Chronic venous insufficiency (CVI) happens when your leg veins become damaged and can’t work as they should. Normally, valves in your leg veins keep blood flowing back up to your heart. But CVI damages those valves, causing blood to pool in your legs. This increases pressure in your leg veins and causes symptoms like swelling and ulcers.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Chronic venous insufficiency (CVI) is a form of venous disease that occurs when veins in your legs are damaged. As a result, these veins can’t manage blood flow as well as they should, and it’s harder for blood in your legs to return to your heart. CVI causes blood to pool in your leg veins, leading to high pressure in those veins.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
CVI can happen due to damage in any of your leg veins. These include your:
CVI may cause mild symptoms at first. But over time, this condition may interfere with your quality of life and lead to serious complications.
Both terms refer to the same problem of damaged leg veins. Post-thrombotic syndrome is chronic venous insufficiency caused by deep vein thrombosis (DVT). DVT is a blood clot in a deep vein in your leg. “Post-thrombotic” means after a blood clot (which is also called a “thrombus”). After the blood clot is gone, it can leave scar tissue that damages your vein.
About 20% to 50% of people who’ve had DVT develop post-thrombotic syndrome, usually within one to two years.
Venous disease in general is very common. For example, varicose veins affect about 1 in 3 adults. Each year, about 1 in 50 adults with varicose veins go on to develop chronic venous insufficiency.
Chronic venous insufficiency usually affects people over age 50. The risk goes up the older you get.
Overall, chronic venous insufficiency affects about 1 in 20 adults.
Advertisement
Chronic venous insufficiency slows down blood flow from your legs back up to your heart. Without treatment, CVI raises the pressure in your leg veins so much that your tiniest blood vessels (capillaries) burst. When this happens, the skin in that area takes on a reddish-brown color and can easily break open if bumped or scratched.
These burst capillaries can cause:
Venous stasis ulcers don’t heal easily, and they can become infected. The infection could spread to nearby tissue. This condition is known as cellulitis, which is dangerous if not treated right away.
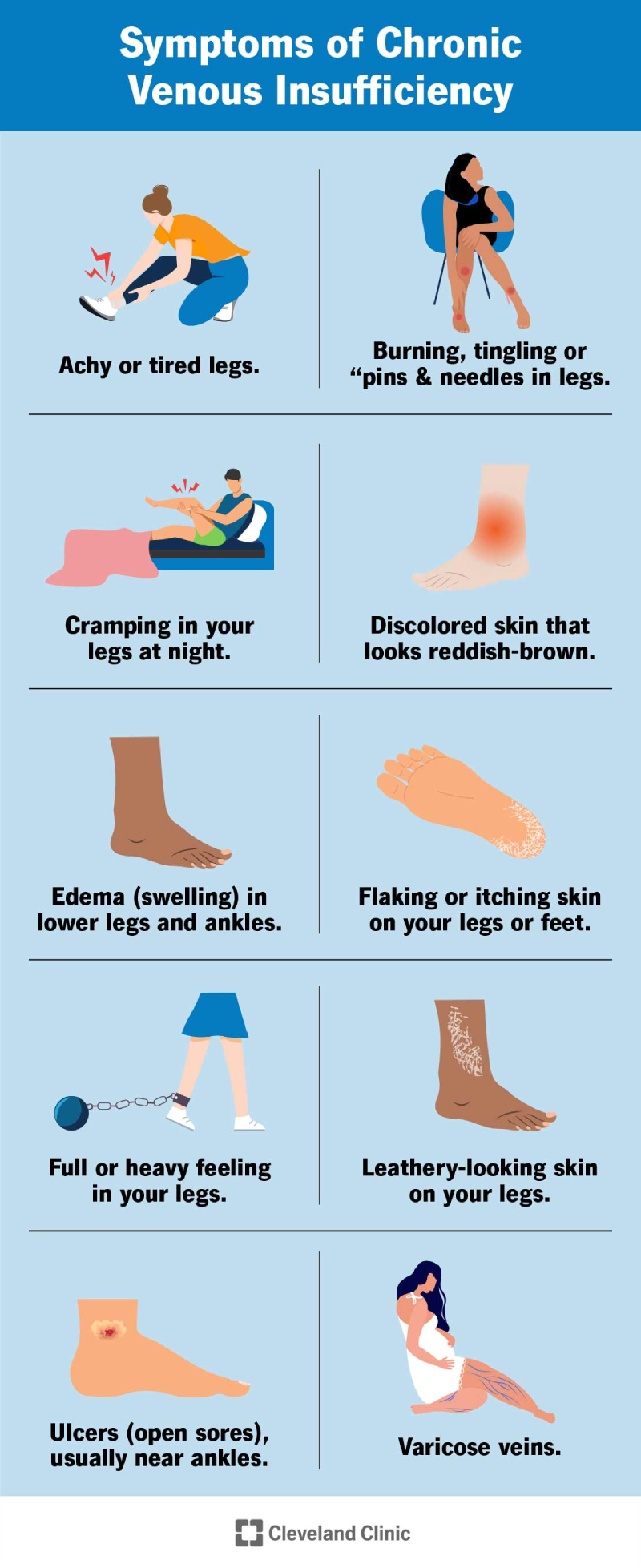
Chronic venous insufficiency signs and symptoms include:
Severe edema in your lower leg can cause scar tissue to develop. This scar tissue traps fluid in your tissues. Your calf may feel large and hard to the touch. When this happens, your skin is more vulnerable to persistent ulcers.
You may not have all of these issues at once. Instead, you may only have one or two. Your signs and symptoms depend on how far your condition has progressed.
The stages of venous disorders range from 0 to 6. “Venous disorders” is a general category for many possible issues with your veins, including CVI. The stages are based on clinical signs, which are things your provider can see or feel when they examine your legs.
Venous disorder stages include:
You’ll be diagnosed with chronic venous insufficiency if you’re at stage 3 or above. In other words, having varicose veins doesn’t mean you have CVI. But varicose veins are a sign of blood flow problems that could get worse over time. So, it’s important to tell your provider about any new varicose veins you notice.
Advertisement
Chronic venous insufficiency happens when the valves in your leg veins don’t work properly. Your leg veins contain valves that help your blood flow in the correct direction (toward your heart). If a valve becomes damaged, it can’t close properly. Gravity takes over, and blood struggles to flow upward toward your heart. It instead flows backward, a situation known as venous reflux.
Causes of valve malfunction may be congenital, primary or secondary.
Deep vein thrombosis (DVT) is the most common cause of chronic venous insufficiency. The blood clot damages the valve in your leg vein. People with a history of DVT face a higher risk of developing CVI.
Chronic venous insufficiency is diagnosed through a physical exam and ultrasound imaging. During the physical exam, your provider will:
Advertisement
Your provider will also rule out other medical conditions that could be causing your symptoms. This may involve other tests like an MRI.
Many people with CVI also have peripheral artery disease (PAD). So, your provider may ask questions or run tests to check you for PAD. If you have both CVI and PAD, your provider will advise you on treatment methods and precautions you need to take with compression therapy.
Treatment for chronic venous sufficiency involves lifestyle changes and compression therapy. If these measures aren’t enough, your provider may recommend a procedure or surgery. The best treatment for you depends on how far your condition has progressed and other medical conditions you have. Your provider will tailor treatment to your individual needs.
The goals of treatment are to:
Advertisement
Usually, providers recommend lifestyle changes as the first method of treatment for CVI. These include:
Providers commonly recommend compression therapy for treating CVI. Compression therapy helps ease swelling and discomfort in your legs.
There are many types of compression bandages and stockings. Some offer more compression than others. Very tight stockings require a prescription.
Some stockings are “graduated,” meaning they’re tighter down by your ankles and less tight further up your leg. It’s essential that you follow your provider’s guidance on the type of compression you need and when to use it.
Many people with CVI struggle to wear compression stockings over the long term. But compression therapy is very important to help your veins work better and ease your symptoms. If you struggle with compression therapy, talk with your provider. You may need a different type of stocking. Or, your provider may offer advice to make the treatment plan more doable for you.
If stockings don’t help, your provider may suggest intermittent pneumatic compression (IPC). IPC devices are inflatable sleeves you wear on your legs that help blood flow through your veins.
People who have peripheral artery disease (PAD) need to be careful with compression therapy. Your provider may caution you not to use it at all depending on the extent of your PAD. Closely follow your provider’s instructions.
Medications used to treat CVI include:
Nonsurgical treatments for CVI include:
Surgical treatments for CVI include:
CVI usually isn’t life-threatening and doesn’t result in amputation. But it’s a progressive disease that can cause discomfort, pain and reduced quality of life. Treatment can help manage your symptoms and give you a better quality of life.
Venous ulcers are difficult to treat, and they may return even after treatment. It’s important to keep all your medical appointments and closely follow your provider’s guidance.
Treatment can’t reverse the damage to your vein valves. But it can reverse your symptoms so that you feel better and have a better quality of life. Some procedures and surgeries can target and remove the damaged veins so that blood doesn’t flow through them anymore.
Similarly, chronic venous insufficiency can’t be cured. But you can manage the condition with lifestyle changes and other treatments your provider recommends.
If you have risk factors for CVI, you’re more likely than other people to develop the disease. Risk factors include:
Sometimes, CVI can’t be prevented. But you can lower your risk of CVI and other vein problems by making some lifestyle changes. These include:
If you’ve had DVT, your provider may recommend anticoagulants.
Your provider will tell you how to manage CVI at home. Some general tips include:
See your provider if you have any risk factors for chronic venous insufficiency. Your provider can assess your risk factors and help you lower them.
If you have CVI, keep all your medical appointments, and follow your provider’s guidance on when to return.
Call your provider if:
Call your local emergency number right away if you have symptoms of a pulmonary embolism. This is a life-threatening complication of deep vein thrombosis. It needs immediate medical attention.
There’s a lot to learn about chronic venous insufficiency. Don’t hesitate to ask your provider any question that comes to mind. You may also want to ask:
Vein problems are often more than just a cosmetic concern. Chronic venous insufficiency gets worse over time and can greatly interfere with your quality of life.
If you’ve been dealing with venous disease for a while, you’re probably frustrated and wish it would just go away. Luckily, there’s a lot you can do on your own to manage your symptoms and feel better. But sticking with the program is essential. Talk with your provider about strategies for keeping up a daily treatment plan and making compression therapy doable for you.
Vascular disease may affect your life in big and small ways. Cleveland Clinic’s specialists treat the many types of vascular disease so you can focus on living.

Last reviewed on 07/17/2022.
Learn more about the Health Library and our editorial process.