Atypical ductal hyperplasia occurs when you have abnormal cells in the milk ducts of your breast. These cells have a higher-than-normal chance of becoming cancerous. A breast biopsy diagnoses it. Your provider may recommend additional mammograms if you have atypical ductal hyperplasia.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
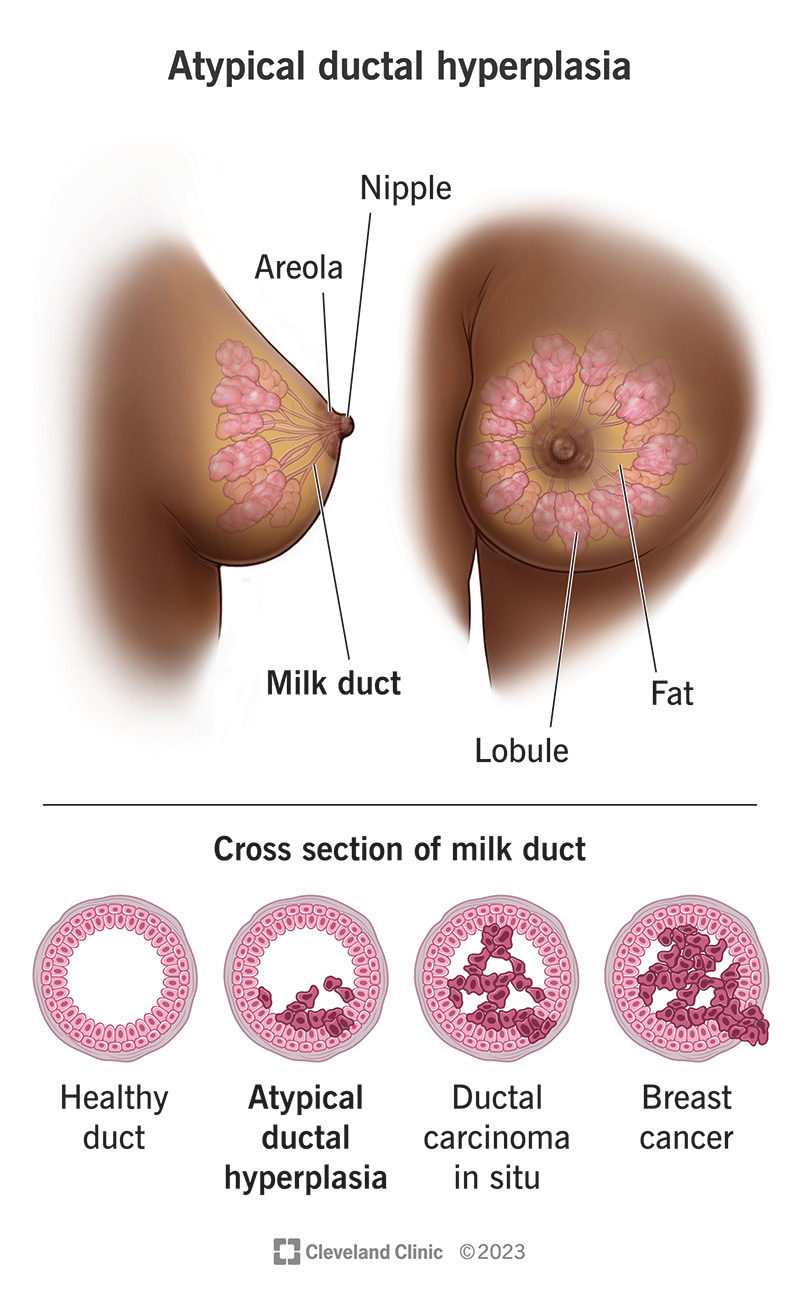
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/16242-atypical-ductal-hyperplasia.jpg)
Atypical ductal hyperplasia (ADH or atypia ductal hyperplasia) is when you have abnormal cells in the lining of the milk ducts in your breasts. Your milk ducts are small tubes that carry milk to your nipples. Typically, the cells in the lining of your milk duct appear lined up in two layers. With ADH, the cells are multi-layer and don’t line up. They appear disorganized or overgrown. The cells themselves are noncancerous (benign). But the cells share some features of ductal carcinoma in situ (DCIS), which is an early-stage breast (Stage 0) cancer. For that reason, ADH cells have a higher-than-average chance of changing into cancer.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your healthcare provider diagnoses ADH with a breast biopsy. A biopsy involves your provider removing tissue from your breast and sending it to a lab for analysis. Treatment for ADH involves more regular breast cancer screenings so that if cancer does occur, it’s found as early as possible.
Atypical hyperplasia is a general category that includes two types.
Hyperplasia is a term that describes abnormal cell growth. Sometimes, these cells appear normal under a microscope. But, when the cells are an irregular shape or size, a healthcare provider considers them atypical.
The two types are atypical ductal hyperplasia (ADH) and atypical lobular hyperplasia (ALH). ALH means that abnormal cells are in your breast lobule (the milk-making parts of your breast). ADH means abnormal cells are in the milk ducts (the tube that carries the milk to your nipple).
If your breast biopsy shows atypical ductal hyperplasia, it doesn’t mean that you have cancer. The cells are a marker for increased breast cancer risk. Studies have shown that people with either type of atypical hyperplasia may be up to four times more likely to get breast cancer compared to those who don’t.
A diagnosis of ADH usually means your healthcare provider will want you to have more breast cancer screenings such as mammograms, ultrasounds or breast MRIs (magnetic resonance imaging).
Advertisement
A healthcare provider may find atypical ductal hyperplasia (ADH) in between 5% to 20% of breast biopsies. It’s not cancer but increases your risk of breast cancer up to 20% or 30% depending on the types of irregular cells your provider sees, as well as other risk factors like genetics or having a personal or family history of cancer.
There are sometimes no symptoms of ADH. It’s a condition your healthcare provider may find during an examination or breast cancer screening. Some people develop lumps, pain or irregular nipple discharge which can alert them that something is wrong with their breasts.
Healthcare providers aren’t sure why the cells in your breast become irregular or why some people develop ADH. They do know that it increases your chance of developing breast cancer in the future. It’s best to talk to your healthcare provider to find out your risk for breast cancer.
Risk factors for ADH are similar to risk factors for breast cancer. But, many people develop breast cancer without any risk factors. These factors include:
The main complication of ADH is that it increases your risk for breast cancer. It’s important to follow your provider’s treatment plan, which typically involves annual mammograms or other breast cancer screenings.
Your healthcare provider finds ADH during a needle biopsy while investigating abnormal findings on a mammogram or ultrasound. A needle biopsy is a procedure that allows your provider to draw cells from your breast tissue. They may also find ADH while determining the cause of symptoms like a breast lump or nipple discharge.
Upon examining the cells from your milk ducts, your provider will notice the cells are distorted or stacked in multiple layers.
No, ADH isn’t cancer. It only increases your risk for breast cancer because the changes in the cells resemble changes in cells that do become cancer.
ADH itself isn’t cancer. It increases your risk for breast cancer in the future. A person with an atypical ductal hyperplasia diagnosis may not get breast cancer. Additionally, your breast cancer risk increases over time:
The treatment for ADH is a surgical (excisional) biopsy to remove more of the tissue that contains atypical ductal hyperplasia, plus the area immediately surrounding it. Your provider will send this tissue to a lab to make sure there isn’t cancer present. If your biopsy comes back normal, no further treatment is necessary. Your provider usually recommends more breast cancer screenings. If your risk of cancer is very high, they may prescribe medications to reduce your risk.
Advertisement
It’s worth noting that treatment for ADH is personal and unique to your situation. Only you and your provider can make decisions on the best treatment for you.
People with atypical ductal hyperplasia may benefit from taking a five-year course of certain preventive medications. These medications block estrogen and help decrease the risk of estrogen receptor-positive invasive breast cancer. The effects can remain for up to 15 years after taking them.
If you haven’t reached menopause, your provider may recommend tamoxifen (Nolvadex®). If you’ve reached menopause, your provider may prescribe:
All of these medications have some side effects. But the number of serious side effects is very low.
You’ll need to have a detailed discussion with your healthcare provider to determine if these medications are right for you. Although not a routine recommendation, your provider may recommend a risk-reducing mastectomy (removal of your breasts) if your risk is especially high.
Your healthcare will recommend annual breast cancer screenings and clinical breast exams (exams your provider performs) every six or 12 months. This ensures that if breast cancer were to develop, you can begin treatment as soon as possible. Treating breast cancer early leads to the best outcomes. Talk to your provider about what they recommend. You may qualify for an annual breast MRI based on your risk factors.
Advertisement
Most healthcare providers perform surgery to remove the entire area of tissue where the atypical cells were found. Providers find precancerous or cancerous cells in up to 20% of surgeries for ADH.
Your risk for breast cancer increases up to four times compared to someone without atypical hyperplasia. Other factors are involved in determining your overall risk. Be sure to discuss your risk with your healthcare provider.
It’s helpful to become familiar with your own breast tissue so you can identify changes. Learning how to perform self-breast checks at home is the best way to do this.
While you can’t prevent ADH, you can take steps to reduce your risk. Some of these steps include:
Follow your healthcare provider’s instructions for follow-up care. This involves attending all breast cancer screenings and making healthy lifestyle choices to reduce your risk. Lifestyle choices could include maintaining a healthy weight, exercising regularly and avoiding beverages containing alcohol.
Advertisement
ADH increases your risk for breast cancer but doesn’t necessarily mean you’ll get breast cancer. Talk to your healthcare provider about your risk of developing cancer in the future. Be sure to ask any questions you have about treatment.
Alerting your healthcare provider to any changes in the look or feel of your breast is important. Knowing what to look for is key to taking control of your breast health. Perform self-breast exams and attend annual examinations with your provider so they can find any changes early.
Contact your provider if you notice:
If you receive an atypical ductal hyperplasia diagnosis, you may want to ask your provider:
Having ADH can be stressful and cause worry since it increases your risk for breast cancer. Remember, an ADH diagnosis doesn’t mean you have breast cancer. It means your provider needs to watch you more closely. Be sure to follow your healthcare provider’s advice, including going to all your follow-up appointments and breast cancer screenings, and maintaining a healthy lifestyle. Talk to your provider about your overall risk for cancer and don’t be afraid to share your feelings with friends, family or others who can support you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
