Bunions happen when something puts extra pressure on your big toe and pushes it out of its natural alignment and toward your other toes. Visit a healthcare provider if you notice a bump at the base of your big toe. Treating bunions is usually a combination of wearing properly fitting shoes and treating any symptoms like pain and stiffness.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
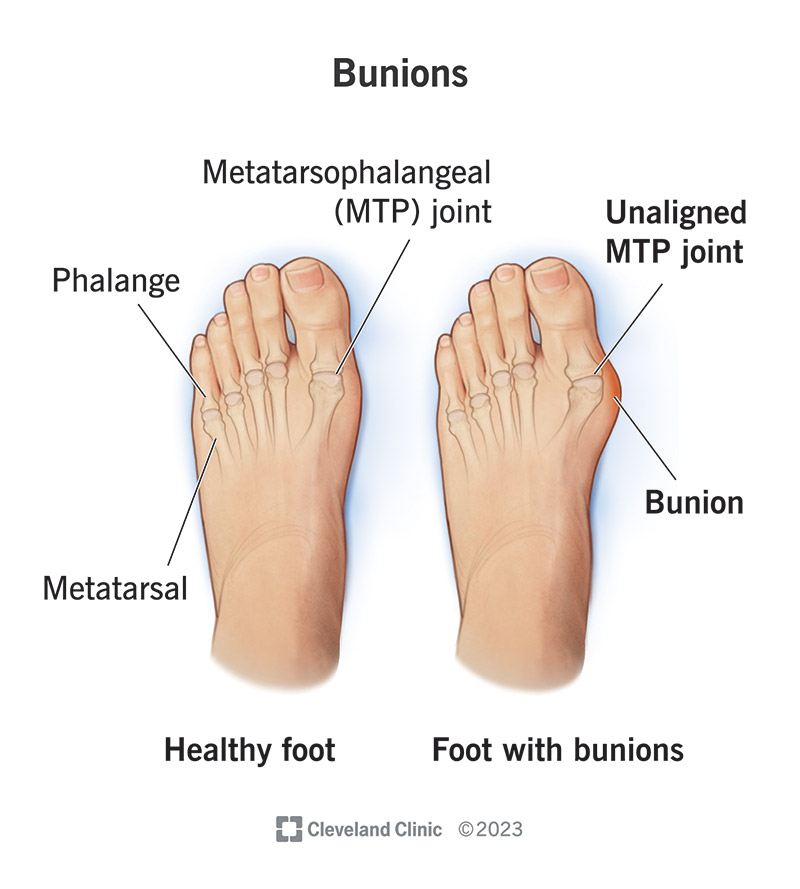
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/bunions)
A bunion is a bony bump that forms at the base of your big toe. Bunions develop on the inside edge of your big toe joint — the metatarsophalangeal (MTP) joint. The MTP joint is where the base of your big toe meets your foot. The medical term for bunions is hallux valgus.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Visit a healthcare provider if you notice a bump on your big toe, especially if you’re experiencing pain, stiffness or numbness in your toes or feet.
Bunions on your big toe from extra pressure are the most common, but they can form on other toes and for other reasons, too. Other types of bunions include:
Bunions are very common. Experts estimate that around one-third of Americans have bunions.
The most obvious symptom of a bunion is the growth that forms at the base of your big toe. You can usually see and feel the bony bump. A bunion can cause other symptoms, including:
Advertisement
There’s not just one reason why bunions develop. It’s thought that a combination of factors — like family history, abnormal bone structure, increased motion and shoe choice — can cause them. When something puts extra pressure on your big toe joint for a long time (usually years), that pressure can push your joint out of its natural alignment and toward your other toes. Eventually, a bunion forms on your MTP joint when your body compensates for your toe being pushed out of its usual place.
The most common causes of extra pressure on your big toe joint include:
Anyone can develop a bunion. Certain groups of people who are more likely to have bunions include:
Having a bunion may increase your risk of:
A healthcare provider will diagnose a bunion with a physical exam. They’ll examine your foot and ask about your symptoms. Tell your provider when you first noticed a bump near your big toe or if certain activities make your symptoms worse.
You might need to visit a podiatrist — a provider who specializes in caring for your feet.
You may not need any tests for your provider to diagnose a bunion. Your provider will use foot X-rays to determine the overall alignment of your bones and your MTP joint.
The most common bunion treatments include:
Advertisement
No, bunions don’t just go away and you can’t fix bunions on your own. See a healthcare provider or podiatrist if you have a bunion. They’ll diagnose it and suggest treatments to relieve your symptoms.
Most people with bunions are able to manage their symptoms with few long-term impacts to their daily routine. Your provider will work with you to find a combination of treatments to relieve your symptoms and keep your feet and toes healthy and strong.
Don’t wait to see a provider if you have bunion symptoms. The sooner you start treatment, the more likely it is you’ll be able to manage your symptoms without surgery.
People who need bunion surgery can usually resume all their usual activities in two to three months.
Since bunions are caused by a combination of several different reasons, they can be difficult to prevent. That being said, wearing well-fitting shoes may help reduce the progression of bunions. In general, follow these tips to find comfortable shoes that fit your feet properly:
Advertisement
Your provider or podiatrist can recommend types or brands of shoes that’ll work well for your feet. If you have other structural foot issues like flat feet or high arch feet, ask your provider whether you need orthotics to prevent bunions.
Visit a healthcare provider or podiatrist as soon as you notice any of the following symptoms:
Bunions are a common foot issue. They happen when something pushes your big toe out of its natural alignment and toward your other toes. Eventually, a bony bump can form on the joint where your big toe meets your foot.
Bunions need treatment if they cause pain. Even if it’s a simple solution like changing the kinds of shoes you’re wearing, you still need to see a healthcare provider or podiatrist to diagnose a bunion. Your provider will suggest treatments that’ll relieve your symptoms and help you get back to the activities you love.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Bunions can affect the way you move through your life. At Cleveland Clinic, we can work with you to create a treatment plan that’ll help relieve bunion discomfort.
