Epidermolysis bullosa is a connective tissue disorder that causes your skin to blister and tear easily. Treatment helps prevent blisters from forming, care for blisters and skin, treat nutritional problems that arise from blisters in the mouth or esophagus and manage pain.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
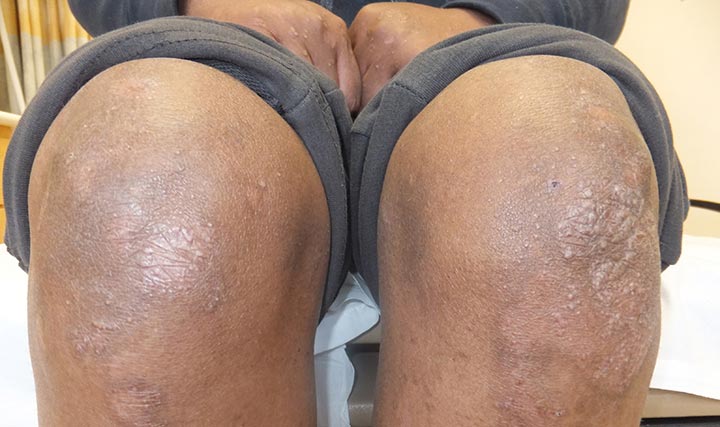
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17792-epidermolysis-bullosa-knees)
Epidermolysis bullosa (EB) is a group of genetic (inherited) disorders that causes your skin to be fragile and blister and tear easily. Blisters and sores form when clothing rubs against your skin, or you bump your skin. Mild cases of the disease usually cause painful blisters on the hands, elbows, knees and feet. However, tears and blisters can appear anywhere on the body. EB symptoms can range from very mild to very severe.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In some cases, blisters form inside the body in places such as the mouth, esophagus, other internal organs or eyes. When the blisters heal, they can cause painful scarring. In severe cases, blisters and scars can harm internal organs and tissue enough to be fatal.
EB has four primary subtypes:
Healthcare providers diagnose EBS, JEB and DEB according to your affected layers of skin. Kindler syndrome may appear as blisters throughout different layers of your skin.
EB affects everyone. People of all sexes, races and ethnic backgrounds can have EB. However, you’re more likely to have EB if you have a parent with the disorder.
Advertisement
An estimated 1 in 50,000 people in the United States have EB.
Severe cases of EB may cause blisters in your eyes, which can result in vision loss. It may result in severe scarring and deformities of your skin/muscles, making it difficult to move your fingers, hands, feet and joints. Some people with EB are at an increased risk of developing a type of skin cancer called squamous cell carcinoma. Death can sometimes occur during infancy due to severe infection (sepsis), breathing problems due to blocked airways, dehydration and malnutrition.
It depends on what type of EB you have. Mild cases of EB aren’t fatal. People with severe cases of EB have a life expectancy that ranges from infancy to 30 years of age.
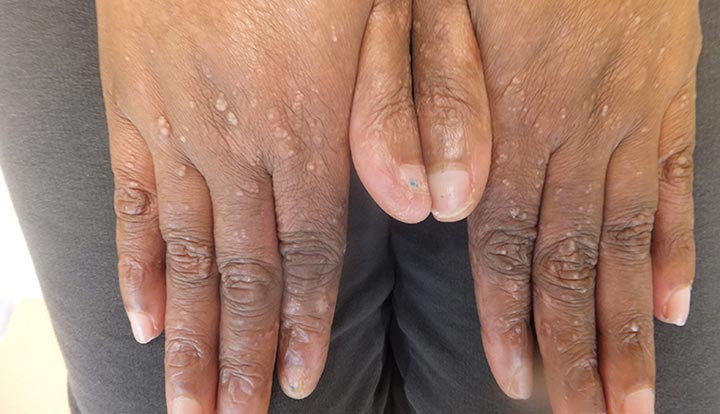
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17792-epidermolysis-bullosa-hands)
The signs and symptoms of EB depend on the type, and they usually appear when you’re a baby or toddler. Some symptoms overlap between the types. Symptoms of EB include:
A mutation (defect) in one of 18 genes causes EB. People with the disorder have a missing or damaged gene that affects a protein used to make collagen. Collagen gives connective tissues, like skin, their strength and structure. Because of this defect, the epidermis and dermis layers of your skin don’t bind together as they normally would. This results in skin that’s fragile and blisters and tears easily.
EB is usually an inherited disorder, which means that one parent may have it and pass it down to their children.
In rare cases, EB may also be an acquired autoimmune disorder.
EB isn’t contagious. It’s usually an inherited disorder.
Doctors diagnose EB with a test called a skin biopsy. In this test, a doctor removes a small skin sample and studies it under a microscope.
A genetic test can confirm the type of EB by identifying the defective gene. A prenatal genetic test can confirm if parents are at risk for having a baby with EB.
There is no cure for EB. Treatment helps:
To avoid damage and friction that may cause the skin to blister or tear, doctors recommend:
Advertisement
To treat blisters, your doctor may recommend:
To treat infections, your doctor may recommend:
To prevent nutrition problems due to difficulty eating because of blisters in the mouth or esophagus, your doctor may recommend:
For severe cases of EB, you may need surgery. Surgery will widen the esophagus (the tube leading from the mouth to the stomach) if blisters and scarring have caused it to narrow. Inserting a feeding tube directly into the stomach, bypassing the esophagus entirely, is another option for some people. Surgery also separates fingers or toes that have fused from the blisters.
Advertisement
The following tips will help you take care of yourself:
Your child’s needs are unique, and they may not yet have the ability or vocabulary to express what’s bothering them. The following tips will help make your child as comfortable as possible:
Advertisement
It may be difficult treating your child’s symptoms, and you may feel overwhelmed or stressed. Ask your healthcare provider about any other tips or suggestions on how to keep your child — and you — as comfortable as possible.
Parent support groups also allow you to share your experiences and learn new ways to manage your child’s EB.
The outlook for people with EB depends on the type and severity. Severe forms of the disease can result in severe pain, disfigurement, disability, wounds that never heal and early death.
Healthcare providers can help you manage symptoms with proper treatment and, if needed, medicines for pain management. Preventive measures — extensive every-other-day wrapping of the skin with nonadhesive, protective dressings — and regular bathing and wound care can help manage EB’s impact.
Because it’s genetic, you can’t prevent EB. People with a family history of EB who are thinking about becoming parents may benefit from genetic counseling to decide how to grow their families.
In addition, experts don’t currently know what causes EB acquisita. Therefore, healthcare providers don’t know how to prevent it.
Contact your healthcare provider if:
Bullous pemphigoid is a rare autoimmune skin disorder that may cause itchy, hive-like welts or fluid-filled blisters. Bullous pemphigoid occurs most often in people over the age of 60, and it usually goes away within five years. In severe cases, blisters and scars can harm internal organs and tissue enough to be fatal.
EB may be an autoimmune disorder, but a gene mutation that affects the collagen in your skin is typically the cause. EB usually occurs in infancy or early childhood. There is no cure for EB, so you may experience symptoms throughout your life.
Epidermolysis bullosa causes blisters, tears and sores on your skin, which may be mild or severe. The life expectancy for people with severe EB is poor. However, most people with EB continue to live well for decades after diagnosis, though they may have to take more precautions to protect their skin.
EB is usually an inherited disorder. If you have a family history of EB, it’s a good idea to see your healthcare provider to discuss genetic counseling to help you make family-planning decisions.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
