Most burns happen because of something that’s too hot for you to handle. But burns can also happen when something’s too cold, with friction, chemicals and even from the sun. Knowing how to recognize and treat burns is important. And knowing when to get expert medical care for them can be lifesaving.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Burns are a type of injury that happens when something — usually something hot — damages tissues of your body. They’re more severe when they’re deeper and cover a larger part of your body’s surface area.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Burns are extremely common and usually unintentional. Worldwide, about 10 million people experience burns, and about 180,000 die from them each year. In the U.S., about 486,000 people receive medical care for burns each year.
There are five types of burns:
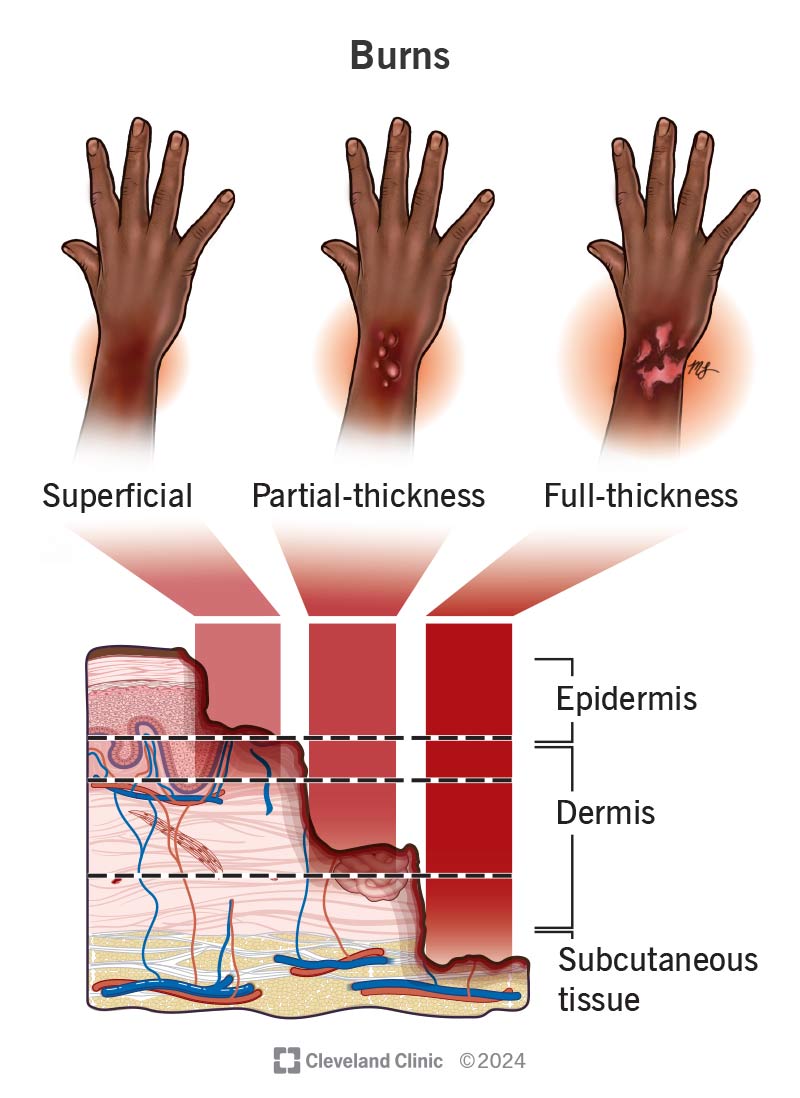
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/burns.jpg)
Burns can cause varying levels of damage to your skin, and are more severe the deeper the damage goes.
Experts determine how severe a burn is partly by how deep it goes. The older system of rating burns by degrees is no longer in widespread use. Instead, experts use the following system:
Advertisement
Burns can extend even deeper and damage muscles, nerves, bones and other deep tissues. These aren’t as common, and experts sometimes call these fourth-degree burns.
Common symptoms of burns include:
Burns can happen in many ways, including:
Burns can cause many complications, ranging from minor to life-threatening. Some of the most common complications include:
More severe complications can happen when burns are deeper and cover more of your body’s surface area. Some of these serious or dangerous complications can include:
Advertisement
The complications that are more likely in your case can vary depending on many factors. Your healthcare provider can tell you more about what to expect in your case.
A healthcare provider can diagnose burns by examining the injury and by asking questions about what happened. If you’re unable to answer, they may rely on input from first responders or others who were there.
Lab and imaging tests don’t usually help diagnose burns but can help catch complications before they become severe. Blood and urine tests are especially important for finding signs of organ damage or infections. And CT scans and magnetic resonance imaging may help detect deeper tissue damage in some cases, but these aren’t usually necessary.
Treating burns depends on how deep they go and how much of your body’s surface area they cover. Superficial burns are always minor and you can treat them yourself. When deciding how to treat a burn or if it needs medical care, remember the following Dos and Don’ts:
Do:
Advertisement
Don’t:
You can treat pain with over-the-counter medications like acetaminophen (Tylenol®) or ibuprofen (Advil® or Motrin®). Talk to a healthcare provider if you have any concerns about whether you can take these.
You always need professional medical care for partial-thickness burns that are too large to cover with your hand. You also always need professional care for all full-thickness burns.
Professional care can include the following treatments:
Advertisement
The treatments that might benefit you specifically can vary. Your healthcare provider can offer information tailored to your situation, preferences and needs.
What you can expect from a burn depends on how severe and large the burn is.
Many other factors can affect what you should expect from a burn and during your recovery. Your healthcare provider can tell you more about what to expect and the outlook for your specific case.
Yes, experts estimate that up to 90% of burns are preventable. Some key ways to prevent burns include:
Seek medical care if:
Call 911 or your local emergency services number, or seek immediate medical attention with the following:
Some questions you can ask your healthcare provider include:
Maybe your hand slipped while you were handling something hot in the kitchen, or you dropped a hot beverage and spilled some of it on yourself. Burns are painful and unpleasant, but you can do several things to aid your recovery.
The best thing you can do when it comes to burns is limit the complications they can cause. That means you shouldn’t hesitate to get medical care for burns that are deeper and larger. That way, you can recover and move forward with experience in preventing similar future burns.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Whether you need stitches, a broken bone set or think your appendix might be causing your abdominal pain, Cleveland Clinic’s emergency medicine team is here to help.
