Bullous pemphigoid is a rare skin condition that causes blisters on your skin. It’s an autoimmune disease. Certain medications may trigger bullous pemphigoid, but healthcare providers aren’t sure exactly what causes it. It can be well-managed with medications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
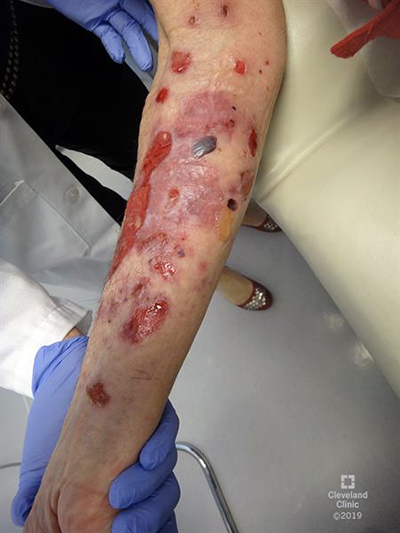
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15855-bullous-pemphigoid)
Bullous pemphigoid (bull-us pem-fuh-goyd) is a rare skin condition that causes itchy, hive-like welts or fluid-filled blisters.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It may affect a small area of your body or it may be widespread. Blisters may occur anywhere, but often develop on flexural areas of your skin, such as under your armpits (axilla), around your groin or on your stomach (abdomen). In some cases, blisters also form on mucous membranes, including your mouth, tongue, throat, esophagus and/or eyes.
Yes, bullous pemphigoid is an autoimmune disease. That means bullous pemphigoid occurs when your body’s immune system attacks the layer of tissue below your top layer of skin.
Bullous pemphigoid most commonly affects people over 60 years old, but it may also appear in younger people, too. It’s more common in the Western world, and uncommon in the Far East.
Bullous pemphigoid affects men and women equally.
You may be more likely to get bullous pemphigoid if you have a neurological disorder, including:
Bullous pemphigoid is relatively rare. There are between 2.4 and 23 cases per 1 million people in the general population. However, in people 80 years of age and older, there are between 190 and 312 cases per 1 million.
Bullous pemphigoid may be fatal if you’re in poor health or don’t seek treatment, especially if your blisters become infected.
Advertisement
Bullous pemphigoid appears as itchy welts that look like hives or multiple, itchy blisters (bullae). It most commonly appears on your:
The blisters typically appear along the creases of your skin. They usually aren’t painful, but they may break open and become a painful sore or ulcer.
The fluid inside of your blisters may be clear, or it may contain some blood. The skin around your blisters may look normal or discolored (red, purple, brown or slightly darker than your normal skin color).
Welts and blisters rarely result in scarring.
Bullous pemphigoid is an autoimmune disease. Healthcare providers and medical researchers aren’t sure why your immune system responds this way.
Certain medications may trigger bullous pemphigoid, including the diabetes medication alogliptin. Ultraviolet (UV) light and ionizing radiation may also trigger or aggravate bullous pemphigoid.
Healthcare providers and medical researchers aren’t sure if diet affects bullous pemphigoid. Some people have reported their bullous pemphigoid improved or went away after eliminating certain foods from their diet. However, there’s currently no good scientific evidence to support that certain foods trigger bullous pemphigoid.
If you have bullous pemphigoid, talk to your healthcare provider about any potential benefits of eliminating certain foods or drinks from your diet. They may recommend keeping track of what you eat and drink in a food journal. If you notice your bullous pemphigoid flares up after eating certain foods, gradually eliminate them from your diet to see if your symptoms improve.
No, bullous pemphigoid isn’t contagious. You can’t spread bullous pemphigoid to another person through skin-to-skin contact.
Your healthcare provider will examine your affected areas. They may ask you questions, including:
Your healthcare provider may recommend the following tests to confirm their diagnosis:
For mild cases of bullous pemphigoid, the best treatments are topical corticosteroid creams or ointments that you rub directly on the affected areas.
Advertisement
For moderate-to-severe cases of bullous pemphigoid, your healthcare provider may prescribe an oral corticosteroid, like prednisone, in addition to a steroid-sparing immunomodulatory agent such as dapsone, mycophenolate mofetil, azathioprine, methotrexate or chlorambucil.
If you can’t take can’t corticosteroids or other immunomodulatory agents, your healthcare provider may prescribe oral tetracycline or doxycycline pills.
For refractory cases of bullous pemphigoid, your healthcare provider may prescribe rituximab or IVIG infusions.
There aren’t any home remedies for bullous pemphigoid, but there are things you can do to make your symptoms more tolerable, including:
If you have bullous pemphigoid in your mouth, the following tips can make your symptoms more tolerable and help prevent nutrition problems:
Advertisement
You should start to feel better a few days after starting treatment.
Bullous pemphigoid usually clears up on its own after about five years. It generally responds well to appropriate treatment. You may have flare-up and times where it seems to go away (remission). During remission periods, you may stop your treatment.
If your blisters pop and become infected, you’re at risk of developing sepsis, which is a life-threatening condition.
Healthcare providers and medical researchers aren’t sure how to prevent bullous pemphigoid.
Contact your healthcare provider as soon as you develop unexplainable blisters.
Advertisement
Both bullous pemphigoid and pemphigus vulgaris are autoimmune blistering diseases. Pemphigus vulgaris symptoms share some similarities to bullous pemphigoid symptoms. Pemphigus vulgaris almost always starts on the mucous membranes inside of your mouth. Very few people have involvement of the skin. Also, the blisters in pemphigus vulgaris are much more fragile than those in bullous pemphigoid.
People with pemphigus vulgaris usually have erosions if their skin is involved, not intact blisters like bullous pemphigoid people typically develop. If you have pemphigus vulgaris, the top layers of your skin easily separate from your lower layers of skin with pressure, usually from pressing or rubbing (Nikolsky sign).
While all people with bullous pemphigoid have skin involvement, only about 33% of them develop blisters in their mouth.
Bullous pemphigoid is a rare autoimmune disease that causes blisters or sores on your skin. It may go away and come back, but it generally responds well to treatment and goes away completely after approximately five years. If you’re in poor health and your blisters pop and become infected, bullous pemphigoid may be fatal. Contact your healthcare provider right away if you notice blisters that you can’t explain.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
