that grow quickly, contact your healthcare provider right away.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
