Toxic shock syndrome (TSS) is a rare but serious condition caused by certain strains of bacteria. It’s often associated with tampon use, but it can affect anyone. It causes toxins to spread into your bloodstream, causing severe organ damage or death. Knowing the signs of TSS and seeking prompt treatment results in the best outcomes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Toxic shock syndrome (TSS) is a rare but serious condition that happens when bacteria make toxins that get into your bloodstream.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You may hear about TSS most often when people talk about using tampons. But TSS can affect anyone. Skin wounds, surgical incisions, nasal packing or other areas of injured skin can all lead to TSS. You can get it when bacteria grow in a moist, warm environment (like your vagina). But bacteria can also enter your body through broken skin. These bacteria release toxins that eventually get into your blood. These toxins can damage organs, like your heart, liver or kidneys.
The symptoms of TSS happen suddenly and worsen quickly. But most people recover from it with a prompt diagnosis and treatment.
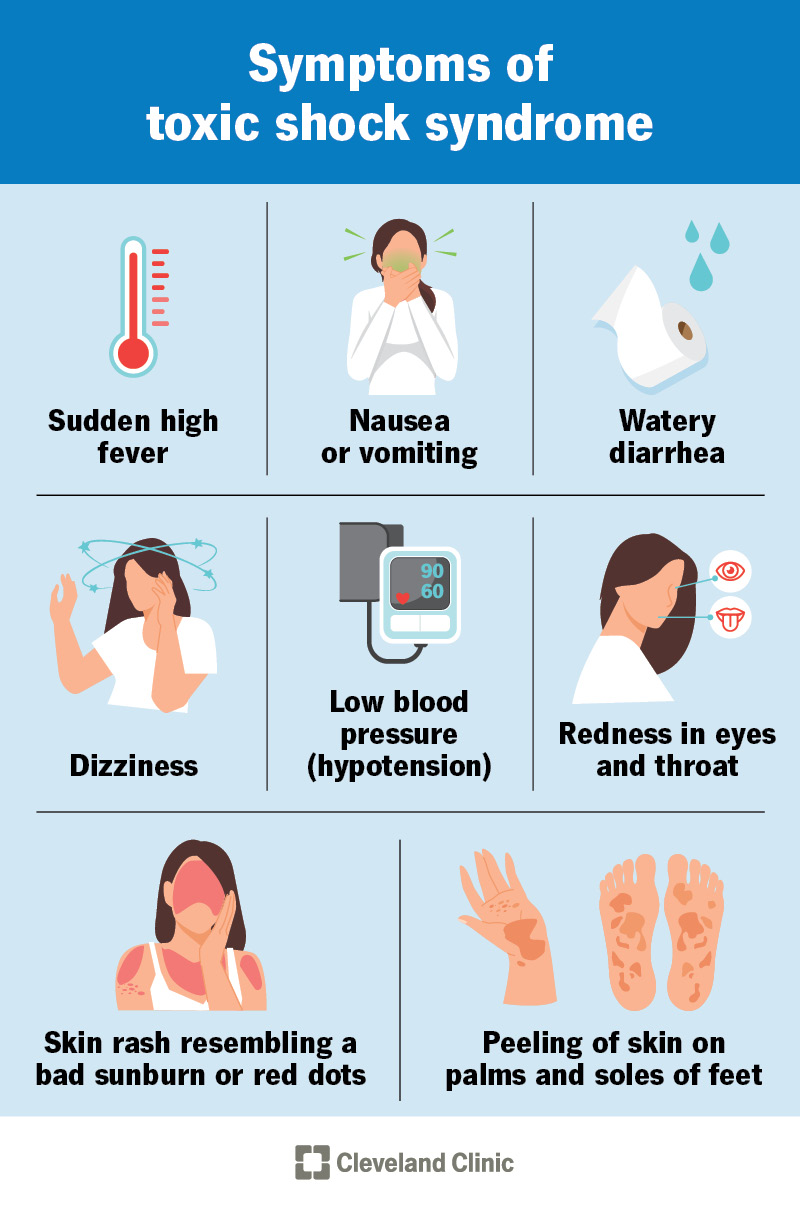
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15437-toxic-shock-syndrome)
Symptoms of toxic shock syndrome may vary depending on the type of bacteria producing the toxins. Symptoms may include:
Symptoms can begin within days of the toxins getting into your bloodstream.
A toxin produced by Staphylococcus aureus (staph infection) and Streptococcus pyogenes (group A strep infection) causes most cases of toxic shock syndrome. Clostridium sordellii can also cause toxic shock syndrome, but it’s less common.
Advertisement
These bacteria typically live on your skin or in your throat or mouth without causing any problems. Problems can happen when the bacteria are trapped in one area. This makes the bacteria grow quickly and spread. The bacteria can release toxins, which make you sick once they get into your bloodstream.
Tampons create an environment where bacteria grow, especially if they stay in too long. These bacteria can release toxins that enter your bloodstream.
Leaving a tampon in too long isn’t the only way to get TSS. Anything that stays in your vagina too long can increase your risk. This includes cervical caps, diaphragms or menstrual cups.
TSS can also happen when bacteria get into open wounds, cuts or sores on your body. This can be from a skin infection, surgery or a nosebleed that requires packed gauze to stop it. Anytime bacteria are close to your skin, they can multiply and produce toxins.
There isn’t an exact time. But you should remove a tampon after eight hours. This doesn’t mean you will get TSS if you leave it for longer. But leaving a tampon in too long gives harmful bacteria more time to grow.
Yes, you can still get toxic shock syndrome if you wear menstrual pads. It’s less common, but it can happen. This is because bacteria cause the condition, not the pad.
Most cases of toxic shock syndrome are linked to using tampons during your period. But TSS can happen to people who don’t use tampons. It can occur after surgery or from infections and skin wounds.
These factors can increase your risk:
Some steps you can take to lower your risk of TSS are:
Toxic shock syndrome is more likely to occur in people who’ve already had it. You should avoid using tampons during your period if you’ve recovered from a case of TSS.
Toxic shock syndrome is serious and life-threatening. Symptoms can progress quickly, and immediate treatment is necessary.
Advertisement
Shock, organ failure, amputation of limbs and death can occur if toxic shock syndrome is left untreated.
A healthcare provider may use a combination of exams and tests to check for bacteria. These include:
If your symptoms are severe or have progressed, your healthcare provider may order these tests to check the health of other organs:
Treatment usually happens in the hospital because the condition can be life-threatening. First, a healthcare provider will remove any tampons or contraceptive devices from your vagina if that’s the cause. You’ll get intravenous (IV) fluids and medications to raise your blood pressure if it’s low.
Treatment for the bacterial infection that causes TSS is antibiotics through an IV. This will help control the bacteria. But it will not stop the toxins from making you sick until your body clears them.
Other than antibiotics, other treatments for TSS may involve:
Advertisement
Contact your healthcare provider if you have signs of toxic shock syndrome, especially if you use tampons, have a skin wound or have recently had surgery.
Yes. While it can be serious, getting treatment right away improves your chances of making a full recovery.
Hearing about toxic shock syndrome (TSS) can feel scary. Many people think you can only get it from tampons, but this isn’t true. TSS can affect anyone, at any age. Symptoms often come on suddenly and can include flu-like symptoms, diarrhea and dizziness.
Using tampons is the most common way to get TSS, but it’s not the only way. The best thing you can do to protect yourself is to change tampons often and keep wounds and open cuts clean and dry. If you notice any symptoms of the condition, seek treatment right away.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
