Stereoelectroencephalography (SEEG) is a minimally invasive surgical procedure used to identify deep areas in your brain where difficult-to-treat epileptic seizures begin. Neurosurgeons most often use SEEG to determine if adults and children older than 2 with drug-resistant (refractory) epilepsy are eligible for surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
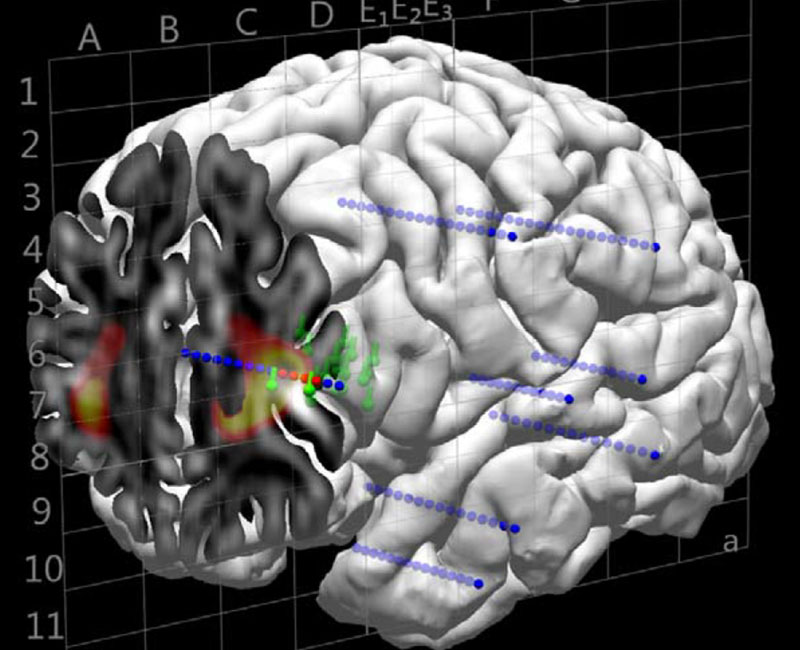
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/stereoelectroencephalography)
Stereoelectroencephalography (SEEG) is a minimally invasive surgery that can locate areas in your brain where difficult-to-treat epileptic seizures begin. Neurosurgeons place electrodes in deeper and more extensive areas of your brain than a regular electroencephalogram (EEG) can reach. After the surgeon places the electrodes, you stay in the hospital while an epilepsy team records your seizures.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
SEEG helps your epilepsy team figure out whether you can receive precisely targeted treatment, including surgery (resection) to remove brain cells that cause seizures. Your provider may also use SEEG during surgery or to guide other therapies for epilepsy.
Neurosurgeons most often use SEEG (also called stereotactic EEG) to figure out if adults and children older than 2 with drug-resistant (refractory) epilepsy are eligible for surgery. Refractory epilepsy doesn’t respond to at least two antiseizure medications or other medical treatments.
Your specialist may also use SEEG before you have brain surgery to map brain areas (sensory, motor and language) that need to be protected during surgery.
Or you may receive SEEG as part of treatment, like:
About 20% of people with complex focal epilepsy (seizures in one area of their brain) receive SEEG when the results of other tests, like MRI (magnetic resonance imaging), aren’t clear. If you have generalized epilepsy (seizures in multiple areas of your brain), you aren’t eligible for the procedure.
Advertisement
Your specialist may recommend this test if you:
The main differences are that SEEG:
During EEG, your provider attaches electrodes (small metal discs) to your skull to record electrical activity. An EEG is often more appropriate than SEEG for children and infants under age 2.
Typically, you’ll have EEG as a phase 1 test to determine where your seizures start. If results are unclear, or your neurosurgeon needs more information, they may recommend SEEG as phase 2.
Because SEEG records activity in areas on both sides (hemispheres) of your brain at different depths, your provider can more precisely identify (localize) where the seizures start. Children older than 2 can safely have the procedure.
In one study, people who received SEEG before epilepsy surgery spent a much shorter time in the operating room than those who had a specialized EEG, called subdural intracranial EEG, where electrodes were placed on the exposed surface of their brains. They also had a shorter hospital stay with SEEG and used fewer medications to control pain.
Your care team gives you instructions about how to prepare for SEEG. This usually involves other tests to see if you’re eligible for surgery. Your specialist may recommend:
You may worry that all or part of your hair, or your child’s hair, will be shaved. Or you may have questions about reducing or stopping your antiseizure medication before SEEG.
Discuss any concerns or questions with your care team before surgery. Your team works closely with you to ensure you and your child are as stress-free and comfortable as possible.
SEEG surgery usually lasts about four to six hours. On the day of your test, your anesthesiologist gives you medication. You’re asleep during the procedure and don’t feel any pain.
After you fall asleep, your surgical team:
Advertisement
After SEEG, you typically go to an Epilepsy Monitoring Unit. A team observes you for seizure activity. The electrodes are attached to equipment that records your brain activity. A computer then creates 3D images showing the start and spread of your seizures.
You may remain in the hospital for a few days to weeks based on how often you experience seizures. The average stay is one week. At the end of the testing, your team removes your electrodes in a simple process that takes about 10 to 15 minutes under local anesthesia.
SEEG is considered safe, but brain surgery has risks. These include:
Your care team will discuss with you when you can expect to feel better and get back to your usual activities. Typical recovery times are about 24 to 48 hours.
SEEG results depend on what your care team learns from the monitoring. In most cases, SEEG successfully locates the source of seizures. Specialists review your recorded brain activity and figure out if you can have surgery or other treatments for epilepsy. Surgery to treat epilepsy most often occurs four to eight weeks after SEEG, so you have time to recover.
You may receive early results before you leave the hospital. Before your treatment plan is set, you and your loved ones have time to review and discuss the final results with your care team.
Advertisement
When you can’t stop focal epilepsy seizures with medication, life can be challenging. You may be wondering what your options are. SEEG is a safe and often successful surgical procedure to locate the precise source of seizures in your brain. By providing detailed information, SEEG helps your specialists develop a treatment plan that may involve surgery. With effective therapy, your care team can help you reduce your seizures and embrace life.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Epilepsy and seizures can impact your life in challenging ways. Cleveland Clinic experts can help you manage them and find relief.
